Researchers discover second case of person resistant to Alzheimer’s
A rare genetic mutation protected a Colombian man from developing the hereditary dementia for two decades. The finding may open the door to new treatments for the disease
In the 18th century, a man — likely from Spain — brought a mysterious disease to the region of present-day Antioquia in Colombia. This individual had a unique genetic mutation — not present in previous generations — which condemned him to an unenviable fate: sudden memory loss at around 44 years of age and early Alzheimer’s at around 49. Today, about 6,000 descendants of that man live in Antioquia, and 1,200 of them carry that mutation, known as E280A or Paisa. Early dementia is so common that in some villages it has popular names, such as “la bobera” after the Spanish word for fool.
On Monday, a team of scientists presented an exceptional case of a man who carried the mutation, but did not suffer cognitive impairment until the age of 67. He is called patient J. He began suffering from Alzheimer’s when he was 72 years old, more than two decades later than expected. Researchers believe that his case opens the door to new ways to search for an effective treatment against the disease.
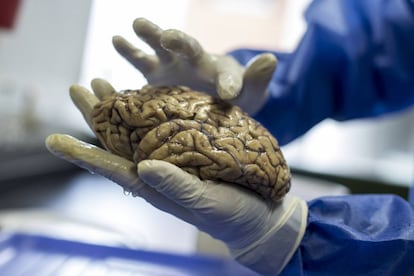
Colombian neuropathologist Diego Sepúlveda received patient J’s donated brain in late 2019, in his laboratory at the Hamburg-Eppendorf University Medical Center in Germany. The man had died at age 74 from aspiration pneumonia, a common infection in people who have difficulty swallowing due to dementia. In the brains of Alzheimer’s patients, it is common to find plaques of beta-amyloid, a protein that clumps between neurons, and tangles of tau, another protein that accumulates inside brain cells. Sepulveda’s team, however, ran into a surprise. In the brain of the deceased there was amyloid beta, but there were hardly any tau tangles in the entorhinal cortex, one of the first areas affected in Alzheimer’s disease. The researchers believe this resistance to early dementia was due to another protective mutation, which they have named COLBOS, an acronym for Colombia and Boston, where most of the authors are from.
Patient J is the second known person to carry the E280A mutation and not suffer from early Alzheimer’s disease. The first was person Aliria Rosa Piedrahita de Villegas, who died in 2020 at age 77 in the Colombian city of Medellín, after suffering from dementia three decades later than expected. Piedrahita de Villegas had a protective mutation, called Christchurch, in the apolipoprotein E gene, which is linked to Alzheimer’s risk.
In this second case, researchers detected a mutation in the gene that expresses reelin, a protein that competes with apolipoprotein E to bind to the same receptors in brain cells. If reelin binds, tau tangles associated with Alzheimer’s disease decrease. If apolipoprotein E binds, they increase.
Sepulveda stresses that the mutations in the two cases possibly have common cellular effects, but the big difference is in the expression of each protein. “The brain swims in apolipoprotein E, we express a relatively large amount and in many parts, while reelin in adults is expressed little and in very specific cells. Our finding tells us that this localized effect is enough to postpone the onset of the disease by several decades,” explains the neuropathologist.
“In terms of therapy, what it tells us is that we can seek to mimic this localized effect, apparently in the entorhinal cortex. Perhaps in the future we will know that some cases will benefit from a global therapy, in the whole brain, while in others it will be enough to protect this specific region,” he adds. His results were published Monday in the journal Nature Medicine.

More than 55 million people worldwide suffer from a type of dementia, with Alzheimer’s accounting for about 70% of cases, according to the World Health Organization. Among the lead authors of the new study is Francisco Lopera, the neurologist who began analyzing early dementia cases in Colombia more than 30 years ago. His team, from the University of Antioquia in Medellín, has studied more than 6,000 members of 25 families, concentrated in one town: Yarumal, which has become a genetic island due to of its centuries-long isolation. According to Lopera, “the secret against the disease” may be hidden there.
Lopera met patient J and says that he lived normally until the age of 67. “What Aliria and J teach us is that disease and cure live together in nature. We just have to read nature and imitate it. If we succeed, we will be able to delay Alzheimer’s by 20 or 30 years,” says Lopera. The Colombian neurologist points to two possible avenues for treatment: developing molecules that mimic the effect of these protective mutations and modifying DNA through gene therapies introduced into the brain by means of a virus.
Neuroscientist Inmaculada Cuchillo applauds the new study but remains cautious. “Due to the novelty, and the scarcity of subjects carrying this mutation, it is too early to consider possible therapeutic avenues from the findings of this article,” says Cuchillo, who is a professor at the Institute of Neurosciences in Alicante, Spain.
In her laboratory, Cuchillo has investigated the reelin protein in the tissues of people with Alzheimer’s disease and has discovered alterations that would impair its protective function. “This mutation seems to have a greater beneficial effect with respect to tau in the entorhinal area of the brain, which is very interesting, because this is the region where the progressive accumulation of tau tangles begins in Alzheimer’s disease. This suggests that this is the reason why it protects against cognitive impairment, despite the fact that tau and beta amyloid continue to accumulate in the rest of the brain,” says Cuchillo.

The researcher compares the new mutation, COLBOS, with the Christchurch mutation carried by Aliria Rosa Piedrahita de Villegas. “Both mutations protect against Alzheimer’s disease and, although the effects on the accumulation of tau and beta amyloid are not the same, the proteins they express — reelin and apolipoprotein E — bind to the same cell receptor, ApoER2, which has been extensively studied in our laboratory. This indicates that this receptor and the signaling cascade that starts after activating it may be key in Alzheimer’s disease,” argues Cuchillo.
The fight against Alzheimer’s disease has so far focused — with little or no success — on trying to reduce the accumulation of beta-amyloid and tau proteins in the brain, which cause the death of neurons.
“It is possible that a treatment focused on increasing the function or levels of reelin may be key to finding a therapy against Alzheimer’s, but, taking into account the primary functions of reelin in the development of the nervous system and neuronal connection, we must be cautious,” warns Moreno. “The function of this molecule is finely orchestrated: both low and high levels can be detrimental.”
Colombian neuropsychologist Yakeel Quiroz, from the Massachusetts General Hospital in the United States, co-led the research on patient J. She is also optimistic about the study. “Our findings with this exceptional case open new doors for the development of Alzheimer’s therapies,” she says.
Her colleague Joseph Arboleda, from Harvard Medical School, founded the company Epoch Biotech, which is trying to develop treatments inspired by Alzheimer’s-resistant patients. “Current drugs offer very limited benefits. Our patients were protected for more than 20 years and the hope is that new therapies will do the same,” he notes.
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition
Tu suscripción se está usando en otro dispositivo
¿Quieres añadir otro usuario a tu suscripción?
Si continúas leyendo en este dispositivo, no se podrá leer en el otro.
FlechaTu suscripción se está usando en otro dispositivo y solo puedes acceder a EL PAÍS desde un dispositivo a la vez.
Si quieres compartir tu cuenta, cambia tu suscripción a la modalidad Premium, así podrás añadir otro usuario. Cada uno accederá con su propia cuenta de email, lo que os permitirá personalizar vuestra experiencia en EL PAÍS.
¿Tienes una suscripción de empresa? Accede aquí para contratar más cuentas.
En el caso de no saber quién está usando tu cuenta, te recomendamos cambiar tu contraseña aquí.
Si decides continuar compartiendo tu cuenta, este mensaje se mostrará en tu dispositivo y en el de la otra persona que está usando tu cuenta de forma indefinida, afectando a tu experiencia de lectura. Puedes consultar aquí los términos y condiciones de la suscripción digital.








































