Spain’s hospitals now treating more Covid-19 patients than during fourth and fifth waves
Infection curve keeps rising and 12,942 patients have been admitted into medical centers. Of these, 1,983 are in intensive care, near the peaks of earlier surges
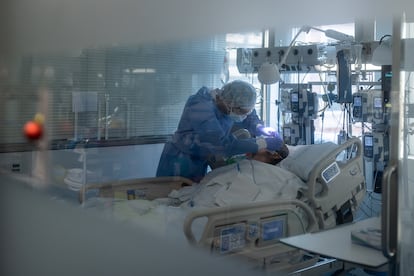
The sixth wave of the coronavirus pandemic is now making itself felt in Spanish hospitals, where there are currently 12,942 patients being treated for Covid-19. The growth in admissions is, however, slower than that seen in previous waves and the proportion of serious cases compared to infections is much lower. But a very high number of contagions has translated this week into a number of hospitalized patients that exceeds the peak seen during the fourth and fifth waves, when the number was around 10,500. The occupation of intensive care units (ICUs), meanwhile, where on Tuesday there were 1,983 coronavirus patients being treated, is now nearing the level seen in the wave during the summer (2,031), and is also getting closer to that of the fourth wave (2,356).
For now, these figures are manageable. They vary greatly from region to region, and while some hospitals have had to reorganize non-urgent surgeries, most have not had to take this step. The problem lies with the fact that this wave is still growing with a force that has never been seen during previous waves.
According to Tuesday’s Health Ministry report, 117,775 new coronavirus infections were registered from the day before, pushing the cumulative incidence up to 2,434 cases per 100,000 inhabitants over the previous 14 days. This suggests that complicated weeks are ahead for the healthcare system, both on wards and in intensive care units, where the peak of admissions will arrive a few weeks after that of notified cases. The ministry report also added 116 fatalities to the official death toll on Tuesday.
Since the pandemic began, one of the major objectives of the authorities has been to avoid the health system from being overwhelmed. Beyond protecting the most vulnerable for what could be for them a deadly illness, the mantra of flattening the curve was aimed at avoiding the critical situation seen during the first wave back in the spring of 2020: overwhelmed hospitals, triage for the admission of patients who were more likely to survive, and total dedication to treating a single illness that disregarded all others.
The milder nature of the sixth wave – in part due to the effect of the vaccines, but also, although it is not known to what extent, due to the intrinsic milder nature of the omicron variant – has prompted Spain’s central government and the majority of regions to not ramp up social restrictions. The measures that help to avoid infection also involve a blow to an economy that has been suffering for nearly two years due to the effects of the pandemic.
The authorities are banking on the healthcare system not being overwhelmed – or at least if it is, the situation will be manageable. Several weeks will have to pass before it can be determined as to whether this was the right way to go. Specialists consulted by EL PAÍS believe that some hospitals could reach their limit toward the end of the month. The mathematical model of Álex Arenas, a physicist and professor at Rovira i Virgili University in Tarragona, indicates that cases may start to fall from mid-January, meaning that the occupation of ICUs could continue to grow for two to three weeks more.
Whether the system is overwhelmed depends on two variables that are still unclear: how many people will be infected, and what percentage of them will require hospitalization and intensive care.
There is still a margin to treat many more patients: in the third wave, which saw much higher figures, there were more than 32,000 Covid patients on wards and nearly 4,900 in the ICUs (there are no such records of statistics for the first wave). But these numbers were a synonym of breakdown in many areas of Spain.
The numbers published by the Health Ministry can be deceiving. According to the latest report, 10.58% of hospital beds are occupied by patients with Covid – some of them may have the coronavirus, but have been admitted for other conditions, something that the official statistics do not reflect. This may appear to be a small percentage, but it’s actually incredibly high for a single illness.
The percentage rises to 21.35% for ICU beds, and here they are all Covid cases. This suggests that many more could be admitted without major problems, but this is not the case. Life continues (more or less) despite the pandemic, and there are still traffic accidents, heart attacks and surgeries that go wrong. The victims of many of these circumstances require ICU care. According to the Health Ministry data, there are more people in ICUs with other conditions (around 3,000) than with Covid (nearly 2,000).
The last official data on structural ICU beds dates from 2017, when there were 4,404. Since then the number has grown and the pandemic has seen capacity multiplied by more than two. In the worst moments, as many as 11,000 beds can be made available. But an ICU space is not simply a bed with a respirator. It also requires the attention of staff, whose numbers have not substantially varied and who are prepared to deal with around 5,000 patients. The fact that there are more beds and ventilators, along with the facilities of surgeries – whose activity has been suspended during the worst moments of the pandemic – means that double the ICU patients can be treated, but this is far from an optimal situation.
Any region with more than 20% of Covid patients in its ICUs enters a situation of stress – as is the case right now in Aragón, the Balearic Islands, Cantabria, Castilla y León, Valencia, Madrid, Navarre and La Rioja. From 30% the situation becomes very complicated – as is the case currently in Catalonia and the Basque Country.
Profile of admissions
Half-a-dozen pulmonologists and ICU specialists consulted by EL PAÍS agree that in serious cases, the pneumonia symptoms presented by coronavirus patients are very similar to those seen in previous waves. The only difference, according to Pedro Landete, from the Spanish Pulmonology and Thoracic Surgery Society (Separ), is that they appear to recover somewhat faster. He works in the Isabel Zendal Hospital in Madrid, where he has seen the average stay in the Intermediate Respiratory Care Unit fall from seven or eight days to five. These figures will have to be analyzed, but if they are accurate, this lower treatment time would lead to a greater capacity for the system to deal with more patients without reaching the limit.
Virginia Fraile, from the Spanish Intensive, Critical and Coronary Unit Medicine Society, indicates that around half of the patients in ICUs have not been vaccinated. This represents a proportion of serious illness that is much higher than that among the vaccinated, given that 90% of the adult population in Spain has been fully vaccinated against Covid-19. “Among the rest, most are people with two doses who did not get a third in time,” she explains.
Health professionals are watching the huge number of infections right now with a certain sense of vertigo, given that they will inevitably lead to more admissions – but no one for now can predict how many. José Luis López Campos, the director of training and teaching at Separ, says that the rise in pressure is already being noted. “Before the sixth wave, we had practically no admissions for several weeks, something that we hadn’t seen since the summer of 2020, after the lockdown,” he explains. “This let us see a ray of light. It took a while, but now we are in a rising period. Very complicated days and weeks lie ahead.”








































