Coronavirus patient, 28, in Spain’s ICU: ‘I wasn’t careful. I was walking around without a mask’
Vanessa Martínez did not think she was at risk of Covid-19; now she is having to relearn how to walk and brush her hair after spending 69 days in intensive care
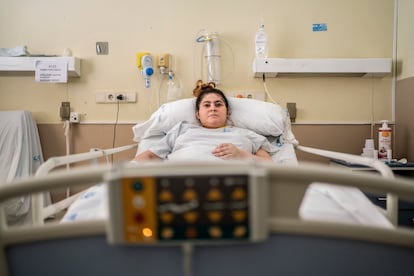

On August 26, Vanessa Martínez will celebrate her 29th birthday in a hospital bed at the Gregorio Marañón hospital in Madrid. The scars of her tracheotomy are still visible, she can no longer see properly, and she has to relearn how to walk. Just a week ago they removed the tube they put in her bladder on April 22, when she was admitted into the intensive care unit (ICU) with Covid-19. She spent 69 days there. On June 29, Martínez was moved to a normal hospital ward, but she still has months of treatment ahead of her. “It’s one day after the next after the next,” she says. “I was irresponsible.”
Martínez never thought she would contract the coronavirus. Not even when a senior residence in Orpea de Algete, a municipality northeast of Madrid, called her in to work as a cleaner. She was later asked to be a nursing assistant. “They told me that they needed people, that although I had no experience it was easy. I said yes despite the risk because I needed to work for my daughter,” explains Martínez. Her eight-year-old girl Allison has Down syndrome and lives with her family back in Honduras. Martínez left that country in 2015 to work in Spain. “The treatment for the medical complications [of Down syndrome] is very expensive, and I had no other choice.”
The need to work and the belief that the Covid-19 wouldn’t affect her were key factors. “I wasn’t careful. I was walking around without a mask. I was young, why would I get infected? And here I am,” she says. Martínez was admitted into hospital on April 5, but she doesn’t remember much about what happened. “The day I arrived in a taxi to Goméz Ulla [hospital in Aluche], I had a fever and felt immensely tired. From there, I was taken in an ambulance to the Ifema field hospital. I don’t remember anything more,” she says. Leyre Pérez, the infectious disease doctor who is treating her, helps with the dates: “She was admitted into [Gregorio] Marañón hospital on April 17, they brought her here from Ifema because she was experiencing complications. She entered the ICU four days later and we brought her to a ward on June 29.”
It is one of the most serious and longest cases that the Gregorio Marañón hospital has treated. Since the beginning of the pandemic, the center has admitted 6,511 Covid-19 cases, 2,861 of them acute and 248 which were placed in intensive care. All serious cases require a long rehabilitation period. Pérez explains that “maintaining a patient asleep for such a long time requires strong sedation to relax all the muscles, and this leads to loss of muscle mass and many long-term health effects.” The lungs are the worst affected, but the digestive and cardiovascular systems can also suffer, while nutritional deficiencies can affect organs like the eyes. And then there is the problem of recovering mobility.

When Martínez was placed in a normal hospital ward, she was no longer able to support the weight of her own head, which she now props up with a few pillows. She misses being able to have a shower. “For three months, they’ve been washing me with sponge baths, and until not long ago, I couldn’t even go to the bathroom alone. They have been putting diapers on me … Diapers,” she says. Despite everything, Martínez manages a smile when Anabel García, one of the nurses looking after her every day, appears at the door. García says her job is to take care of Martínez by doing “whatever it takes,” and she admits it is not always an easy task. “There have been very difficult phases, moments of anguish, because it is a very slow process. But it is also very gratifying when you see that they [patients] are making progress. She is making progress.”
Martínez’s progress now largely depends on a room located on the ground floor of the hospital, which is tasked with rehabilitation. This area is one of eight specialties, including psychiatry, internal medicine and pulmonology, that make up the recovery program for Covid-19 patients who have been in intensive care. As well as Martínez, there are another 30 patients in the program.
Olga Arroyo, is the head of the rehabilitation department, which covers physiotherapy, occupational therapy and speech therapy. She explains that “Vanessa has neurological and neuropathic complications, as well as problems with the central nervous system, lack of balance, reflexes .... We have to reteach her all of that, taking into account the respiratory problems as well.” The recovery period for these patients can be very long. “Rehabilitation will easily take eight months, and there will still be health effects and they won’t recover 100%,” warns Arroyo.
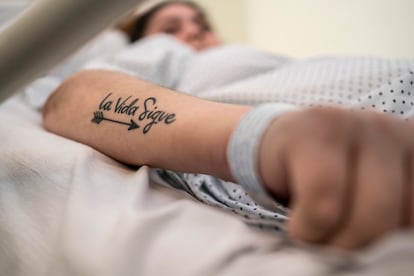
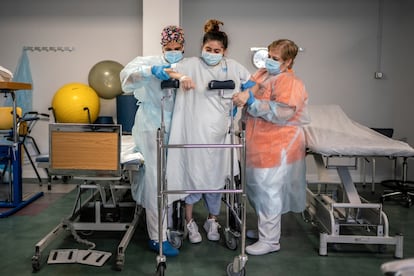
Rubén Juárez, one of the rehabilitation doctors, says the most important thing is to help patients how to relearn basic actions like sitting, standing, brushing their teeth, taking a shower and eating. “They have to relearn how to do it,” he explains while looking at Martínez as she tries to move her stiff feet using a walking frame. Martínez’s physiotherapist, Cristina Muñoz, holds her up. The specialist says her progress has been slow, but steps have been made: “If she had strength in both arms she would already be able to comb her hair by herself, but at the moment only one arm can reach the head. The buttock is stronger and she is able to stand up by herself, although she still does not have enough strength in her pelvis and legs.”
Martínez can’t maintain the effort for longer than 30 seconds. “It’s little by little, although I would like to run out of here right now. But I can’t. I will have to go back to the room,” she says, as she is eased back into the wheelchair. While they are placing her hands and feet in the chair, a tattoo is revealed on her left arm. It says: “Life goes on.” Martínez looks at the message and nods in agreement: “And I am thankful for that.”
English version by Melissa Kitson.







































