‘We’re not getting to patients in time’: Experts say Covid-19 has slowed detection of leprosy cases worldwide
Hansen’s disease is one of humanity’s oldest afflictions but remains one of the most unknown, neglected and stigmatized, despite the fact that a cure has existed for 40 years. In 2021, the WHO recorded a 10% increase in cases — another side effect of the pandemic

One day, a person in a remote rural village in India notices a spot on their skin. He or she doesn’t think much of it, and in any case, the nearest health center is dozens of miles away. Months later, that person starts to lose movement and sensation in their hands and feet, and lesions begin to appear on their body. If the person is a woman, she likely does not even consider making a trip to a clinic, because her money is controlled by her husband, and in any case, she has too much work to focus on at home. By the time the patient’s condition becomes so bad that they seek professional help, they may have already suffered irreversible disabilities, such as the loss of fingers or nose cartilage. Around the world, stories of leprosy in areas of extreme poverty, where the vast majority of cases are recorded, all tend to resemble each other. This grim picture could be very different, experts say, if leprosy were not so stigmatized and steeped in ignorance and marginalization, and so neglected by authorities.
“This disease is surrounded by stigma. Governments of affected countries consider it an embarrassment to the nation, and have worked to invisibilize it, hiding the sick despite the existence of a cure,” explained Alice Cruz, the UN Special Rapporteur on discrimination against persons with leprosy, in an interview with EL PAÍS conducted in the lead-up to World Leprosy Day, which was observed on the last Sunday in January. For example, Cruz explained, there are currently more than 100 laws in the world that ostracize people who suffer, or have suffered, from the disease. These include laws that prohibit patients from attending school, from holding various positions of responsibility, or even from entering the country.
Every day, nearly 400 new cases of Hansen’s disease – as the condition is officially called, in honor of the 19th century Norwegian physician who identified the bacteria that causes it – are detected worldwide, although there are many patients who are not included in these official statistics. In addition, experts say that lockdowns and other emergency Covid-19 health measures have impeded case detection and disrupted patient treatment programs. In 2021, according to the World Health Organization (WHO), the number of people diagnosed with leprosy increased by 10% compared to 2020 levels, for a total of 140,594 new cases reported globally.
“In the last decade, there were 3% fewer cases reported annually,” explains Lucrecia Acosta, head of molecular diagnosis of leprosy at the Fontilles Foundation, and a scientific advisor at Anesvad, an organization dedicated to combating neglected diseases. “With the pandemic, most programs around the world were interrupted, the search for new leprosy cases was suspended, and people were deprived of a diagnosis and, in some cases, of access to treatment. This is why it is normal that we’re seeing an increase in documented cases, but there is no increase in actual cases, although it is also true that lockdowns may have increased infection in some contexts.”

Acosta notes that the data for 2022 and 2023, which will reflect the post-pandemic return to relative normality, may show leprosy cases reaching upwards of 200,000 a year – the number of cases documented by the WHO in 2019, based on data provided by the governments of over a hundred countries worldwide.
“First, the priority is to restore other programs, like those focused on fighting tuberculosis or HIV/AIDS,” Acosta says. “Leprosy is not a high priority and is not lethal, so it always comes last. On top of that, it’s a disease that no country wants to have, because it’s considered bad for the national image, and so that’s why there has always been an underreporting of cases. There are thousands of patients who are not included in WHO records.”
In Spain, according to data provided by the Fontilles Foundation, a leading organization in the fight against leprosy, 10 new cases were reported last year. “The disease is highly politicized and the Spanish government, for example, often does not report cases to the WHO; they are registered in the national system, but are not reported,” explains Eduardo de Miguel, the director of international projects at the Fontilles Foundation.
Women are more vulnerable
Over the past 20 years, more than 16 million leprosy patients have been treated with a combination of three drugs administered by the WHO free of charge over the course of one year. This drug course successfully cures leprosy, but to access it, patients must be included in the official registry and be able to access the medicine and receive their doses on time. Experts say that the number of patients presenting with visible disabilities at the time of diagnosis increased by 18% in 2021. “In other words, we’re not getting to patients in time,” says De Miguel.
Leprosy, which is transmitted by tiny droplets expelled through the nose and mouth, is not very contagious, despite its reputation. Invariably, it is also associated with extreme poverty: studies show that when quality of life improves in a given country, the disease eventually disappears. The WHO has identified 23 priority countries in the fight against leprosy, which account for almost 95% of the world’s cases. Among them, India accounts for half of all cases, followed by Brazil with 13% and Indonesia with 7.8%.
According to official data, rates of leprosy tend to be the same among men and women, but girls and women account for only 39.4% of total officially diagnosed cases. “Women face more difficulties in accessing diagnoses and treatment,” says Cruz. Barriers to care are multiple: female patients often need authorization from parents or husbands to visit a health clinic, and they often do not have the economic resources required to travel alone to the closest doctor, and may not feel comfortable undressing to be examined by a specialist. “We also see that women lose much more to this disease than men, and suffer divorces or separation from their children,” says Cruz. “This causes many women to avoid a diagnosis, which ultimately only makes their situation worse.”
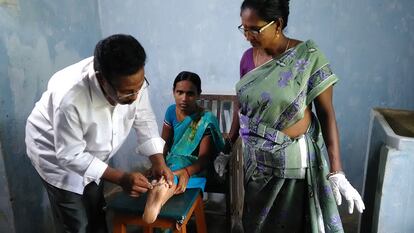
“It’s a major problem,” De Miguel agrees, explaining that in some communities in India, when a person, especially a woman, has a disease that can cause a problem with the community, she withdraws into the home and avoids seeking professional help out of fear of being associated with the disease. “This is why in India we have a program that provides care for women in their own homes, because outside the family context, it’s difficult to access patients. Health advocates, all of them women, go house to house and provide care, to make it easier to access more patients.”
‘Towards zero leprosy’
One of the United Nations’ Sustainable Development Goals is the elimination of leprosy by 2030, although recent trends have led many experts to doubt the feasibility of this ambitious plan. For Acosta, the objective serves as “an incentive” more than anything, but she says it is not realistic given that the world “is currently well above the case levels needed to stay on track to reach that goal.” Acosta explains that there is still no reliable serological test to detect the disease, and no available vaccine to prevent it, but welcomes a recent initiative in the United States to develop a vaccine, which is already being tested in Brazil.
Another reason Alice Cruz is skeptical of the feasibility of the UN’s 2030 goal of “zero leprosy” is because the global health industry is “very market-driven” and “does not generate the tools necessary to fight these neglected diseases,” because it is not profitable. Cruz also stresses the importance of guaranteeing leprosy patients basic rights, like access to clean drinking water and adequate nutrition, which are essential to eradicating the condition. “Diseases are not only biological; they are social and political. Your likelihood of getting the disease depends on the education you receive, the house you live in, and whether or not you can bathe regularly. Access to treatment is also associated with your economic and social level. If you are diagnosed with leprosy, you have to take care of yourself to avoid a disability, but if you have to work every day in the fields, for example, you cannot afford that luxury, and this creates significant additional risks for your health. The health of your body is the result of an entire life. And your life is the result of the history of a whole region or country, and this is reflected in the individual body,” Cruz explains.
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition







































