US aid cuts collapse Malawi’s LGBTQ+ health services as volunteers scramble to fill the void
The lack of funding has left some 15,000 users of NGO programs scrambling for care in a public system that many fear to enter
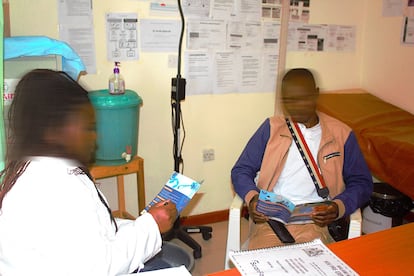
At the central hospital in Mzuzu, in a crowded corridor, a nurse shouted at Chisomo Nkwanga. The 24-year-old had come to the public hospital for the first time to collect his life-saving HIV medication, the same medication he had received with dignity at the donor-funded clinic in his city until it closed its doors in January 2025.
He had been waiting in line when he fell into an argument with one of the nurses. “You are gay, and now you are starting to patronize our hospitals because the whites who supported your behavior have left?” she said, loudly enough for the corridor to hear.
Too humiliated to respond, he left the hospital that day without his antiretroviral medication. At the local drop-in center in Mzuzu, people knew his name and greeted him when he arrived. He was treated, he said, as “a patient, not a pariah.”
Nkwanga learned he was HIV-positive six years ago after he began falling sick frequently. In the years since, the condition has left him thin and pale. “I am a living dead,” he says.
Same-sex relationships are illegal in Malawi. In 2010, Steven Monjeza and Tiwonge Chimbalanga, the first gay couple to marry in the country, were sentenced to 14 years in prison for “gross indecency and unnatural acts.” They were later pardoned during a visit by then-U.N. secretary general Ban Ki-moon, but a government minister told the BBC the men could be re-arrested if they continued their relationship. That legal climate is the backdrop against which U.S. tax dollars built a parallel health universe where LGBTQ+ people could seek care without fear of arrest or assault.
When the United States froze funding for the President’s Emergency Plan for AIDS Relief (PEPFAR), the global HIV initiative launched in 2003 and widely hailed as one of the most successful humanitarian programs in history, several health programs across Malawi shut down almost overnight. The cuts left at least 15,000 LGBTQ+ people registered in programs — run by organizations such as the Center for People Development (CEDEP), the Nyasa Rainbow Alliance, and Art & Global Health Center Africa (ArtGlo) — scrambling for care in a public health system many fear to enter.
“Everything stopped at once”
Organizations like the CEDEP and the Nyasa Rainbow Alliance had operated drop-in centers that functioned as community hubs offering HIV testing, PrEP, and mental health support.
“When the stop-work order came all 1,921 PrEP [pre-exposure prophylaxis] clients lost structured service delivery overnight, refills, counselling, peer follow-up, everything stopped at once,” says Gift Trapence, CEDEP’s executive director. “We were providing continuity, follow-up, mental health support…a whole ecosystem designed specifically for key populations.”
George Kachimanga, program manager for the Nyasa Rainbow Alliance, explains that most of these clinics — such as those serving the cities of Mzuzu and Mangochi — are still closed. “Only a few are still operating. For example, CEDEP runs two urgent care centers in Blantyre and Lilongwe using its own funds,” he says. “And since the funding freeze, none of the programs supporting the LGBTQ+ community in Malawi have resumed.”
“Now there is hope, as some European Union countries have shown interest in funding the work through other agencies such as the United Nations Development Programme [UNDP],” he continues. “We hope that something substantial will emerge by the end of this year. The only fear is that the current conflict between the U.S., Israel, and Iran will have knock-on effects, impacting budget decisions and so on. I hope it doesn’t come to that.”
Some CEDEP volunteers like Yamikani Samala have tried to hold the line. He once served more than 200 clients through CEDEP’s outreach clinics. Now, each morning, he moves door to door, checking on clients who have missed appointments, collecting health passports so he can queue on their behalf, and paying transport from his own pocket.
“When someone tells you they haven’t taken their medication because they were afraid to go to the clinic, it stays with you,” he says. “These are not statistics. These are people I know by name.”
Not enough
But individual effort cannot replace an entire system. Kachimanga estimates that between 2,300 and 2,500 of the roughly 3,000 clients his organization once supported have lost effective access to prevention services. Only 500 to 700 have managed to remain engaged in public facilities. His organization estimates that while clients were “administratively” transferred to government hospitals, as many as 80 to 90% have stopped showing up.
“For many of our clients, continuity, safety, and confidentiality remain extremely difficult in routine public facilities,” Kachimanga tells EL PAÍS.
According to a CEDEP report, another group of transgender women reported being publicly “outed” and harassed at a local bar by a health worker who had previously seen them at a clinic.
The human cost surfaced most starkly in Lilongwe, where a young LGBTQ+ client died after losing structured support. The individual had no parents and had been forced to return to what Kachimanga described as a “homophobic community,” a rural village where hostility made open care-seeking dangerous.
“We tried as organisations, even individuals tried to support,” says Kachimanga. “But the situation got worse. We lost the person.”
But on the ground, the transition has been challenging. Thandi, a transgender woman and sex worker, used to rely on a drop-in center for her healthcare. Since its closure, the gaps have been immediate. At public hospitals, she is permitted only 10 condoms per month. She says she chooses to buy condoms when she has the money or asks her clients to bring their own. “I can’t afford to risk my health or that of my clients,” she says. “I have to be creative, but it’s not a sustainable solution.”
Rodgers Phiri, executive director of Art & Global Health Center Africa, which had trained health providers, magistrates, and police officers as institutional champions of inclusive care, says the informal systems his organization built have collapsed since the withdrawal of funding. Most alarming are reports of clients sharing antiretroviral drugs after losing adherence support.
“Because ARV regimens [the specific combination of antiretrovirals a person should take] differ, for example, someone on a 13A regimen should not be taking a different combination, it is dangerous to substitute a friend’s medication without clinical guidance,” he says. “This risks treatment failure and drug resistance.”
Long-term consequences
According to UNAIDS data, more than 4,500 health workers nationwide, including 247 nurses and 1,600 diagnostic assistants, have lost their jobs as U.S. funding dried up. Many focused on bridging gaps between formal clinics and marginalized communities. Maziko Matemba, an independent public health expert, contends that much of the risk lies in the unravelling of targeted interventions.
“Programs providing pre-exposure prophylaxis, anti-retroviral therapy adherence support and stigma-reduction initiatives were designed specifically for marginalized communities whose interaction with the health system is often shaped by fear and discrimination,” he says.
Studies, including Malawi’s stigma index, have consistently shown high levels of social hostility toward LGBTQ+ people, making specialized outreach indispensable. Without dedicated funding streams, Matemba warns, prevention efforts risk reverting to “generic models that fail to reach those most vulnerable.”
“If indeed we don’t have resources,” he adds, “we are putting these groups at greater risk. We might see increased HIV incidence in the next few years. HIV can only be contained in these groups if they are reached.”
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition







































