The disease that kills the most children is preventable and curable, but only in rich countries
Pneumonia is a silent pandemic that causes more deaths than the coronavirus, but receives neither the attention nor funding necessary to combat it. Around 700,000 children under the age of five die every year from it, mostly in poor countries
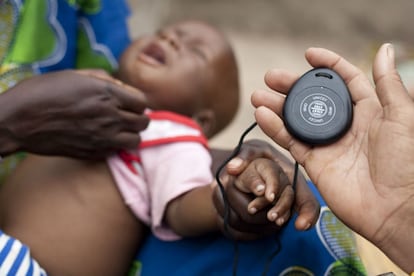
The good news is that pneumonia — the disease with the highest child mortality rate in the world — can be prevented and cured with existing vaccines and treatments. The bad news is that those affected live in poor countries that lack both the funds and the political will needed to reverse this situation. Authorities, international organizations, companies, donors and experts gathered to discuss the issue at the Second Global Forum on Childhood Pneumonia last week in Madrid.
“We are finally going to introduce a pneumonia vaccine in the country in 2024, but we do not have enough resources to buy the necessary doses or to guarantee their application,” said Mohamed Lamine Yansané, Secretary General of the Guinea-Conakry Ministry of Health, summarizing the feelings of many of the authorities present.
Pneumonia kills 2.4 million people annually. It causes more casualties than the officially registered deaths from Covid-19 in 2020, which reached two million. The lung infection claims the lives of 2,000 children under the age of five every day and one every 42 seconds. The profile of the victims is the same everywhere: children born in conditions of poverty or conflict are exposed to infections, malnutrition and polluted air, factors that increase the risk of pneumonia. They live in areas with limited or no access to basic health services.
The international meeting’s objective was for countries, funders and multilateral institutions to set commitments to prevent and treat pneumonia and reduce the number of child deaths. The first Global Forum on Childhood Pneumonia, held in Barcelona three years ago, set specific objectives to curb the disease, but the coronavirus pandemic cut short most of the plans.
“In the last three years, the coronavirus pandemic has killed many elderly people in rich countries, but there is another pandemic taking place now, which kills thousands of children and is entirely linked to poverty,” Keith Krugman, an expert in pneumonia and pandemics at the Bill and Melinda Gates Foundation, told EL PAÍS. “The reality is that children who are victims of pneumonia die in poor countries. There are almost no deaths in rich countries.”
According to Quique Bassat, a researcher at the Barcelona Institute for Global Health (ISGlobal) in Spain, pneumonia has a role in 43% of pediatric deaths. Ending those deaths would mean solving the vast majority of deaths of children under five in the world, he says.
Right now, only a third of children with pneumonia receive the antibiotics they need, according to the World Health Organization (WHO). Half of childhood pneumonia deaths are concentrated in five countries: Nigeria, India, Pakistan, Democratic Republic of the Congo and Ethiopia. The figures are serious, but the general public is unaware of them. Childhood deaths from pneumonia have fallen by half in the last 20 years, but cases are still concentrated in 54 countries, 80% of which are in Africa.
“We still have time, but we must sustain the financial effort dedicated to the Covid-19 pandemic,” said Gustavo Suárez Pertierra, president of UNICEF Spain.
A joint plan between donors and governments
The coronavirus caused the biggest decline in childhood vaccination in 30 years. According to the latest data from UNICEF, the pandemic has undermined confidence in vaccines and has meant that 67 million children have not been fully or partially immunized against preventable diseases. Of that population, 48 million did not receive any type of vaccine. They are called “zero dose” children. In absolute terms, the countries that have the most zero-dose children are India and Nigeria, two of the nations with the highest number of child deaths from pneumonia. One of the forum’s objectives was to find concrete solutions to reach children who have been left out of the immunization systems.
“The coronavirus has taught us several things that can be used to fight pneumonia: the importance of producing oxygen locally to treat the sick, and the need for minimum health services, including vaccines, to work even in a catastrophe,” said Bassat.
Currently, according to the organizers of the forum, 51% of the world’s children receive three doses of the pneumococcal conjugate vaccine (PCV), which helps prevent pneumonia. According to Klugman, in the medium term, two new vaccines will increase the prevention of pneumonia. One works against the respiratory syncytial virus, the main cause of death in babies under six months. It is applied to the mother and is transmitted through the placenta. Another is against a type of strep that kills newborn children, developed by Pfizer.
“We are asking Gavi, the vaccine alliance, and its partners to help us,” said Guinean official Lamine Yansané. “We have almost 200,000 zero-dose children and an infant mortality rate of 90 per 1,000 live births. Pneumonia causes a large part of these deaths,” he stressed. In addition to vaccines, he added, the country also needs greater awareness and the ability to store and transport doses to reach remote parts of the country. According to experts at the forum, low-income countries such as Guinea-Conakry can access Gavi financing for the vaccine, although they agree that the requirements to demonstrate their needs are an obstacle for some eligible states.
“It is unacceptable that children suffer from countries’ inability to pay for vaccines. There has to be a joint plan of donors and countries,” said Klugman, a pneumonia expert at the Bill and Melinda Gates Foundation. But he also stressed governments should create their own economic strategy and not rely solely on donors.
The best vaccine: Invest in girls
Leith Greenslade, coordinator of Every Breath Counts, a public-private coalition of entities that seeks to end pneumonia deaths, believes that, regardless of the funds granted, the problem also lies in the money’s distribution. Donors do not trust local organizations, so the money is channeled through large multilateral or academic institutions in the north that have become “big monsters” that are difficult to maintain.
For her, the solution is to financially support local groups. “We are at a point where you have to ask yourself very tough questions about how the system works,” she said. Her concern is in line with other forum participants, who underlined local health workers’ critical role in pneumonia prevention and treatment.
Reducing infant mortality caused by pneumonia also includes alleviating child malnutrition, promoting education and strengthening the rights of women, who in most affected countries are responsible for the health of their children. “The best vaccine is to invest in girls, who will become informed women and mothers, aware of their rights, with the ability to decide when and with whom they want to have a child, and the courage to demand that governments change things,” said Rebeca Gyumi, director of Msichana, an organization that works for gender equality in Tanzania. “When funds are dedicated to female education in countries like mine, Tanzania, the children of those mothers are less likely to die from diseases like pneumonia.”
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition







































