Spain’s primary healthcare centers struggling to cope with strain of pandemic
With more work but no new resources, doctors and nurses say they are “exhausted,” with many at risk of mental illness or on leave for post-traumatic stress


The coronavirus pandemic has pushed Spain’s primary healthcare workers to the breaking point. When describing their situation, the words they use are “overwhelmed,” “disheartened” and “exhausted.” In the first wave of the pandemic, primary healthcare workers were the protective wall against the epidemic. In the second, they were the guards looking out for the spread of virus on the street and in senior residences. Now, in the third wave, they are leading the charge, overseeing both the Covid vaccination campaign and assisting patients whose care has been delayed by the pandemic.
Spain’s primary healthcare system was already under strain before the pandemic hit, but this has intensified in the last year, leaving it in a state where it is under constant pressure. “There is increasingly more work and with the same amount of resources,” says José Polo, the spokesperson for the Spanish Society of General Practitioners (Semergen). And this is taking a toll on both healthcare professionals, whose mental health is suffering as a result, and on patients, who are more likely to fall off the radar, delay getting care and arrive in a worse condition to their appointment.
We are not an elastic band. Health workers are human and if you continue stretching us, one day we are going to breakMaría Justicia, head of primary healthcare at Madrid’s doctor union Amyt
In the waiting room of the Creu Alta medical center in Sabadell, in Catalonia, 76-year-old Josefa Cerezo and her daughter Marga are killing time looking into space. “It took a lot for me to come,” says Josefa. “It’s difficult to contact the medical center because the telephone is always busy. I had sciatica that was killing me and I ended up going to the emergency ward. Today I am here to monitor my blood pressure.” There are just two other patients waiting in the corridor. To prevent contagion and optimize resources, primary healthcare centers have prioritized phone consultations over in-person appointments.
There is not much happening in the waiting room of the medical center, but inside the doctors’ offices, it’s a different story. “Access has changed, but we continue to provide service for acute but not life-threatening cases like a urine infection, patients with chronic illness and end-of-life treatment with home visits,” says Ángeles Zamora, a nurse at Creu Alta medical center.
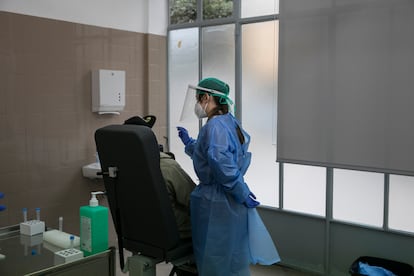
The ground floor of the facility houses an area for suspected Covid-19 patients. “In the first wave, we saw more serious cases. Now there are more family contagions, but they are more minor cases. People continue to be afraid of the virus and they are scared and anxious when they come in,” says Laura Estirado, a nurse on the floor, who wears a personal protective suit and two face masks.
Primary healthcare is the entry point to the health system, but the pandemic has created a bottleneck that cannot easily be relieved. The workload of doctors and nurses has multiplied: as well as being responsible for detecting and tracking Covid cases, they also see their regular patients, as well as those who the pandemic may have left behind, make home visits, assist palliative care patients, coordinate care in the residences of their area and oversee the flu and coronavirus vaccination campaign. All of this, they warn, with practically the same resources they had before the pandemic. “The way things are now, it’s almost impossible to do everything,” says Salvador Tranche, president of the Spanish Society of Family and Community Medicine. “Nursing does 130 million appointments a year and the coronavirus vaccination drive of the general population will involve 50 million more. In other words, it means 50% more activity. You need resources for that.”
The pandemic has not created these shortfalls, which are the result of 10 years of decimating budget cuts, but it has exacerbated them. “Before the pandemic, we estimated that we needed 15,500 more nurses in primary healthcare. Now, just the shortage in nursing is massive. Increasing human resources is crucial,” says María José García, the spokesperson of the nursing union Satse. According to a report from the Spanish Medical Colleges Organization (OMC), spending on the public health system – which falls to the regional governments – was cut by €8.64 billion between 2009 and 2014, a drop of 12.24%. But the cuts were even deeper in the primary healthcare system, where spending fell by 16.17%, a fall of €1.74 billion. “Our schedules are overwhelmed and people are already taking leave due to psychological problems,” says María Justicia, the head of primary healthcare at Madrid’s doctor union Amyts. “The precarious conditions are worsening. If it continues this way, primary healthcare will not be able to endure.”
According to a report from the Spanish Medical Colleges Organization, spending on the primary healthcare system was cut by 16% between 2009 and 2014
The spike in coronavirus cases in the third wave has pushed already strained healthcare centers to their limit. While staff have more experience, more diagnostic tools (unlike in the first wave, they can test for Covid now) and personal protective equipment, there is still a shortage of workers. “We are completely overwhelmed and overstretched,” says Rosa Magallón, the president of the Spanish Primary Healthcare Network of the Spanish Public Health Society (Sespas).
This pressure is being felt above all by the patients who don’t have Covid-19, who arrive in a worse condition to their appointments, if they make it at all. “The diagnosis delays we have are tremendous,” warns Tranche. “Hospital tests are being delayed and we are finding very advanced tumors or important changes in quality of life due to some disease.” The number of operations fell by 36% in the first six months of 2020 with respect to the same period in 2019, and surgery waiting times have skyrocketed – patients wait on average 183 days for a knee replacement, for example. “We are hearing a lot of complaints from patients about test and surgery delays. A cataract is not considered an urgent disease, yet the patient can’t see,” says Polo.
These problems are exacerbated by the precariousness of the healthcare system, which means personnel are often moving from one position to another. “You have to do double shifts, you see patients you don’t know due to the discontinuity of care, and this creates delays. Because we don’t have time to see patients properly,” says Magallón. “Other delays also happen because the patients don’t want to come to the medical center.”
During the first wave of the pandemic, when Spain was under a strict lockdown, people across the country applauded at 8pm every day to show their appreciation for health workers and other essential workers. But now the feelings have changed, says Tranche. “People are furious,” he says. “They scold us because they don’t feel like they are getting proper treatment.” Polo agrees: “They are sullen, angry and upset.” Zamora, however, believes this attitude “is not discontent, but rather fear: they are afraid, they are afraid of losing access [to primary healthcare].”
Strain on health professionals
Working under constant pressure is not good either for health professionals. “We arrive early to work and leave when we can,” says Cándido Pequeño, the head of a medical center in Cee in A Coruña province. “No one asks us to, and no one compensates us for it, but we do it. And that’s what leaves you burned out. We are overloaded. Professionals are despondent and arrive at work suffering.”
Two studies by researchers at Hospital del Mar in Barcelona show that nearly half of health workers are at high risk of mental illness as a result of the pandemic. “There is an increasingly high percentage of health workers who are taking anxiety medication and antidepressants, and people who are on leave for post-traumatic stress,” says María Justicia, who warns: “We are not an elastic band. Health workers are human and if you continue stretching us, one day we are going to break.”
English version by Melissa Kitson.







































