Researchers discover the malignant cancer cells that cause metastatic deaths
The scientists believe that the identification of cells responsible for colon cancer relapse has the potential to change the treatment of the disease
Metastasis, the spread of a tumor to different parts of the body, is one of the biggest enemies of humanity: 90% of all cancer deaths are caused by this lethal dissemination of tumor cells. Now, an international team of scientists has found a possible weakness in the attacker: the group, led by Spanish biologist Eduard Batlle, spotted the malignant cells that are released from colon cancer, travel through the bloodstream and invade the liver. Colon cancer is the second deadliest tumor on the planet (only after lung cancer), with one million deaths per year. The finding was published recently in the journal Nature.
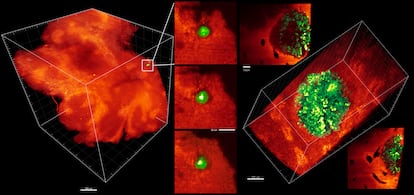
With traditional equipment, these malignant cells remained invisible until now, explains Batlle. His team developed a new method that is capable of capturing tiny metastases, of only three or four cells, in order to study them. “We are investigating whether this type of cell also exists in other tumors. In fact, these cells have genetic similarities with those of the most aggressive pancreatic cancer,” says Batlle, from the Institute of Biomedical Research of Barcelona.
The usual treatment for colorectal cancer consists of the removal of the affected area, followed by chemotherapy to prevent recurrence. However, approximately 35% of patients with an apparently localized tumor develop metastasis in the following years, with a mortality rate of over 85%. The cells that Batlle’s team identified and named High Relapse Cells remain hidden in other organs, like the liver or a lung, and produce these fatal secondary tumors. The biologist believes that their discovery has the potential to change the treatment of the disease.
Overall, cancer is no longer a death sentence. More than half of the patients survive. What’s more; in some types of tumors – leukaemias, lymphomas and myelomas – “miraculous” cures can be achieved in a few weeks thanks to the immunotherapy revolution, which uses the body’s own natural defenses to fight cancer cells. These treatments, however, do not usually work against colon cancer and its metastases, according to Batlle. The biologist’s studies in mice, on the other hand, do suggest that immunotherapy can be effective if applied at the right time.
In the colon, the primary tumor shields itself by forming a microenvironment with blood vessels and fibrous cellular material, which protects the cancer cells from the body’s defenses. “However, High Relapse Cells arrive naked in the liver or lungs. They still don’t have their tumor microenvironment. There is a window of opportunity for them to be noticed by the immune system,” says Batlle. In mice with localized tumors, the scientists injected standard immunotherapy to clean up residual detached cancer cells before removing the primary tumor. “These mice, after surgery, are cured. They never relapse, ever again,” celebrates the biologist. The effectiveness of this strategy in humans remains to be proven.
Independently, and without being aware of the existence of the High Relapse Cells, oncologist Myriam Chalabi started a clinical trial in 2017 to test early immunotherapy in people with colon tumors, at the Netherlands Cancer Institute. Her experiment uses a combination of drugs, including nivolumab, which releases the natural brakes on the body’s defenses, causing the immune system to unleash a ferocious attack on the tumor cells. Japanese researcher Tasuku Honjo, creator of nivolumab, won the Nobel Prize for Medicine in 2018; at the award ceremony, he declared that by 2050 cancer could be a chronic disease that in most cases does not cause death.
Batlle is also optimistic. “Approximately half a million colon cancer patients a year could be suitable for treatment with a therapy that prevents relapse,” he estimates. His team has identified 99 genes that are activated in patients that have up to five times greater risk of relapse after the usual treatment of surgery and chemotherapy. Those 99 genes can be found in the High Relapse Cells, which live on the periphery of the primary tumor until they detach themselves and form small clusters that colonize the liver or the lung through the blood. The researchers believe that their finding could also serve to identify the patients with a higher risk of metastasis.
The scientists at the Institute of Biomedical Research of Barcelona, led by Batlle and biotechnologist Adrià Cañellas, worked with colleagues from Spain and other countries, such as the geneticist Simon Leedham, from the University of Oxford (United Kingdom) and the oncologist Sabine Tejpar, from the Catholic University of Leuven (Belgium). And while Batlle’s team continues to investigate this promising line of research on its own, it is also watching closely for the results of the clinical trial in humans in the Netherlands. “We are expectant. We think that many patients are going to benefit from this,” says Batlle.








































