Spain: over one million official coronavirus cases
Patients who survived Covid-19 and medical staff who battled the health crisis tell their stories
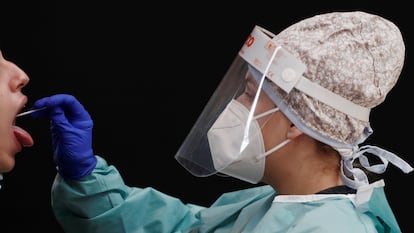
On Wednesday, October 21, Spain reached 1,005,295 confirmed cases of coronavirus, eight and a half months after a German tourist on vacation in the Canary Islands became the first known patient on January 31. But one million is just the official figure; the real figure is undoubtedly much higher.
During the first wave of the pandemic, from March until the end of the state of alarm, there were 246,504 diagnosed cases. However, the ENE-Covid study carried out by the Carlos III Health Institute estimated that at least 5.2% of the Spanish population had contact with the virus, which is close to 2.5 million people. During the second wave, 750,000 have been diagnosed with the virus. But the Health Ministry itself recognizes that possibly only 60% to 80% of the real caseload is being detected. In this case, the actual number of infections would rise to at least 3.5 million, although many experts believe that this is a conservative estimate and that it may be closer to 5 million.
This is the story of the pandemic according to a handful of victims who came down with the disease at four key moments in its trajectory and have lived to tell the tale. January and February were spent giving little credence to the virulence of the disease. The general feeling was that it would not reach Spain and, if it did, that it would not be a big deal. But by mid-February, the virus was already spreading like wildfire across the country, as later studies revealed.
The hospital in Torrejón de Ardoz, Madrid, registered Spain’s first Covid-19 patient in serious condition on February 27, and it changed the criteria for testing. Until then, only those who had been in China or Italy or who had had contact with positive cases from those countries were being tested. But from that day on, testing began on every pneumonia patient whose illness had no clear origin. “We tested a patient who had already been admitted and he was positive,” says Mari Cruz Martín, head of the ICU [Intensive Care Unit] at Torrejón de Ardoz. From that day on, it changed our lives and everyone’s lives. The patient died 15 days later."
“It was explosive, and we didn’t expect it,” adds Martín. “It was like a tsunami; we heard something, we were getting ready, and suddenly, boom, we were flooded. We didn’t think it would come like that, so suddenly. So we felt helpless. We were running out of resources, and we weren’t used to that. We saw standards drop. The other thing I remember is the sadness. The other day a colleague told me that an admission had reminded him of March, because it was very sudden, very fast and very serious.”
1. First cases
Two days later, on February 29, Manuel Pedrosa, 63, arrived at Torrejón de Ardoz Hospital’s emergency room because he had had a high fever for days. He was told it was probably just a cold – the perception of the problem had still not changed. “No one at that time thought there was a virus and I had no idea, either” says Manuel. “We went home. But I was still feeling bad. On March 1 there was a Madrid-Barça game, and I had a season ticket, but I couldn’t go. I got very sick, with a fever of 40º C. On March 6, we went back to the hospital ER. They did the test and after two or three hours they told me I had the coronavirus. I was admitted to the ward, but three days later I had trouble breathing and they told me that I would be admitted to the ICU, that they would try an experimental treatment. In the state I was in, whatever they said was fine with me. I was intubated for 18 days, then I had a tracheotomy and spent 43 days in an induced coma. They told me that they disconnected the ventilator for a couple of minutes, but that I couldn’t manage breathing without it; that I was relapsing. There were times when they didn’t think I would make it. I weighed 75 kilos and lost 14, and even now I’ve only put on eight, although I’m fully recovered, almost without after-effects. I only have pain in my left shoulder, and I go to the physio.” Manuel left the hospital on April 29.
At that time, doctors came up with a cocktail of drugs that were administered to the most serious cases. From a biological point of view, these drugs could plausibly help fight the virus, but there was no evidence that any of them actually did. Over time, it became apparent that most of them were ineffectual, and that many had side effects, according to Ricard Ferrer, president of the Spanish Society of Intensive, Critical and Coronary Unit Medical Care (SEMICYUC). The clearest example of this was hydroxychloroquine, the drug promoted by US President Donald Trump at the time, which besides not proving effective against SARS-CoV-2, also has adverse effects on the heart. The only drug that proved modestly effective was remdesivir. While not a life saver, it did seem to reduce the average stay in hospital by several days. “Now we offer more personalized treatments, depending on the characteristics of each seriously ill patient, we administer corticoids and anti-coagulants, as thrombus tends to develop,” explains Ferrer.

Manuel Pedrosa does not remember anything about the time he spent in intensive care. “I have – I don’t know what to call them – dreams, delirium,” he says. “But I’d better not describe them, because you won’t get back out of your chair. Terrible nightmares. I work with cars, and I remember that I was convinced that I had left a car in the ICU with a trailer attached to take me away. When I woke up, I realized that I couldn’t talk and I had a tube that left a mark on my face, which is now fading. But the worst thing is that when I woke up, everyone was in lockdown. My children came to see me and they told me that there was no one out on the streets; that everyone was at home. I kept crying and crying. And I still cry. I’m very sensitive. It was very hard for me to get my head around why this happened. But it was even harder to get my head around the situation in general. I worry because I know what it’s like to have a business. In 2008, with the crisis, I had to lay off 20 people and it was very hard; and now with this. I find it really difficult.”
In Manuel’s case, there was little in the way of track and trace. As coronavirus tests were like gold dust back then, the only people who were tested were those close to him who showed symptoms. The limited number of tests that Spain had at its disposal were used on people with a high probability of testing positive, meaning that asymptomatic cases, which could account for around 50% of the total, were ignored.
Manuel’s wife had the virus, but only discovered this later when she paid for her own test; she had no symptoms. Neither one of their two children contracted it. Now, what Manuel is keen to stress is his gratitude to the hospital staff. “A huge thank you to the health care workers,” he says. “I take my hat off. There are no words … doctors, nurses, people who put their lives on the line for me.”
2. The first wave
By March, the pandemic was out of control and on the 18th of that month, Asunción Fuster, from Barcelona, was admitted to the Delfos Clinic, where she was transferred from Vall d’Hebron hospital, which was already bursting at the seams. She left on June 8, 83 days later, 71 of which were spent in intensive care. “I don’t remember anything, of course, and thank goodness for that, otherwise it would be torture,” she says. “When I got to the hospital, I was already pretty out of it. The memory I have is of the day I left in a wheelchair, all the nurses applauding, and I didn’t know why. I didn’t understand anything, and they were calling me a ‘champion’ and things like that.”
A force to be reckoned with, Asunción, better known as Chon, has fully recovered but it is her daughter, Silvia Gallés, who remembers what happened during those three months.
“She started with symptoms at the beginning of March and the doctor said it was a flu,” she explains. “We were holding off going to the hospital as they were saying at the time that it was better to stay away, that she could catch the virus there. But then we called another doctor and he tested her oxygen levels and told us to go to the hospital immediately. When we got there, she was taken straight into intensive care. She was exhausted, dispirited, wanting to throw in the towel. She stayed there for 15 days, but then they had to perform a tracheotomy. Later, she also caught bacterial pneumonia in the ICU. We called every night, but we couldn’t go to see her. Luckily, a doctor who had operated on her before and knew her sent us a photo – that was after a month. We were very grateful – it really cheered us up.”
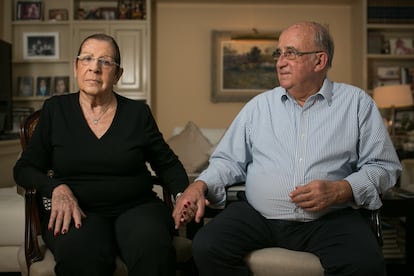
Like thousands of families in Spain, the Gallés family made a WhatsApp group that also included friends. “I posted the war reports, as I called them, every day,” says Silvia. “That was very important, to feel the support of so many people who loved us.” Finally, one day, the family was allowed to see her. “To look in through the window,” explains Silvia. “She would throw kisses at us, although she didn’t remember anything about that afterwards. The nurse would put her ear to the glass, I would yell and the nurse would tell her what we were saying. My brother Pitus had the idea one day of taking an iPad to the hospital with songs that we selected among us – Sinatra, Julio Iglesias –and so there was music to cheer her up, as well as letters and photos of everyone. She seemed to be doing well, but one day they told us she had relapsed and things did not look good. We all got really depressed. In April or May, we were told we should say goodbye. I remember looking for her will at home, thinking about the burial, everything. It was horrible. Then, one day, she opened her eyes and started to wake up. It was slow, and they told us not to get our hopes up too much. We needed to be really patient. The problem was that she couldn’t stay alive without the machine to breathe and, of course, she couldn’t take the machine home. But little by little, she began to breathe without it, until finally she breathed on her own and was transferred to the ward and, finally, discharged.”
The family brought cakes for all the doctors and nurses who had taken care of Chon over the weeks. “They were spectacular,” says Silvia. “We will be grateful to them for the rest of our lives. And they were so nice – guardian angels. They saved our mother.”
Running alongside this story is that of Chon’s husband, Juan Gallés, an 83-year-old businessman who tested positive but was asymptomatic, and who spent the three months his wife was in hospital – and the lockdown – alone at home. “We would take him ready-made food, because he doesn’t cook much, and we would leave it at the elevator door,” says Silvia.
Gallés himself recalls how hard those months were for him. “On two occasions, they told me to prepare myself for the worst,” he says. “I got depressed, which is normal. But I kept my head above water by focusing on my luck – many people were much worse off. I realized that I had to survive, that if the virus got me, my family would be devastated. My wife had to find me here when she came home. And she did come back. But [in his social circle] of the three couples that would go out to eat together, three people died. But life goes on.”
Meanwhile, his wife, Chon, 76, is back in top form: “Scared? I’m not afraid. I go out with a mask on. I used to go out every afternoon to play cards with my friends, but that’s all gone by the wayside, and now you can’t even have a coffee.”
Juan and Chon belong to the most vulnerable demographic when it comes to Covid-19. If the virus has made one thing clear, it is its deadly impact on the elderly. But even among the aged, most cases are not fatal.
In the first wave, one out of five testing positive died in the over-80 group. Many did so without being diagnosed, especially in nursing homes. And it will undoubtedly take time before there are more rigorous estimates of the numbers of deaths that Covid-19 leaves in its wake. What is clear is that the figure of 34,366 released this Wednesday by the health authorities falls short. This year’s excess mortality – that is, deaths above the expected average – already exceeds 50,000. Not all of them have died from the coronavirus, but it is probable that most of the deaths are related to it either directly or indirectly; some because they were not treated for other conditions due to hospitals being overburdened or because they themselves feared being in such an environment and stayed away. Nevertheless, as the second wave is demonstrating, the coronavirus is not a death sentence, not even for the elderly. Now, with the increased diagnostic capacity and many mild cases being identified, more than 90% of positive cases over the age of 80 recover.
3. The deescalation
Summer came and the pandemic abated. And the deescalation process began. But coronavirus cases were beginning to creep up and spread throughout Spain, even reaching the rather remote corner of the country where Beatriz García, a 38-year-old Madrid-based journalist, had been holed up since March with her husband and 13-month-old daughter.
On March 11, they went to their parents' house in El Bierzo in the Castilla y León region. Without a day-care center but with both of them working from home, it seemed like the obvious thing to do. “We packed a small suitcase, thinking we’d stay 15 days, but in the end we were there for seven months,” says Beatriz. “It was a very quiet life. We went out very little. In August, one day, our daughter got a bump on her head. It was nothing. But then she threw up, cried a lot and on August 15, we went to emergencies where, according to protocol, they did a PCR test, because at that stage in Bierzo, there were hardly any cases and everything was working well. And the test came back positive.”
The couple also took the test, which showed that Beatriz was positive and her husband negative, even though the three of them had been sleeping in the same room. “I had only noticed a headache, which I joked about in the Slack [app] at work,” she says. “I never thought I would get it considering the hermit existence I was leading in the town. When I got the result, I started to cry, I really felt a dead weight on me right then and all I could think about was who we had given it to, because our daughter was positive, and everyone had been holding her, and kissing her, and I felt horribly guilty. When everyone tested negative, I was so relieved. I think that’s what will happen to a lot of people. More than worrying about yourself, the worst thing is thinking about who you might have passed it on to.”
The couple was told that Beatriz and their daughter had to self-isolate for two weeks. As it was a two-story house, they kept to the top floor. “They left our food on the stairs,” says Beatriz. “We would go down to the garden every day for a while, but those were three very hard weeks, because I was very tired, and had a headache, and I couldn’t lie down in bed and go to sleep, which is what my body needed, because I had to be with our daughter, playing with her as I was the only one who could do that. My daughter was very good, she had incredible energy. All the viruses she’s picked up at nursery school have been worse. One day I lost my sense of smell – I realized when I smelled nothing while changing her diaper, and in fact, I never knew when to change her,” she laughs. “I ran to the bathroom, opened a bottle of cologne and smelled nothing, absolutely nothing.”
More than worrying about yourself, the worst thing is thinking about who you might have passed it on toBeatriz García, 38-year-old Madrid-based journalist, who tested positive for the coronavirus
For days, Beatriz was obsessed with where she had picked up the virus because she had barely left the house. “I gave myself a hard time,” she says. “It made me feel guilty, like I’d done something wrong, and on top of that our daughter had it. The system worked very well here, though. I saw everyone on Twitter complaining about Madrid but I had three PCRs. They also tracked my family and all my contacts, who all tested negative. They also tested two friends from Madrid who we went for lunch with one day near Ponferrada [the capital of El Bierzo]. And then one day my sister called me and told me that they had closed that restaurant because of an outbreak there; that it had spread to the kitchen and the waiters. It was August 8 and there were four of us, sharing tapas and octopus, but only I got it. We ate indoors – that was the mistake. It was very hot and the air conditioning was on high. I think it was because I was the one who talked to the waitress the most.” Ponferrada, which was hardly affected at that time, was placed under a perimteral lockdown on Thursday.
The track and trace efficiency experienced by Beatriz has been far from the norm in Spain. The summer began with less than half of the contact tracking professionals needed and public health services were overwhelmed. Most experts agree that this, coupled with the fact that primary healthcare has not been strengthened, are largely to blame for the fact that Spain is the country hardest hit by the second wave of the pandemic in Europe.
According to Salvador Tranche, head of the Spanish Society of Family and Community Medicine, talk by the authorities in May and June, starting with Spanish Prime Minister Pedro Sánchez’s speech, advocating shoring up resources in health centers to create a dyke against the virus, has not been accompanied by the necessary means. Primary healthcare centers were earmarked for carrying out quick and early diagnoses, acting as the first track and trace link, but these have been overwhelmed practically since July, when half of the staff went on vacation – in most cases without substitutes. They are now “worn out,” according to Tranche. “You come home after seeing 50 or 60 patients with the feeling that you haven’t done things quite right,” he adds. “And people have the impression that they are not being treated because they call their health centers and there’s no reply. And there are rows breaking out at the entrance [of primary healthcare centers] every day.”
4. The second wave
The end of the summer saw the pandemic return. Coronavirus outbreaks began to multiply. Aragón started to see a rise in transmissions in July and, from there, it moved to Catalonia. But in both regions, the situation seemed to be under control after a few weeks. Meanwhile, in Madrid, the number of coronavirus cases was growing slowly but steadily. By September, the region was already the epicenter of the epidemic in Europe.
Lázaro González, 50, a doctor in Alcobendas in the Madrid region, who works in both a nursing home and a private clinic, started having symptoms on August 30. He went to get tested at his health center – as a doctor and nursing home staff member – he had priority, and he decided to stay at home.
“It was the worst time – it took a week to get the results,” he says. The day the results came back positive, he began to feel worse and went straight to the Emergency Unit of the Santa Sofía hospital in San Sebastián de los Reyes. He was admitted to the ward on September 7 with bilateral bronchopneumonia and left on September 15. “But because I’m a doctor,” he says. “If I’d waited two more days, I’d have gone straight to the ICU.”
Last Monday, more than a month later, he took another test and the result was still positive, but he has already been discharged and, on Tuesday, returned to work. “I’ve had such a variety of symptoms that if a patient had come to me with them, I wouldn’t have believed them,” he says. “I’ve had neurological effects such as problems articulating words – words I could think of but couldn’t say; or instant memory loss – I’d forget what I was doing; I also had insomnia and only slept for two hours at a time; I thought I was short of breath. A week after I was discharged, I lost my sense of smell.” González believes that prevention is the key but says little has been done in this respect. “The epidemiological management has been very poor,” he says. “There is no tracking. If you only attend to those who have symptoms, you won’t get anywhere.”
He doesn’t know where he contracted the virus, but it wasn’t at the nursing home where he works, as there have been no cases there. His wife, his brother-in-law and his son, all of whom he lives with, have only had mild symptoms. But González is asthmatic and obese with high blood pressure. “Until you get it, you have no idea, you think you’ll be asymptomatic, but for those going through it, it’s a very serious thing,” he says.
The total number of coronavirus cases officially passed the million mark in Spain on Wednesday, after several weeks of what seemed to be a flattening curve. The current figures are record-breaking, but the actual numbers are still far from those in late March and early April. The health authorities estimate that at that time the real number of cases was close to 100,000, even though – due to the limits on testing – the highest figure reported was just over 9,000.
Now there are days when the official number of cases exceeds 15,000 and the Health Ministry estimates that the real figures are not much higher than 20,000. The number of Covid-19 related deaths in this second wave have not exceeded 300 on any given day, while in the first wave, during the worse days of pandemic, this figure was more than 900. So though the real number of cases during the first wave is still not comparable with the second, it is heading in that direction. And if the measures taken to curb contagion do not have a significant impact, we will inevitably move toward a similar situation. Hospitals are better prepared to deal with it, but their resources are not unlimited. “ICU beds have increased, but the real problem is one of human resources,” says Ricard Ferrer. “Intensive care workers are not trained overnight.”
Credits. Mariano Zafra, Daniele Grasso and Borja Andrino also collaborated on this report.
English version by Heather Galloway.