How Spain’s sixth coronavirus wave is increasing pressure on hospitals
The number of Covid-19 admissions is close to the peak reached last January and is rising at an exponential rate
The sixth coronavirus wave in Spain has been growing since Christmas. The number of cases detected has broken all records, tripling the figure recorded during the worst moment of the health crisis one year ago. Worse still, although the proportion of cases requiring hospital admissions is smaller, the number of hospitalizations has reached very high levels and is continuing to rise.
In the worst week of 2021, 3,600 Covid-19 patients were being admitted into hospital wards and 300 into intensive care units (ICUs) every day. Last week, daily hospitalizations were at more than 60% of that peak: around 2,150 admissions in regular hospital wards and around 170 in ICUs.
The following graphic shows the number of coronavirus cases, admissions and deaths in relation to the wave in January 2021.
In last year’s January wave, some 19,000 people died of Covid-19 in two months. Fortunately, the number of fatalities of the sixth wave so far is much lower, with 1,500 recorded in three weeks. But this figure is likely to rise as there is usually a delay between an increase in cases and an increase in deaths, which may also be notified at a later date.
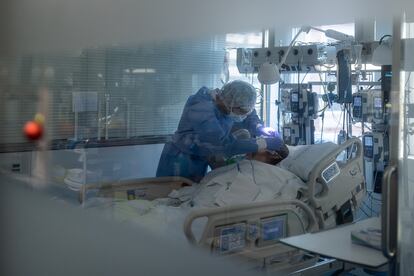
What’s of most concern right now is the number of hospitalizations for Covid-19. The volume is high and is currently rising at an exponential rate. This is putting Spanish hospitals under great pressure. In the northeastern region of Catalonia, for example, Covid-19 patients occupy 41% of ICU beds – a figure that comes close to the peak reached last year, when the region was at a near breaking point. Similar occupancy levels are being seen in the Basque Country (32%), while in Madrid, the Valencia region, Castilla y León and Cantabria, Covid-19 patients are occupying more than 20% of ICUs.
One positive factor to take into account is that some of these Covid-19 patients are mainly being treated for other illnesses. In Spain, the exact figure is not known, but in the United Kingdom, it is around 30%. This is good news because it means that some of the patients counted as Covid-19 admissions are not in hospital due to the virus, but for other health reasons. That said, they should not be overlooked. Firstly, because Covid-19 infection will often worsen their health situation. And secondly, because they are complicating the work of hospitals, which have to maintain separate spaces and protect other patients from getting infected, especially those with compromised immune systems.
Are contagions slowing?
Although it is too soon to say for sure, last week there was a slight slowdown in the number of coronavirus cases detected. Daily infections have been rising in Spain, but they are doing so at a slower rate.
The change is most clearly seen in the data offered by some regions, which are in charge of their healthcare systems, Covid-19 vaccination drives and coronavirus restrictions. In Madrid, for example, Saúl Ares, a systems biologist and researcher at Spain’s national research institute CSIC, explains: “The seven-day cumulative incidence series saw a peak days ago.”
This has also been detected in Catalonia, where the rise in cases has slowed in all age groups, particularly among teenagers. The incidence rate among this age group is now lower than what it was a week ago, perhaps due to school vacations.
This coming week will be key to determining whether contagions are really slowing or whether it is an illusion due to underreporting over the recent public holidays. Spain will be keeping a close eye on the situation in the UK: in that country, cases have been stable for days and hospital admissions also stopped rising last week.
New studies on omicron
In more good news, there is growing evidence that the omicron variant of the coronavirus causes less serious illness. Not only does it infect more vaccinated people – who experience less serious illness – it is also intrinsically less dangerous.
According to a report by the UK Health Security Agency (UKHSA), the risk of hospital admission after infection with omicron was approximately one-third of that for delta (after adjusting for various variables such as vaccination status and prior infections). What’s more, new lab studies offer a possible explanation for this, with research showing the omicron variant is less infectious in the lungs.
But it is important not to remain cautious. As Tedros Adhanom Ghebreyesus, the director of the World Health Organization, explained last week: “Just like previous variants, omicron is hospitalizing people and it is killing people. In fact, the tsunami of cases is so huge and quick, that it is overwhelming health systems around the world.” He added: “While omicron does appear to be less severe compared to delta, especially in those vaccinated, it does not mean it should be categorized as mild.”
The UKHSA report also offered new data on the effectiveness of Covid-19 vaccines against the new variant. The findings, which are difficult to summarize, can be seen from two different perspectives. The research says that the vaccines continue to prevent serious cases of Covid-19. For those who are fully vaccinated, the risk of hospitalization was 50% lower, even after nine months had passed since the shots were administered, while a third dose increased protection to 88%. However, if this data is confirmed, it would mean that we are less protected than we were against the first coronavirus variants, given that the Covid-19 vaccines were up to 95% effective against these.








































