An army of mosquitoes modified to fight dengue fever
EL PAÍS accompanies Doctors Without Borders on a pilot project in Honduras that has released the ‘Aedes aegypti’ variety with Wolbachia bacteria to combat the disease at a time of record cases in America


First it’s asphalt and then dirt roads. We’re in the weeds. From the top of the Canaán neighborhood you have one of the best panoramic views of Tegucigalpa. The tallest buildings are far away, but they are few; closer are the tin roofs, the lush vegetation, a royal poinciana tree, which litters the ground with its large orange flowers. Even here, attached to a post in one of the most challenging neighborhoods of the Honduran capital, there are information posters about the Wolbachia method. This new pilot project to control dengue fever is being conducted by Doctors Without Borders and EL PAÍS has accompanied the organization in the release of thousands of mosquitoes in a key test to combat an epidemic that is breaking records in the region.
Dengue is bleeding the Americas dry. So far in 2023, the highest number of infections in the last five decades has already been recorded on the continent: more than 3.35 million. And there have been 1,567 deaths, according to the Pan American Health Organization (PAHO). More cases than ever have been recorded in Mexico, Bolivia, Peru and Brazil. In Argentina, patients have multiplied by 160 compared to all of 2022, in what is already the most lethal outbreak in the country’s history. Behind this health emergency is the Aedes aegypti, a mosquito that is extremely skilled at adapting to humans.
The mosquito lives in stagnant water, but it prefers it clean: it lays its eggs in pots, containers, or garbage bags that form little basins when it rains, and it also breeds in wells. It is more attracted to dark colors and it is the female that bites. It has recognizable black-and-white legs and breeds outside, but always returns to the house. The ‘little fly’ with the innocuous sounding name is responsible for an estimated 440,000 deaths per year, according to the World Health Organisation (WHO). With climate change and rising temperatures, the insect is adapting faster and better and is appearing in new places.

Aedes transmits the so-called arboviruses, dengue, Zika and chikungunya, for which there is still no effective vaccine. Therefore, given the uncontrolled spread of the disease, the focus of health campaigns has been on avoiding bites from the mosquitoes that transmit the disease. This is where the release of these insects with Wolbachia comes in. Honduras is going to be the first country in Central America and the second on the continent (after Colombia) where the method is used. Although it is not a silver bullet, and is more useful combined with larvicides and household insecticides, it has opened a new front of hope.
The hatchery
There are hundreds of them and they get very angry when the light is shone on them. They have been locked in a boat with water, powdered liver (typical fish food) and activated charcoal for 10 days. They have grown from tiny eggs and pupae to these giant adult mosquitoes. Their caregivers from Doctors Without Borders, Jocelyn, Fer, and Alejandra, have been monitoring their growth since they arrived in refrigerators, sent by their mother colony: the biofactory at the World Mosquito Program (WMP) in Medellín, Colombia.
In the insectarium that the medical organization has built in Tegucigalpa it smells like an aquarium and it is 29 degrees, which is what suits them best. The workers have put cotton candy on the top of the boats where they are trapped so that they can feed, but the females want blood, they need it to reproduce. So the women sometimes put their arm in the container to receive dozens of small bites. All for the success of the ambitious project that Doctors Without Borders has with the National University of Honduras, the Ministry of Health and the WMP against one of the most resistant endemic diseases in the region.

Wolbachia is a bacteria that occurs naturally in around 60% of insects, from dragonflies to bees and butterflies. But not this mosquito. For more than 15 years, the WMP has been extracting Wolbachia from fruit flies and injecting it into the eggs of the Aedes aegypti. The bacteria prevents the spread of dengue, the mosquito may host the disease, but it does not transmit it. The first modified mosquitoes were released in northern Australia more than 10 years ago and the area was soon declared “dengue free.” It has also worked in Indonesia, where the incidence decreased by 77%. At Doctors Without Borders they call them “safe mosquitoes”: there are bites but there is no fever, muscle pain, or hospital.
The next step in the plan is for mosquitoes with Wolbachia to reproduce with local populations. There are two options, explains the logistics manager of Doctors Without Borders, Stavros Dimopoulos: if the female has Wolbachia and the male does not, the next generation will also inherit the bacteria and will not be able to transmit dengue, if the male has Wolbachia and the not the female, “the eggs will not hatch or will be too weak to become adult mosquitoes.” The population is not suppressed, so as not to generate an imbalance in the ecosystem, but rather it is replaced. “In sites with a high breeding density, the proportion of mosquitoes with Wolbachia can reach up to 98%. But it takes a while: probably about three years to reach that percentage, but it is capable of being maintained for a very long time,” explains Dimopoulos. Mathematical studies speak of between 60 and 80 years with mosquitoes without dengue.

Mosquito delivery
It’s the first day and Héctor Espinosa is excited. He is 38 years old and goes everywhere on his motorcycle. In the past, his work involved running errands around Tegucigalpa and carrying tourists or packages. This Tuesday in August, as the sun rise at five in the morning, the Honduran puts on his shin guards and secures his backpack full of mosquito canisters. Each container has between 150 and 200 Aedes. Previously he had worked for Hugo and Pedidos Ya, commonly used applications for ordering takeaway food in Honduras: “This is like a delivery of mosquitoes,” he jokes, “but it will benefit my country.”
A supervisor and 10 motorcyclists are going to do 250 routes for six months to free the mosquitoes with Wolbachia. In total, they are going to release more than eight million, that is 40,000 new mosquitoes every day. The distribution is carried out in El Manchen, an area north of Tegucigalpa, which suffered one of the worst dengue outbreaks last year and which usually registers almost half of the cases in the entire capital. It covers 39 neighborhoods, ranging from the boundary with the imposing United States embassy, to the high neighborhoods controlled by the gangs. On the same day, the delivery drivers meet former Honduran president Carlos Flores, who is walking his Yorkshire terrier in the wealthy Lara neighborhood, and they leave early for La Fraternidad, one of the more dangerous areas guarded by the police, “before the guys wake up” and make their work difficult.
About 90,000 people live in El Manchen. If all goes well, by 2025 dengue cases in this area should have dropped between 85% and 95%; It should also affect the Aedes population of the entire Central District, where Doctors Without Borders calculations point to a 30% or 40% reduction in cases. A revolution for an area where dengue has become an unwelcome companion.

All the residents of these housing projects that América Futura has asked know of a case of dengue in their immediate environment, they themselves or their families have suffered from it. The mother of a gang member was admitted to the hospital a couple of weeks ago, she was saved and now she is watering her flowers again; several members of the family of Wendy Espinal, a neighbor from Canaán, fell ill at the same time from the bites a few days ago, and the girlfriend of Isaac Martínez, one of the Doctors Without Borders delivery drivers, cannot get out of bed because of the disease. Meanwhile, he navigates the streets of Manchen on his Suzuki carrying modified mosquitoes on his back: “I think of it as work, but as help for my community. And if it turns out well for the country, it would be something we have fought against all our lives.”
“But they are crazy, how are they going to release more mosquitoes?”
Sandra Espinal’s breathing is agitated as she winds her way up the hill in sector four of the Canaán neighborhood. At 45 years old and with two long black braids, Sandra is the key piece of the second part of the plan that humanitarian organizations, the government, and the university have designed to combat dengue. Without it the chain falls apart.
In Tegucigalpa, as in most Latin American capitals, there are many areas that cars cannot reach. Cleared land, where the path has been made with machete: nothing with wheels can drive through there. Thus, in addition to the motorcycle distribution of mosquitoes, Doctors Without Borders has come up with what they call “community liberation.” Until January they will be placing boats in the houses of the residents of Manchen so that they themselves can raise and release the mosquitoes with Wolbachia. This is easier said than done. It takes six months work in the background.

“We went house to house asking and explaining,” says Espinal, who is a leader of La Estanzuela community. She has the trust of her neighbors and is able to gain access to an area completely controlled by the gangs. Alicia Salazar’s first response to the project illustrates the mood: “Oh, no, but these guys are crazy, how are they going to release more mosquitoes so they won’t come [and bite us]?” Sandra says that she was also shocked at first: “People get scared and think that they are going to have a large cloud of mosquitoes, and they won’t even be able to see. But we were already training and understanding the method.” To support the project, Doctors Without Borders conducted a survey among the population before it started the releases: it received 93% approval.
Carmen Mendoza has not even gone out to the grocery store for a soda this morning. She is waiting for the doctors and Lilian Carbajal, the organization’s health promoter, who was telling her about Wolbachia. Carmen says that she was not afraid of the releases, on the contrary: “I was happy, because it’s like a swarm, we can’t even sleep at night because of the mosquitoes.” Her 15-year-old son was admitted to the hospital for two weeks with dengue fever. He survived, but the fear has not gone away.
Her well is covered, because she knows that it is a breeding site for Aedes. In these neighborhoods, water only arrives for two hours on Mondays and Thursdays. For the rest of the week it must be stored, in wells, in buckets, or in containers and used for washing and bathing. That is one of the reasons why cases are multiplying throughout the Manchen area. Poverty, the high concentration of people, proximity to the mountains, and the normalization of symptoms are some of the others. Sandra Espinal’s granddaughter had hemorrhagic dengue. It took them a while to take her to the hospital because they thought it was just a fever. “The doctors scolded us, they said ‘how is it possible that we waited for it to reach that stage,’ that the girl could die of dengue. She was six years old. Sometimes we didn’t take the risk into account. Because we understood it was something that we lived with every day in our communities and we did not try to combat it.” Until now.

Six health emergencies in a decade
Before the releases, technicians from the National University of Honduras (UNAH) calculated that in the Manchen area, six out of every 10 mosquitoes were Aedes. Now, the same motorcyclists who release Wolbachia are in charge of making new captures so that the Microbiology Institute at the university can monitor how the bacteria is growing among the populations. For that, researcher Dennis Escobar explains, you have to do a PCR test on the mosquito. When they arrive at the laboratory, the mosquitoes are liquefied and, using reagents, the DNA is separated and analyzed to check if it has Wolbachia. They will spend 18 months taking samples. This monitoring is essential to verify the effectiveness of the project.
“It’s not about generating information that looks good on paper, but rather, it is very useful for decision-making by the authorities, thinking about being able to scale it up in the future and bring this methodology to other sites,” says Escobar, who points out that until now the government’s “operational capacity” against the disease has been limited. The objective, says the researcher, is that it can be part of the Ministry of Health’s package of options to fight dengue.
The coordinator of the Doctors Without Borders project, Edgard Boquín, explains that the organization chose Honduras from the entire region, because, in addition to the vulnerability of its medical infrastructure and its exposure to natural disasters, his organisation has attended six health emergencies due to dengue since 2010, the most recent one being just last year. One of the outbreaks in 2019 left more than 100,000 cases and 180 deaths, in addition to overstretched hospitals.
“It was the time when we said that we had to do something different and sustainable,” the coordinator explains. Initiatives like these are long — they are not useful for controlling an outbreak because the first results will be seen in a few months — and they are expensive. The organization has budgeted $1 million for the entire project (WMP’s modified mosquitoes alone cost $500,000). But it also takes the burden off health systems that are overwhelmed with each emergency.
The organization and experts are convinced they can replicate what they have just started, not only in other areas of Honduras, but in other Latin American countries that are also engaged in the battle against dengue. The sky opens and the Supaya basilica watches over the traffic of Tegucigalpa. Among the cars, 10 motorcyclists pass by carrying red backpacks and the best weapon yet in the fight against the region’s mosquitoes.
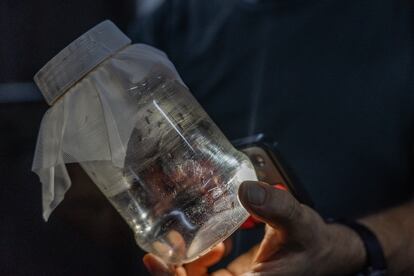
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition
Tu suscripción se está usando en otro dispositivo
¿Quieres añadir otro usuario a tu suscripción?
Si continúas leyendo en este dispositivo, no se podrá leer en el otro.
FlechaTu suscripción se está usando en otro dispositivo y solo puedes acceder a EL PAÍS desde un dispositivo a la vez.
Si quieres compartir tu cuenta, cambia tu suscripción a la modalidad Premium, así podrás añadir otro usuario. Cada uno accederá con su propia cuenta de email, lo que os permitirá personalizar vuestra experiencia en EL PAÍS.
¿Tienes una suscripción de empresa? Accede aquí para contratar más cuentas.
En el caso de no saber quién está usando tu cuenta, te recomendamos cambiar tu contraseña aquí.
Si decides continuar compartiendo tu cuenta, este mensaje se mostrará en tu dispositivo y en el de la otra persona que está usando tu cuenta de forma indefinida, afectando a tu experiencia de lectura. Puedes consultar aquí los términos y condiciones de la suscripción digital.








































