How breast density influences breast cancer risk: ‘It can hinder diagnosis’
A dense breast can mask tumors in mammograms. But a study shows that few women perceive it as a risk factor for developing cancer
There are genetic mutations that predispose a person to breast cancer. Other risk factors include a family history of the disease, obesity and unhealthy habits like smoking. While most people know about these risks, having dense breasts goes under the radar. A study published in the journal JAMA revealed that few women perceive this variable as a risk factor and know little or nothing about it. Breast density has nothing to do with breast size; it pertains to the internal composition: that is, breasts with more fibrous and glandular tissue than adipose. For women with extremely dense breasts, that difference elevates the risk of developing a tumor, making it up to four times higher.
Breast density is not visible to the naked eye. Only a mammogram can reveal it, explains Javier de Santiago, the president of the Gynecologic Oncology Section of the Spanish Society of Gynecology: “The breast is made up of fibroglandular tissue and fat. When the former predominates, we speak of a dense breast. But this has nothing to do with size. In fact, generally, smaller breasts are denser.” Younger people are also more likely to have dense breasts. However, breast density is not a fixed characteristic; it can change over the course of a woman’s lifetime as a result of different factors, such as chronological age, the scientists explain. According to de Santiago, who is also the director of Gynecology at MD Anderson, 50% of women have dense breast tissue.
According to the JAMA article, a qualitative study of women aged 40 to 76 years, when comparing various risk factors and the risk associated with breast density, 93% of participants felt that family history of breast cancer posed the greatest risk, and 65% believed that being overweight or obese posed a greater risk than breast density. “Among 61 women interviewed, few women perceived breast density as contributing to their risk of developing breast cancer,” the researchers noted. But just because this variable is not well known among patients does not mean that the scientific community is unaware of it or that it is not taken into account in examinations.
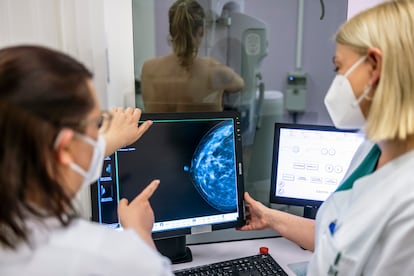
One of the reasons for the greater danger is that a dense breast can mask a tumor in mammography, says Marina Alvarez, the spokesperson for the Spanish Society of Medical Radiology: “Mammography is a variant of X-ray. The image is in black and white; the fat is seen in black and both the glandular tissue and the tumor are in white”. Because they are the same color, a dense breast can make a malignant nodule go unnoticed. “It can make diagnosis difficult. The more fibroglandular tissue there is, the more difficulty we have in seeing a lesion in the breast,” the radiologist admits.
Breast density is also a risk factor in itself, although the scientific community is not sure why that is the case. According to Xavier Castells, the head of Epidemiology at Barcelona’s Hospital del Mar, that is probably because “the percentage of breast tissue in the chest is higher and there is a greater possibility of a tumor. “It has been said that a woman with a higher breast density is twice as likely to have cancer as one with less dense breasts,” says the epidemiologist.
Interactions between risk factors
The experts point out that there are different levels of density. In fact, the JAMA study warns that dense breast tissue is associated with a 1.2 to four times greater risk of breast cancer, depending on the degree of density. Radiologists measure all of this, assures Alvarez: “The information from a mammogram is very standardized and the first thing we look at is density, but there are four different types [A, B, C, D, from the lowest to highest level of density]. We also look to see if there are any findings, which can be a nodule or a calcification, and describe them. We use a tool to classify the risk of malignancy: level one [means] no malignancy, [while] level five is highly suspicious and level six is confirmed malignancy, for example.”
In any case, breast density alone cannot be interpreted as an isolated risk factor. It must be contextualized by considering other risk variables, such as age, family history and genetic predisposition. Everything counts, and it adds up. “Patients should not be alarmed. It is not a matter of reading mammograms now. The ideal thing is to study which other factors may also exist in order to conduct specialized follow-up,” says De Santiago.
According to Castells, age and the interactions between different risk factors are important: “If you have a benign proliferative lesion, in four years, the risk of cancer is more than double that of women who do not. And if you add in family history, the risk is seven times higher. And if you also have dense breasts, the risk is 15 times higher,” he explains. But, he warns, this level of risk must also be contextualized: “The woman with the highest risk has a 7% [risk]. Ninety-three percent will not get cancer. In other words, the probability is low.”
Castells says that having BRCA gene mutations, which are closely linked to cancer risk, is a very important factor. Likewise, depending on age and family history, having two or more risk factors, “can also weigh more heavily than any other factor,” he observes. A history of previous benign lesions is another risk factor, but it depends greatly on the type of lesion. “Breast density is also a factor, because it can double the risk, but ultimately the absolute risk is not very high,” he argues.
More personalized screening
The role of breast density has opened a debate on traditional breast cancer screening’s efficacy in patients with dense breasts. In Spain, early detection testing is in place for women between 50 and 69 years of age, who are encouraged to have a mammogram biannually, but experts admit that perhaps a more specific follow-up would be appropriate for this group. “In very dense breasts, screening should be done with MRI, not mammography. That would help detect more tumors and there would be fewer interval carcinomas [the name given to tumors diagnosed in the period between screening rounds],” Alvarez says. In these cases, an MRI is a more reliable method, but it is also more invasive because it requires administering contrast intravenously and there is also a risk of false positives, along with all the stress and impact that can cause for the patient.
Alvarez says that this topic is being debated in Europe, and there are different proposals on the table. One suggestion is to alternate between mammography and contrast-enhanced MRI scans at each round of screening. Another option is to use a different technique like tomosynthesis, which instead of taking a type of photo, as mammography does, records numerous photos in millimetric slices: “For the patient, it is the same as a mammogram: the sensation is the same, and it takes the same amount of time.” A recent study concluded that this technique “is especially beneficial for women with denser breast tissue.”
For now, however, the protocol has not changed. “Generally, women with dense breasts are treated the same as everyone else. No other tests are done. Usually, when a woman is referred for complementary tests, something has been found; it’s not just because of breast density,” the radiologist explains. Indeed, Castells believes that the approach for women with dense breasts or other risk factors must change and move toward “personalized screening.” He observes that “not everyone has the same risk and those who have more [of a risk] should be screened more intensively.”
The epidemiologist adds that an individual decision, a specific case to be assessed between the physician and the patient, is not the same as population screening, which must be guaranteed for an entire target population: “We have the infrastructure, but the problem is that radiologists have to be trained to know how to read it and the response takes longer. We are now calling five million women in Spain every two years. 30% [of them] have high-density [breasts]. And getting 1.5 million women in for a tomosynthesis is not easy.”
Communicating with patients
In some thirty U.S. states, healthcare professionals are required to inform patients of their breast density when they undergo a mammogram. The experts we consulted admit that this is not usually done in Spain. As to whether it would be a good idea to convey that knowledge to the patient, Castells says that “the easy answer is…yes,” but this information must be accompanied by something else, he adds. “At the same time that you tell them that they have more risk, you should offer them a way out, a proposal. What do you [say to] them?”
Montserrat Rué, a researcher at the Department of Basic Medical Sciences at the University of Lleida, advocates improving communication with patients. “Women want to know; they appreciate that you’re giving them information. And having a risk factor does not mean that something will happen to you. It is when several factors are combined that closer monitoring is required,” Rué points out. Her research has studied women’s perceptions of screening and its potential risk. The scientist admits that there is a tendency to “overestimate the risk and underestimate the consequences of diagnostic tests,” such as overdiagnosis, false positives or false negatives.
Rué advocates shared decisions between doctors and patients, creating “instruments and materials that explain the risk and help people…understand” this danger. She adds that “in general, people think that we are at greater risk of these diseases than we really are. A woman’s lifetime risk of breast cancer is 12%. The fear that comes from having [people] close to us who have had [the disease] is contagious.”
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition








































