Coronavirus strain first detected in UK now accounts for more than 80% of cases in Spain, but has not overwhelmed hospitals
Experts blame the variant for the rise of the fourth wave, but say it has not pushed the healthcare system to breaking point as happened in other countries
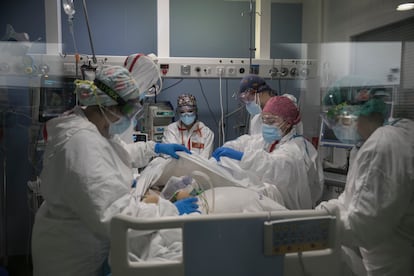
The strain of the coronavirus that was first detected in England has lived up to the threatening reputation that preceded it. The variant was said to be more contagious, and so it has proven to be. While in January it accounted for less than 2% of new cases, now that figure is in excess of 80%, according to the latest data from the Spanish Health Ministry. But there were also fears that it was more lethal, and would push Spain’s hospitals into a critical condition – something that has not happened so far. This is in contrast to what was seen in the United Kingdom at the start of the year and in France in recent weeks.
Experts consulted by EL PAÍS confirm that B.1.1.7, as the variant is known, is indeed causing some more serious cases of Covid-19, although more research is needed to determine whether it is genuinely increasing mortality. The same experts explain that the impact of the strain is having a lesser effect on the Spanish healthcare system. “The worst predictions have not come to pass, which is obviously good news, but it also shows that we still lack a lot of knowledge about the pandemic,” explains Quique Bassat, an epidemiologist and a researcher from ISGlobal, an institute for global health based in Barcelona. “It is not easy to explain why what has happened in other countries has not been repeated here.”
According to the latest report on new coronavirus variants published by the Health Ministry, and dated April 12, the British variant accounts for 90% of new cases in six of Spain’s 17 regions – Andalusia, Asturias, Castilla y León, Valencia, Galicia and Navarre – and 80% in the rest apart from Castilla-La Mancha (77%), Aragón (65%) and Madrid (64%).
“It’s a fact that it has quickly become the dominant strain in Spain,” explains Juan Carlos Galán, the head of virology at Madrid’s Hospital Universitario Ramón y Cajal. “What we still need to research more is whether it causes more serious symptoms or higher mortality rates. There is evidence that suggests that it does, in particular in the 40 to 50 age group, but we still need the evidence to back this up,” he adds.
“There is contradictory and unconsolidated information on this issue,” explains José Miguel Cisneros, the head of the infectious diseases service at the Virgen del Rocío Hospital in Seville. “An article published in [scientific journal] Nature concluded that this variant increases mortality, but a subsequent one did not confirm this.”
The experts warn that while the variant has not seen hospitals overwhelmed, it has had a significant impact. “We are dealing with serious cases among younger people,” Cisneros continues. “The age of patients being hospitalized has fallen. It is true that the system has not been overwhelmed, but I have 180 patients hospitalized and I was not expecting to have this many at this stage of the year, with more of the population having been vaccinated and better weather conditions. It’s clear that all this is due to the variant, which is contributing in a significant way to the fourth wave.”
The vaccination campaign is one of the new variables that could have mitigated the impact of B.1.1.7 in Spain. Jesús Rodríguez Baño, the head of infectious diseases at the Hospital Universitario Virgen de la Macarena in Seville, believes that it is “early to know” whether this is the case and that it should be noted that other countries that have a similar speed of vaccination are suffering greatly. “It’s obvious that the vaccines have reduced infections in a direct and indirect way, especially in environments such as care homes, but we still lack perspective and studies to know whether they have been a relevant factor that has deactivated the danger of the variant,” he explains.

Europe saw a critical moment in January, with the third wave pressuring the majority of countries on the continent. The epidemiological situation was bad, but the forecasts were even worse. The new variants – the British but also the Brazilian and South African – pointed to a future whereby the virus would not only be more serious and more contagious, but also whereby the vaccines could lose their effectiveness.
For Elena Vanessa Martínez, the president of the Spanish Epidemiological Society (SEE), this explains the quick reaction across the continent. Germany, for example, kept its schools closed for months. The European Centre for Disease Control (ECDC) warned countries that they should prepare for a possible “increase in the pressure on healthcare systems.” And the European Union created an ambitious plan with the aim of genetically sequencing up to 10% of positive cases in order to detect new variants and monitor the existing ones.
“The reaction was appropriate after the warnings that came from the United Kingdom,” Martínez explains. “It’s normal for new variants to appear, but until then they were almost unheard of because the ones that were known until that moment were not more dangerous. It was then that we saw that the new ones could be more infectious or cause more serious symptoms.”
Climate differences
The experts agree that one of the reasons that has allowed for the impact of the new variants to be reduced is that containment measures have remained in place. “It has been seen in any event that well-designed restrictions allow, to a certain extent, for daily life to go on, as has been seen by the great job done in schools,” the SEE president adds.
For Quique Bassat, however, this does not explain everything, given that these measures are similar between countries, and within Spain, between regions. And despite this, the incidence and hospitalization rate are very different. “We don’t know why countries like France have had very high incidence rates in recent weeks and not us,” Bassat explains. “The only clear difference is the climate, which allows for more life in the open air and better ventilation, although I believe that this only explains a small part of the reality.
“Once you understand everything that is going on you can design suitable policies,” he continues. “And right now the exact opposite is happening, and we are applying measures that are not producing the desired results. Or conversely, cases whereby we get better results without doing much at all. This is something that we are seeing when we compare countries, but also regions, without being able to explain the reasons why,” he concludes.
English version by Simon Hunter.








































