MRIs for no reason? The health debate unleashed by Kim Kardashian
The rich and famous want certainty that they are not unwell, but they’re turning to a practice that doctors advise against
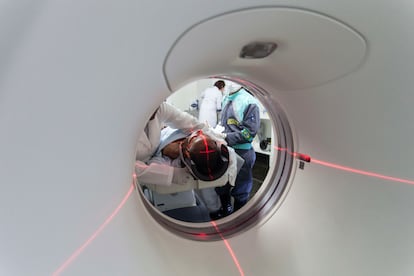
The codes of money and social status change rapidly in these times of technocapitalism. The last time Kim Kardashian bragged on Instagram about accessing elite medical technology, it was to prove that her bottom was real with an X-ray. But this past August, the businesswoman posted about another event that gives her greater peace of mind and all the illusion of control that she needs (at least for a year). Wearing slippers and a gray hospital gown, Kim posed in front of an MRI machine — a tube in which she presumably spent an hour while barely moving, as all of her organs were examined. The full body scan concluded that she had no growths that could cause immediate harm or discomfort.
The photo — with nearly 30,000 comments beneath it, about five times more than her posts usually get — caused a severe case of collective FOMO. Half the world seemed to be wondering: do I need an MRI to get ahead of future illness? Should I take out a loan to afford it?
Kardashian had the scan done at a Prenuvo clinic. The company — based in Redwood, California — offers MRIs for between $1,000 and $2,500, promising to detect tumors, brain aneurysms and degenerative diseases (such as multiple sclerosis) at a very early stage. The company is part of a flourishing industry backed by big investors, many of whom have made the leap from the less lucrative streaming sector.
Ezra, Neko Health and SimonMed are other companies that sell MRIs to healthy people. Neko Health — created by Daniel Ek, the co-founder of Spotify — has raised $65 million this year in a financing round. Prenuvo, meanwhile, raised $70 million in 2022: its shareholders include former model Cindy Crawford and former Google CEO Eric Schmidt. The company benefits from an unprecedented alliance between fashion and medicine: during New York Fashion Week, several designers and models alternated posts of catwalk shows with full-body MRI scans on Instagram. A fusion that may explain the hype that this medical technology is experiencing.
Demand is certainly growing. On one hand, there are the so-called biohackers — highly-paid technological professionals convinced of being able to cheat biology — and on the other hand are the majority, people who have learned of a bad diagnosis from someone close to them and decide to invest in minimizing uncertainty. At the time of the writing of this article, Neko Health claims that its clinics have completed 1,000 MRIs to-date, with a waiting list of 11,000 people. Ezra acknowledged a spike in requests after Kardashian’s post when queried by The New York Times.
The oncologists and radiologists consulted by EL PAÍS observe these practices with a mixture of disbelief and skepticism. Why would a healthy person want to undergo a long — and sometimes unpleasant — procedure, without a clinical indication that justifies it?
“Screening — tracking a disease in a person without symptoms, based on parameters such as age or risk factors — is done with a clear clinical indication, when there’s strong evidence of its effectiveness and the balance between costs, benefits and risks,” explains Dr. Olga Monteagudo, from the Spanish Society of Preventive Medicine.
“These programs are designed to benefit the population as a group — not specific individuals. Opportunistic screening strategies aren’t feasible for the general population, due to their high cost and the low probability of finding tumors without a specific clinical indication,” adds Dr. Rodrigo Sánchez-Varona, an oncologist based in Madrid.
When consulted by EL PAÍS about what can be seen during a full body scan, Asunción Torregrosa — president of the Spanish Society of Medical Radiology and a radiologist at Hospital La Fe in Valencia — emphasizes that the type of MRI being promoted has no ionizing radiation. Hence, in the fashionable scanners, the risk doesn’t exist. However, that doesn’t mean she finds the procedure useful.
“A full body MRI — without organ-specific sequences — has poor resolution and isn’t the most effective for detecting incipient lesions. A lesion visible on a full body MRI is probably already causing symptoms… at least in cancer cases. I find it more useful to detect an aneurysm,” the radiologist explains. She acknowledges that she could get one of those MRIs to feel calmer about the lower-back pain she suffers from, but she prefers not to go through the process. “It’s a long test. For at least 40 minutes, you’re not supposed to move. And [the margin of error] is high.”
What comes after finding a dubious image is “a chain reaction of diagnostic tests with little value — some invasive — which generate anxiety and suffering,” says Dr. Milagros Otero, a radiologist at the University Hospital of Vigo in Spain. A 2019 meta-analysis that studied 5,000 healthy people who underwent this test concluded that 16% of diagnoses were false positives. Only 32% of patients had any “clinically relevant anomaly” detected.
Dr. Otero wonders how often this test should be performed to maintain peace of mind. This doubt is shared by Dr. Carlos Álvarez Fernández, a medical oncologist at the Central University Hospital of Asturias in Spain. “What would be the frequency to remain calm? [Every] two, three, five or ten years?” he asks. “Any test — no matter how sophisticated it may be — always has a limit. [After that], there’ll be no way to obtain more information. Whoever gets into a machine must be aware of that.”
“There’s no extra protection with an annual whole-body MRI. I’ve seen tumors grow in three months,” Otero sighs. “It seems to me that this is the umpteenth phenomenon of consumerism. Medical tests are consumed in the same way as other unnecessary things are purchased. It’s a non-clinical social indicator.”
In most countries, full body MRIs are used to search for distant metastases of certain cancers and for degenerative muscle pathologies, which tend to result in malignant lesions in the kidney and pancreas. However, for a privileged class, the last frontier to conquer is control over health. These are people who worship a single God — technology — and ask him for the impossible: to extend life, free of disease. And, ultimately, to eliminate aging.
Cinthya Molina — a psychologist who practices at the Sha Wellness Clinic — is familiar with powerful people who poorly manage frustration. The possibility of doing an exhaustive check of the body from time to time is a kind of “candy” for one of our modern neuroses: taking tests to try to anticipate the inevitable (the day we will get sick). “The pathological thing is wanting to control even the uncontrollable: when we’re going to die and from what.” She adds that there’s a psychological profile of a person with economic resources who finds it very difficult when a doctor tells them that there’s nothing that can be done about their illness. “It’s difficult for them to accept that, for once, they’ve lost control.”
Dr. Álvarez states that everyone is free to spend their money as they wish. Still, he wants people to remember that an imaging test has a specific intention: to confirm or rule out a suspected diagnosis. He cites a phrase: “He who does not know what he is looking for does not understand what he finds.”
“It’s attributed to the French physiologist Claude Bernard,” the oncologist smiles. “It was the first thing that came to mind with this story.”
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition








































