New technique opens the brain to unprecedented neurological treatments
A study in monkeys and human patients shows how the blood-brain barrier can be crossed to allow the delivery of drugs that, in theory, could treat Parkinson’s and Alzheimer’s
For decades, neurologists have hit a seemingly impenetrable wall: the blood-brain barrier (BBB). This complex network of blood vessels and immune cells protects the most important organ in the body, the brain. The barrier only opens to let in oxygen and a few other nutrients, and cannot be breached by most pathogens, a feature that is key to the brain’s survival. But there is a downside to this: virtually all drugs designed to cure brain diseases, including cancer, fail to reach their destination.
Today, a study led by Spanish doctors shows how part of the blood-brain barrier can be opened up to allow the delivery of drugs that, in theory, could treat Parkinson’s and other neurological diseases such as Alzheimer’s and Huntington’s disease.
This work has shown that the blood-brain barrier can be opened for a few precious hours to deliver the desired drugs to the brain. To achieve this, the researchers have used a very new technology: low-intensity focused ultrasound (LIFU).
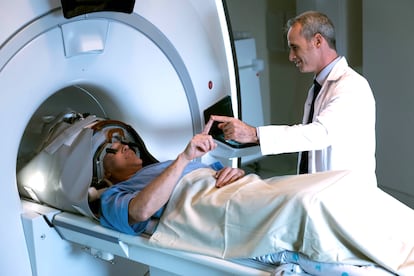
This non-invasive treatment is performed on a machine similar to an MRI. The subject wears a helmet that emits inaudible soundwaves that manage to reach very specific areas of the brain, as the machine is guided by real-time brain images. Prior to this, lipid-shelled microbubbles are administered, and these are activated inside the blood vessel when they come into contact with the soundwaves, opening a crack a few millimeters wide in the BBB — which is big enough for the desired drug to slip through.
Researchers tested this technique on monkeys, and found that they can open the brain barrier for about 24 hours and introduce deactivated adenoviruses, which are commonly used for gene therapy, in which gene treatments are delivered directly to the target area. No apparent side effects were reported. The study, which was published in Science Advances, also reported that this same technology was also able to temporarily deactivate the BBB of three Parkinson’s patients, in the exact part of their brain that was being targeted.
Non-invasive technique
“Our ultimate goal is to treat neurological diseases, such as Parkinson’s, early and non-invasively,” says José Obeso, a neurologist at the Abarca Campal Integral Neuroscience Center in Madrid, and lead author of the study.
One in four people will suffer from a neurological or mental illness in their lifetime. But of the more than 7,000 known drugs, only 5% are able to reach the brain. Parkinson’s disease — which was first described by the British doctor James Parkinson in 1817 — causes tremors, muscle stiffness and impaired coordination. It is caused by the degeneration of nerve cells in a part of the brain called the substantia nigra. Although there are treatments for the symptoms of the disease, Parkinson’s — which affects seven million people worldwide and is the fastest growing neurological disease — has no cure.
Until now, experimental gene therapies had to be delivered to Parkinson’s patients directly into the brain, which involved piercing the skull with needles to bypass the blood-brain barrier. The new LIFU technique opens up the possibility of delivering gene therapy without surgery or serious side effects.
Researchers have already begun a new round of tests with monkeys, this time administering the GDNF gene, which produces a protein that protects neurons and their dendritic branches. “If all goes well, we could start testing on patients in the summer of 2024,” says Obeso.
Ultrasound-based therapies have been revolutionary in the treatment of Parkinson’s tremors. A similar technique, using high-intensity — not low-intensity — ultrasound, was able to target specific areas of the brain, reducing involuntary tremors by up to 80%. The treatment is performed while the patient is awake.
The million-dollar machine
The low-intensity technology used by Obeso’s team has been developed by the Israeli company Insightec, and requires a machine that costs around €1 million ($910,000). There are very few in the world, as the machines are still experimental. The company is funding clinical trials in Canada, Italy and South Korea. These trials have reported initial success in opening the blood-brain barrier in patients with Alzheimer’s and glioblastoma, the deadliest brain cancer. According to Obeso, in addition to Parkinson’s, the technique could also be used to treat rare diseases in children, such as the genetic disorder Gaucher disease, which is caused by a problem with the GBA gene.
Obeso acknowledges that there are still many questions to be answered, principally whether the treatment will be able to reach the affected area of the brain and reverse the course of a disease. This application could be effective in the early stages of Parkinson’s or Alzheimer’s, since once the neuronal death has spread throughout the brain, it appears impossible to reverse it. The challenge now is to be able to diagnose these ailments years or decades before the first symptoms appear. And there is one more hurdle to overcome: around half the population could have antibodies to similar kinds of adenoviruses as the ones used in gene therapy, meaning their body may reject the treatment.
Chemist Meritxell Teixidó, president of the biotech company Gate2Brain — who did not take part in the study — says the findings are very important for the field. “This is very good news because it gives us one more tool to try to deliver drugs to the brain. The fact that it has been successful in primates, which have brains that are much more similar to ours than mice, is very promising,” says Teixidó, whose company is also developing therapeutics that can cross the BBB. He is working on developing small proteins — inspired by insect venom — that can cross this biological barrier and deliver drugs that target brain tumors in children. The third known way to reach the brain, specifically its lower area, is to enter the molecules through the nose until they reach the olfactory bulbs. “That is why some drugs are snorted,” explains Teixidó.
Álvaro Sánchez Ferro, coordinator of movement disorders of the Spanish Society of Neurology, is also interested in the new technique as it is non-invasive. But he warns that it is still in the initial stages of development. “Now we have to show that it has clinical benefits in patients. It may take 10 or 15 years, but it’s worth trying,” he says.
Diego Santos, a neurologist at the University Hospital in A Coruña, Spain, believes that the study’s results are of great interest. “Being able to penetrate the central nervous system may one day allow larger amounts of a drug to be delivered to the brain,” he explains. “What’s more, it’s a procedure that seems safe and reversible. It’s exciting.”
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition








































