In Spain, Covid hospital admissions nearly triple in a month
The rise in coronavirus cases is putting pressure on the country’s healthcare system, but the situation remains under control thanks to the vaccination drive. Primary centers, however, warn they are already overwhelmed
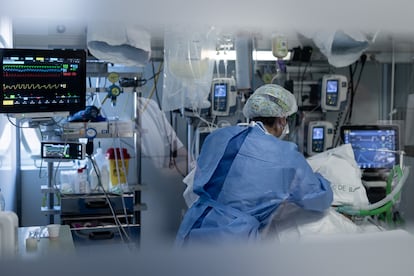

Spain’s healthcare centers are holding their breath given the rise of the sixth wave of the coronavirus pandemic in the country. Hospital and intensive care unit (ICU) admissions due to Covid-19 have nearly tripled in the last month: there are currently 6,667 people hospitalized and 1,306 ICU patients. Healthcare professionals are looking to the coming weeks with “concern.”
With nearly 80% of Spanish citizens fully vaccinated against the disease, this mass vaccination is working as a barrier that will avoid the complete overload of the system and hospital occupation levels are below those registered in other months of 2021. But some centers are already overwhelmed and the short-term outlook is far from hopeful: healthcare professionals are expecting more pressure on hospitals and the primary healthcare system due to the spread of the omicron variant, the effects of social interaction after Christmas, and the combination of the coronavirus and flu season.
“Everything is rising and given that there are no major restrictions in place the expectation is that they will continue to rise,” explains Álvaro Castellanos, the president of the Spanish Society of Intensive Medicine.
The European Center for Disease Prevention and Control (ECDC) has already sounded the alarm, and has called on hospitals to prepare for a possible explosion of cases. “It is therefore considered very likely that the Omicron VOC [variant of concern] will cause additional hospitalizations and fatalities, in addition to those already expected in previous forecasts that only take into account the Delta VOC,” reads the latest risk report published by the ECDC.
The situation seen in Spain so far is not like that of other waves, however. At this point last year, with an incidence of 207 cases per 100,000 inhabitants, there were more than 11,300 patients in the country’s hospitals, with nearly 2,000 in the ICU. This Friday, however, the infection rate was more than double, with 511 cases per 100,000 inhabitants, and hospitalizations were 41% down: 6,667 coronavirus patients, according to the latest data from the Health Ministry.
But this wave is still rising and the situation varies from region to region. In fact, there are half a dozen regions with hospital occupation that is similar to or above the peak of their fifth wave, and there are several, such as the Basque Country, Asturias and Valencia, whose ICU occupation is at the level of the peak during the previous wave.
Meanwhile, the capacity of primary healthcare centers is being put to the test and they are permanently overloaded, but they are not overwhelmed as they were during the fifth wave. For example, in Aragón, 4,300 contacts of cases are being monitored via the primary healthcare system, but last summer this number was as high as 18,500 and in October 2020, it was 24,300.
The pressure on all levels of the healthcare system is growing, however, and staff are already starting to complain of overload. José Díez Manglano, the president of the Spanish Society of Internal Medicine and a doctor at the Royo Villanova Hospital in Zaragoza, explains: “The number of cases in my hospital has quadrupled in the last 15 days,” he says. “This is not a situation where we are overwhelmed, but it is of concern.”
Pere Domingo, the Covid coordinator at the Sant Pau Hospital in Barcelona, agrees. “Last Friday [December 10], given that things looked bad, some surgeries were suspended, but in the end, the weekend was calmer than expected. We have 25 Covid patients on the normal ward and a dozen or so in the ICU.” This is compared to 450 and 100, respectively, during the first wave. “If this doesn’t get worse, we can handle it. The problem is if this is an omen of what’s to come.”
We are tired, we have no support, no reinforcements. We are always lagging behind the pandemicMaría Fernández, spokesperson for the Spanish Society of Family and Community Medicine
Nine regions are already above 15% of ICU occupation with Covid patients. There are even some with an excess of 20%. According to Castellanos, of most concern is Catalonia, where a quarter of its ICU beds is already full (338 people). María José Abadías, a deputy director at Vall d’Hebron, Catalonia’s biggest hospital, says that hospitalization is “growing slowly” and that the situation is still under control. Last week there were 20 or so patients in a critical condition, much fewer than the 220 who they had to treat at once during the first wave.
Sonia García de San José, the deputy manager of the Gregorio Marañón Hospital in Madrid, also points to the situation being under control, but says they have a “wait and see” approach. “We are seeing a rise in the pressure on the emergency room, with around 600 patients a day, which is 50 to 80 more than usual. And the percentage of positive Covid tests has gone from 7% to 26% in a week. But the symptoms that we are seeing are milder,” she explains. They have not yet had to reschedule surgeries nor activate new Covid wards.
The most common Covid patients in this sixth wave, both in the ICU and on the wards, are twofold according to the experts consulted by EL PAÍS. They are the unvaccinated and older people with existing conditions, such as suppressed immune systems or chronic pathologies and who were vaccinated some time ago now. The protection offered by the Covid-19 vaccines wanes as the months pass, Castellano explains. “Now we are seeing that 60% are vaccinated: the virus is affecting immunocompromised patients more and the protective effect of the vaccine falls.”
The expert points to the fact that the average age of those in the ICU is between 60 and 63. On the ward, Díez Manglano adds, there are also people mostly aged between 50 and 70. “There are older people who are fully vaccinated or who have also had their third shot, and there are also people who are 15 years younger and who are not vaccinated or don’t have the two doses.” The internist insists that despite the fact that some people are being admitted who have been fully vaccinated, hospitals are seeing “a contained spike thanks to the vaccines.” He continues: “Any vaccine helps to prevent the illness, but they don’t have a 100% effectiveness. In seniors, just as the body ages, so does the immune system. This generates fewer antibodies and a lower response to the vaccine.” Even so, Díez Manglano adds, “these vaccinated people who are being admitted arrive with less-severe symptoms than those who were being admitted a year ago.”
Contingency plans have still not been put into action in healthcare centers, but some hospitals have already had to take measures in Spain. For example, in the San Jorge de Huesca hospital, specific beds have been made available for patients with Covid-19 and in Vigo, non-urgent surgeries have been rescheduled. In the Basque Country, the number of ICU beds has been increased since the end of November and the surgery schedule has been limited. In the Valdecilla Hospital in Santander, a new Covid ICU has been opened and this week saw two surgeries closed.
In Navarre, where the global hospital occupation is around 79% (including Covid-, non-Covid and ordinary recovery), the fifth floor of the Navarre University hospital has been reconverted in order to treat Covid-19 patients. Home care has also been bolstered and some non-urgent surgeries have been canceled.
Meanwhile, there are complaints from the primary healthcare system of overload – these centers are having to attend to regular patients, manage the vaccination campaign, and detect and monitor new coronavirus cases and their contacts.
Everything is rising and given that there are no major restrictions in place the expectation is that they will continue to riseÁlvaro Castellanos, president of the Spanish Society of Intensive Medicine
The president of the Galician Association of Family and Community Medicine, Susana Aldeoa, warns: “In Ourense, primary healthcare is overloaded like never before in this pandemic.” Primary healthcare staff too are also suffering infections once more, explains Aldecoa, because triage circuits for patients have been relaxed and they now enter for consults without first going through a control for Covid symptoms.
María Fernández, a doctor in Madrid and spokesperson for the Spanish Society of Family and Community Medicine, expresses the same fears. “There is still a tense calm in hospitals because we are the antechamber, but we are already up to our eyes.” The doctor warns that in-person and telephone appointments are all booked up, the nurses can’t keep up and that they are drowning in bureaucracy. “We are tired, we have no support, no reinforcements,” she complains. “We are always lagging behind the pandemic, there’s no proactivity.”
Across the country, it’s the same story in the primary healthcare system. A doctor at a healthcare center in Mallorca, who prefers to remain anonymous, explains that they can’t keep up. “Now we have to deal with the suspicion of Covid with people who come due to other conditions and bring with them a list of problems they’ve had for a while,” she explains. “This is a crazy situation.” What’s more, there are staff shortages. “In my center, for example, there are three colleagues missing and I have 30 patients to see, plus the emergency cases from my quota, plus my colleagues’ patients, who those who are left have to see because there are no substitutes.” They are at capacity, she insists. “We are tired, burnt out and we feel abandoned,” she complains. “We no longer have the fear of the first waves, but psychologically and physically we are exhausted.”
Healthcare centers are waiting to see what the coming weeks bring. The uncertainty caused by some epidemiological variables is preventing them from predicting what will happen, the experts consulted by EL PAÍS admit. For example, Clara Prats, a researcher in Computational Biology at the Polytechnic University of Catalonia, warns that “the progress of ICU occupation in Catalonia is moving toward the upper levels of the forecasts and that is worrying.” The physicist, who is an expert in predicting the behavior of the pandemic, is observing the omicron variant with unease. “If it was a delta wave, between the third dose and some minor measures, it could be properly controlled. But what we’re seeing with the omicron variant, which appears to be up to two or three times more infectious than delta, is a change of the scenario from day to day. It’s as if you’ve suddenly hit a switch. The severity would have to fall a great deal to compensate the overload that could be caused by this high transmission.”
Also of concern is the effect that flu season could have. Last year, there were barely any cases of this seasonal virus, but now they are being detected, Abadías explains. “Covid is now letting other viruses in,” she explains. “We have already admitted some flu patients and we have already had a lot of pressure in the pediatric ICUs due to respiratory syncytial virus,” i.e. the microorganism that causes the majority of bronchiolitis cases among children.
Health professionals are calling on people to maintain individual protection measures in order to combat Covid and other respiratory viruses, but also to accelerate vaccination against the disease among children and administer the third dose to risk groups in order to cut transmission and avoid new hospital admissions.
In a scenario of increasing pressure, the experts agree that healthcare centers are more flexible than at the start of the pandemic to adapt their resources to the needs of the moment. They can, for example, set up or take down beds in just a few hours. They can also activate entire wards. But they warn that if they are overloaded once more, this will have a knock-on effect on the population, which will see their ability to be seen for non-Covid conditions affected, and on healthcare professionals. Domingo explains that they are “better prepared,” but “more tired.” Above all seeing what is coming, he explains. “We are somewhere between fear and weariness.”







































