Pere Ginès, hepatologist: ‘There will be an increase in cirrhosis and liver cancer cases because alcohol consumption has not been curbed and neither has obesity’
The Barcelona-based researcher has recently validated a scale published by ‘The Lancet,’ to determine the risk of the healthy population developing chronic liver disease, a condition that usually doesn’t cause symptoms until it’s very advanced
The liver doesn’t hurt or complain when it suffers. At least, not at first. Chronic liver disease develops silently for years, without giving off symptoms or warning signs. It advances discreetly, bolstered by risky alcohol consumption, hepatitis virus infections, or fatty liver disease, which is associated with being obese or overweight. Only in more advanced stages — when cirrhosis or cancer already plague an exhausted liver — does chronic liver disease show up.
Detecting this disease early was a pending task for the scientific community, which until now didn’t have tools that were robust enough to diagnose it in its early stages. Research recently published in The Lancet has validated a risk stratification scale, which can identify apparently healthy people in the general population who are at risk of developing serious liver disease in the future.
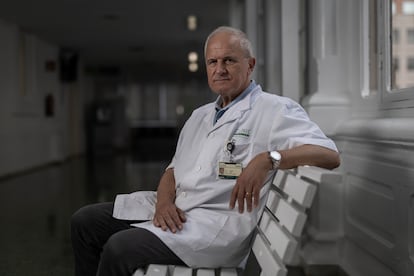
Pere Ginès — a consultant to the Hepatology Service at the Hospital Clinic of Barcelona and the head of the Chronic Liver Diseases working group — is the coordinator of this index, which measures eight variables. “We’ve tried to make it easy; it’s cheap and accessible. It includes eight variables: age, sex and six analytical variables that [are part of] the conventional analyzes that a person undergoes during a routine check-up.”
During an interview with EL PAÍS, the 66-year-old hepatologist warns of a growing epidemic of severe liver disease. He aspires to turn the latest tool into an early detector and implement screening for these ailments among the general population.
Question. Is chronic liver disease totally silent?
Answer. It doesn’t give off any symptoms. Zero. Hence the importance of detecting it early through some measure that’s effective, such as [the recently-developed] scale. The patient develops cirrhosis: it evolves and there comes a time when the cirrhosis becomes complicated. That’s when the person has symptoms. But, of course, they’ve been developing the disease in their liver, silently, for 25 years. And it wasn’t possible to detect it, because we didn’t have the appropriate tools to do it.
Q. What happens inside the liver when the disease is developing silently over the course of 25 years?
A. What happens is that there’s something that injures the liver. This “something” is highly variable, but most often [it turns out to be] hepatitis viruses, which specifically cause liver infections. The other major cause is alcohol consumption, which doesn’t necessarily have to be extraordinary, but falls within what many people would think is normal consumption, but, if continued, can damage the liver. Another major cause — which, at the moment, is the most frequent one — is related to obesity, or being overweight and having diabetes. This causes fat to be deposited in the liver (a normal liver doesn’t have it) and, over time, this fat generates inflammation. In some patients, this inflammation leads to a deposit of scars; they form like wounds in the liver, which is what we call fibrosis. In this situation, the liver loses its elasticity; it becomes rigid, it hardens… everything changes and [this] leads to cirrhosis. That would be the progression from fatty liver and inflammation to scarring, cirrhosis and, later, liver cancer.
Q. This is the case when it’s caused by being overweight or obese, but does the development of liver cancer follow the same pattern in the case of alcohol or hepatitis?
A. For alcohol, the pattern is similar, because risky consumption also causes fat to be deposited in the liver. In viral infections, it’s different, because there’s no fat. But the viruses damage the liver cells and this injury causes inflammation. This chronic inflammation also causes scarring and can lead to cirrhosis.
Q. Is cirrhosis always the last stop in the evolution of the disease?
A. Cirrhosis is pretty much the last stop, but there are several phases. The first is also silent. As the disease progresses (because the factor that’s damaging the liver doesn’t go away), cirrhosis continues to progress. And there comes a time when the liver becomes very disorganized: the cells stop working properly and there’s also difficulty in the flow of blood. An increase in blood pressure is generated inside the liver — portal hypertension — which is what causes most of the serious complications of liver cirrhosis. And, as cirrhosis is a precancerous disease, some of these patients, over time, develop liver cancer.
Q. Does the liver have more recovery capacity than other organs?
A. It does, to a certain extent. If a person has a traffic accident and a part of their liver tears, they undergo surgery: the damaged part is cut out and, after a month-and-a-half, they have a normal liver again, because it grows (regenerates) and returns to the same volume that it intuitively had. The diseased liver is less able to do this, but what it can do is that, the sooner you detect liver disease, the more likely it is that by removing the cause, these scars will disappear… or, at the very least, their progression will be stalled. The more advanced the disease is, the less likely it is [to reverse the situation], but the progression can be stopped. And that’s what matters to us, because people die from the progression of the disease.

Q. Regarding the precursors of chronic liver disease: how has the profile of patients been changing? For example, with the new generation of antiviral drugs, people with hepatitis C can now be cured.
A. The profile has changed a lot. 15 years ago, more than 50% of the people we diagnosed with advanced chronic liver disease with cirrhosis had hepatitis C. Or hepatitis C combined with risky alcohol use. Today, hepatitis C has been reduced to a minimum. The great cause [of liver disease] at the moment is metabolic fatty liver, associated with being overweight or obese. And this will continue to increase in the future: all the forecasts are that severe liver disease due to fatty liver of the metabolic type will increase dramatically.
Q. Regarding obesity: there are studies that indicate that the consumption of fast food already causes more cirrhosis than alcohol. Do you think the population is aware of this situation?
A. I don’t think the public is conscious of this at all, [even though] this was demonstrated 30 years ago. The worse the type of food, the more sedentary the life, the sooner cirrhosis develops. For example, years ago in the United States, they began to diagnose cirrhosis in adolescents: adolescents who were subjected to a bad diet, fast food, many carbohydrates, many fats, with few vegetables, without exercising... They gained a lot of weight. By the time they reach 15, 17, 20, they already have cirrhosis.
Q. So it’s possible for an adolescent to develop cirrhosis?
A. Yes. Actually, nowadays, when we diagnose a case of cirrhosis in a person who is obese or overweight, when we ask them when they began to gain weight, most started at the age of 30 or 35. They develop the disease when they’re 60, so they’ve spent 25 or 30 years putting continuous stress on the liver. But if this stress is more intense — if life is even more sedentary, as is the case with many children and adolescents today — and the intensity of eating poorly and in greater quantities is higher, [along with other risk factors] such as alcohol consumption, the risk of liver disease skyrockets dramatically. We’re already beginning to see this in the United States, in the U.K. We’ll see it here [in Spain] in a short time. The average age of being diagnosed with cirrhosis due to metabolic causes — which is now around 60 — will progressively decrease.
Q. The population probably associates cirrhosis more with alcohol, with a serious problem of alcoholism. But you say that extraordinary consumption isn’t necessary to damage the liver.
A. Most of the people that we diagnose with alcoholic cirrhosis haven’t been drunk in their lives. What happens is that, of course, you can drink enough alcohol without getting drunk. Getting drunk is the acute effect of alcohol on the central nervous system, on the brain; but the chronic effect is the one that affects other organs. [The organ] that suffers the most from this is the liver: everything you drink, after a few minutes, ends up in the liver. So, the amount that’s already considered to increase the risk of chronic liver disease is relatively low: between 14 and 21 drink units [a week] in men (a drink unit being the equivalent of a small glass of wine). So, the man who drinks [two big glasses of wine a day] is already at an increased risk compared to the men who don’t drink at all. A small percentage of these people will end up developing liver disease. The more you drink, the more the risk increases. And if, in addition, you’re obese or diabetic, even more so. Women are more sensitive to the toxic effect of alcohol on the liver: the amount [that puts their livers at risk] is just seven units a week.
Q. What therapeutic treatments are there for liver disease?
A. We have three: one option is to remove the causative agent — if this is achieved, it’s very effective, especially if it’s done early. The second is to correct and try to prevent the complications that are occurring in the patient, such as infections. And the last alternative is the most drastic: a liver transplant. By trying to identify liver disease early, [we can avoid] the transplant option.
Q. What do you hope to find when this new tool reaches clinical practice? What’s the outlook in the coming years?
A. In the next few years, all the models indicate that there will be a very significant increase in liver disease — both cirrhosis and liver cancer — because, despite the fact that hepatitis C has decreased dramatically, a major cause such as alcohol [consumption] hasn’t declined. It actually increased during the pandemic and has shown no signs of slowing down. And the other cause is related to the obesity epidemic, which is very difficult to stop.
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition








































