Breast cancer screenings with artificial intelligence support detect 20% more tumors
A study of 80,000 women finds that using AI to help read mammograms is a safe approach and reduces the workload of radiologists by almost half
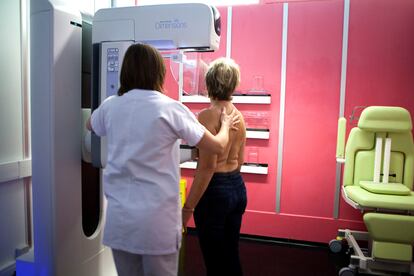
With cancer, time is health. The earlier a tumor is detected, the better: the higher the chances of treatment and cure. Therefore, early detection tests have become an ally in increasing survival and tackling nascent tumors as soon as possible. For instance, scientific literature estimates that population-based screening by mammogram reduces breast cancer mortality by 20%, and this decline may be even more pronounced if screening tests and the analysis of results are refined. Artificial intelligence (AI) has already crept into this field and, according to a Swedish study involving 80,000 women published in The Lancet Oncology, breast cancer screenings that are supported by artificial intelligence systems have detected 20% more tumors than those that follow the traditional methodology, which involves a double review carried out by two radiologists. Preliminary results from the research, which is still ongoing, conclude that using AI to analyze mammograms is safe and nearly halves the workload of radiologists.
In breast cancer screening, mammography analysis is usually done by two independent radiologists, as recommended by European clinical guidelines. If they do not agree on the reading, they usually agree on the discrepancies or allow the most aggressive decision to prevail. For example, between not calling the patient or referring them for more tests, the second option is chosen. One study suggests that this double-read technique will detect 0.44 more tumors per 1,000 people screened than a single reading. However, the specialist’s eye is not infallible either: scientific literature estimates that up to 25% of mammographically visible cancers are still not detected in screening and there is already research suggesting that the accuracy of AI may be similar or even superior to that of radiologists.
To verify whether AI-assisted screening is indeed inferior to standard methodology, the Swedish study recruited more than 80,000 healthy women who participated in population-based breast cancer screening between April 2021 and July 2022. The researchers divided them into two groups: the control group, whose mammogram analysis was to follow the standard double-reading procedure; and the intervention group, which would have the initial help of an AI system to analyze the medical tests — and catalog their degree of risk — before being reviewed and interpreted by one or two radiologists (one, if the risk marked by the AI was low and two if the mammogram was at the high risk threshold).
“There were no false positives among that 20%. They are confirmed cases of cancer.”Kristina Lång, Lund University
The analysis of the medical tests resulted in the detection of cancer in 244 women in the AI-supported group and another 203 in the control group. That is: incorporating AI systems in the analysis allowed 20% more tumors to be diagnosed. “With AI-assisted screening, we detected 20% more cancers than with standard screening (double reading without AI). There were no false positives among that 20%. They are confirmed cases of cancer. AI-backed detection did not lead to an increase in false positives, which is very good,” said Kristina Lång, a researcher in the Division of Diagnostic Radiology at Lund University (Malmö, Sweden) and one of the study’s authors. The false positive rate of all tests performed was similar at 1.5% in both groups.
Lång explains that these AI tools are used as “a detection support in which suspicious findings are highlighted in the images” and that “can help the radiologist detect more cancers that might have been missed.” “AI can also be used to classify screening into low- and high-risk groups. A test result classified as high-risk may alert the radiologist to suspected malignancy. There is a synergistic effect when human and artificial intelligence come together,” the Swedish scientist says.
Reduce workloads
The preliminary results of the study open the door to incorporating AI as a tool to help in the interpretation of mammograms, because apart from increasing the detection of cases, it could serve to optimize the role of radiologists and reduce workloads. The researchers recall that, although the European authorities recommend the analysis of mammograms with double reading by two radiologists, that implies “a huge workload for specialists and can potentially increase false positives.” And these drawbacks are not trivial, they point out, considering the shortage of radiologists who are skilled in reading mammograms. “In addition, despite the double reading, some cancers can be missed and diagnosed as interval cancers [those detected between two screening tests],” the scientists say in the article.
In fact, the Swedish researchers need 100,000 participants in this study and two years of follow-up to evaluate whether the use of AI to support the analysis of mammograms also reduces interval cancer, which usually has a poorer prognosis. A high rate of interval cancer is an indicator that the early detection program is not serving its purpose, as it fails to diagnose that tumor early. “We hypothesize that AI can lead to a better screening program with fewer interval cancers. Since our early results show that we detected more cancers, there is a possibility that we may have a better and more efficient screening program,” Lång said.
“AI should be a tool for the radiologist and not the other way around.”Kristina Lång, Lund University
The workload of radiologists can get very heavy and that affects their ability to analyze. Director of the Radiodiagnosis and Breast Cancer unit at the Reina Sofía Hospital in Córdoba and breast specialist of the Spanish Society of Medical Radiology (SERAM), Marina Álvarez admits that in a day of reading mammograms, a radiologist can analyze more than 100. “And most of them will be normal and that, together with the radiologist’s fatigue, means that some tumors can go unnoticed,” the specialist explains.
Álvarez, who has not participated in the study, calls the research “very good and methodologically impeccable” and highlights the advantages of incorporating AI as a support in analyzing mammograms: “AI has the ability to stratify studies according to risk, save the radiologist time, and improve the specialist’s performance.” In fact, the study confirms, indeed, that in the intervention group, reading mammograms was reduced by about 44%. “These systems can classify the study according to the ability or not to have cancer because it can detect nodules, calcifications... This risk stratification, which cannot be done by a radiologist in such a short time, serves to treat each risk group differently: most are at low risk, only 30% are at intermediate-high risk and only 3% are at high risk; and in that 3% is where we find 70% of cancers. That’s why stratification is so important,” explains Álvarez. With that filter in place, the radiologist can do a faster analysis of low-risk mammograms and focus more attention on the study of those that are high risk.
Josep Munuera, head of the Diagnostic Imaging Service at the Sant Pau Hospital in Barcelona and an expert in digital technologies applied to health, also says that this study, in which he has not participated, has a “very good” design and reinforces “expected” results. “There are algorithms with high detection rates that, if combined with the results the human gets, improve the human’s rates as well.” The doctor also stresses the importance of the human reader being a radiologist with a lot of experience, as they were in this study.
In the intervention group, 75% of the tumors detected were invasive (meaning that they are more widespread) and 25% in situ (small lumps in the breast that may be harmless). In the control group, 81% were invasive and only 19% in situ. The researchers admit that increased detection of tumors in situ “could be concerning in terms of overdiagnosis” because these kinds of lumps may never progress to cancer or may even go away on their own, and risk embarking the patient on more potentially unnecessary cancer tests or therapies. Álvarez, however, qualifies this point: “There are people who may think that 25% of tumors detected in situ is a high percentage because not all end up being cancer and would be treated much more [than necessary], but we cannot differentiate which will advance, we have no way of knowing if it will advance or stay as it is.”
The radiologist is in charge
Faced with this dilemma, Munuera adds, the key is the radiologist. “These lesions, even if detected, are so subtle that they may end up progressing to cancer. The radiologist will make an interpretation of the image and decide,“ he says. But he adds: “Introducing AI tools involves seeing 100% of these tumors and you will have to make a decision about them. That’s the next step, let’s see what we do with them.” Munuera celebrates, in any case, that the reduction of the workload in the readings can favor “a very positive redistribution of workflows to increase the radiologist’s reading speed and reduce the waiting list for mammogram analysis. It could also mean being able to do more interventional treatments and complementary tests” that are associated with the results of these screenings.
The Swedish researchers strongly emphasize that AI is a tool available to the radiologist, but the specialist has the last word. “AI should be a tool for the radiologist and not the other way around,” says Lång. Nor are these systems unambiguous: “Based on retrospective studies, we know that AI missed some types of cancer. AI can also be overly sensitive and points to many findings that we, as radiologists, can easily determine as normal. Therefore, the radiologist is essential to make the final decision if a screening exam is normal or if the woman should be called back for further study.”
Despite the favorable results of this study, there is still some way to go before we see AI replacing reading done by a human. “European guidelines do not currently recommend that AI should replace a human reader,” says Lång. But studies like theirs underpin the evidence to move down that path. Always, of course, under the supervision of the radiologist.
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition








































