Despite its drawbacks, robotic-assisted surgery is on the rise
These expensive systems offer a very sophisticated scalpel that doctors do not need to hold in their hands. Their use is growing in countries like Spain
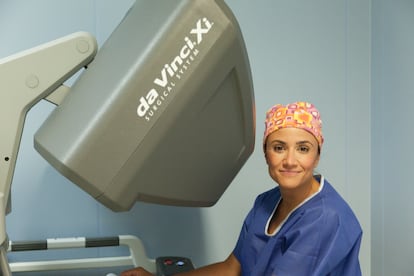
Robotic-assisted surgical systems were introduced to Spanish hospitals in 2005. Since then, they have been used to operate on more than 65,000 people. This figure does not include trauma operations (knee, hip and spine), which are increasingly performed via robot-assisted surgery.
The best-known and most widely-installed system – and until recently, the only one that existed – is the Da Vinci clinical robot, developed by the American company Intuitive Surgical. However, in 2022, the Barcelona Puigvert Foundation began to operate with HUGO.
“At the moment, HUGO only has certification for urology,” says Dr. Salvador Morales-Conde, president of the Spanish Association of Surgeons, “but the company that markets [the system] is pending approval for general surgery.”
These systems do not operate directly: they are tools used by human surgeons. The clinical robots offer a very sophisticated scalpel that a surgeon does not need to hold in his or her hands – it incorporates a camera, tweezers, a needle and other instruments required in a surgical intervention.
When you have been operating for four, five hours in the same position, with stiff shoulders... there comes a moment when you can’t take it anymore and may even have small hand tremorsDr Belén Cuesta, Rey Juan Carlos Hospital in Madrid
“In the past, we operated with open surgery,” explains Dr. Ana Belén Cuesta, a gynecological surgeon at the Rey Juan Carlos Hospital in Madrid, who has been operating with the assistance of a robot for five years. “That means we had to open the abdominal cavity. Then, we started using laparoscopy to make the surgery less invasive. When the robot came up, I had a lot of doubts, because I didn’t see any advantages to it. But since I’ve been operating with it, I’ve discovered that it does make up for the shortcomings of laparoscopy.”
Laparoscopy is a type of surgical procedure that allows access to the inside of the abdomen and pelvis without having to make large incisions in the skin. Tubes containing surgical instruments and cameras are subsequently inserted. Laparoscopy is also known as minimally-invasive surgery – scars are much smaller, postoperative pain is reduced and recovery is faster.
Robotic surgical systems manage to do the same thing, but the difference is that surgeons do not have to hold and move the tubes themselves – they can operate the device from a console.
“With the robot,” continues Dr. Belén Cuesta, “we see the interior of the abdominal cavity in 3D, whereas laparoscopy only permits two-dimensional vision. This is important, because we can appreciate the structures of the organs much better. In addition, laparoscopy uses rigid instruments – it is as if we have to operate with a wrist that has no mobility. The robot’s instruments, on the other hand, can move in all directions. Thanks to this, we can access smaller, difficult-to-access spaces.”
“The operations we do are usually long, especially oncological ones. And in a laparoscopy, when you have been operating for four or five hours in the same position, with stiff shoulders... there comes a moment when you can’t take it anymore and you may even have small tremors in your hands. The robot prevents this by stabilizing the instruments.”
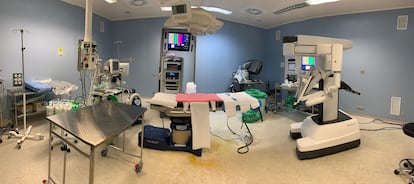
There are obvious advantages to robot-assisted surgery. But not everything is idyllic. For starters, there is a high price tag. A Da Vinci robot costs between €1.5 million and €2.5 million. In addition to that, a hospital must pay a minimum of €140,000 per year for maintenance.
The defenders of this technology often argue that, despite the high purchase and maintenance prices, robot-assisted surgery has advantages, such as shorter duration of operations or shorter recovery time for patients. But published research does not confirm these facts. In June 2021, the Annals of Internal Medicine published research on 50 studies looking at nearly 5,000 robotic surgery patients. The authors concluded that there is no difference between robotic-assisted surgery and laparoscopy in the probability of complications, even in the long term. They also point out that, for example, in gynecological surgery, robotic operations increased their duration by 13% compared to laparoscopic ones. Furthermore, a study by researchers from the University of California at San Diego, published in March 2022, reports that after 10 years of using a robot as a surgical assistant in their hospital, patients operated on remain hospitalized for longer than those who received laparoscopy.
Technical failures can also not be ignored, because, after all, machines are fallible. Another study published in 2016 analyzed the technical problems found in robot-assisted surgeries after 14 years of use: in the cases analyzed, they found that 10.4% of the surgeries had to be interrupted due to some sort of technical failure that involved restarting the system, the robot needing to be reprogrammed, or continuing with the surgery by conventional means.
However, according to Dr. Julio Mayol, president of the Spanish Society for Surgical Research, “Robots can help us reduce the variability of practice and increase the safety of surgery. It is true that their price is high, but that is going to change. When Da Vinci’s patents end, there is going to be more competition.”
Dr. Mayol acknowledges that the current situation is not ideal: “It is debatable how [these machines] are being used. We should establish a group of patients with similar characteristics to allow us to understand how this technology can be implemented in the best possible way. For that, we would need to work as a network.”
The 65,000 operations carried out in Spain with robots over the past 17 years represents a small percentage of the 3.6 million operations done during that time. But the drop in the price of robots and the arrival of new models from other companies will make their implementation jump in the coming years.








































