Covid vaccines saved nearly 20 million lives, study finds
Most of the deaths averted were in developed countries, according to the research, which used mathematical modeling to calculate the global impact of vaccination

Margaret Keenan, a 90-year-old British woman, received the first Covid-19 vaccine outside of clinical trials on December 8, 2020. A study published on Thursday in the medical journal The Lancet has modeled what would have happened without Covid-19 vaccines – in other words, how many lives did they save. According to the research, the vaccines prevented 19.8 million deaths, the equivalent of the entire population of Ecuador. But the study also confirms the vaccine inequality between poor and rich countries.
It is not easy to determine the impact of the vaccines against Covid. Vaccine trials showed that they were between 60% and 90% (depending on the kind) effective at reducing the risk of serious illness. But how many deaths have they prevented? It’s difficult to know. To estimate the number, one needs to imagine two parallel worlds – one that has vaccines and one that doesn’t – and see where more people died from the disease. Since such a comparison is impossible, one has to turn to mathematics and modeling. And that is exactly what researchers at Imperial College London (ICL) did for their study in The Lancet. Using demographic data, including comorbidities, from 185 countries, as well as information on health infrastructure, the previous infection rate, vaccination rate and even types of vaccines, they modeled the impact of Covid-19 vaccines from December 8, 2021, when Margaret Keenan was vaccinated, until just a year later.
If the model only takes into account the statistics on the number of Covid-19 deaths, the vaccines would have prevented the death of 14.4 million people in the 185 countries studied. But not every country has reliable official data, and often the figures are underreported. To address this problem, the researchers compared the number of deaths from all causes in 2020 and 2021, with the figure in pre-pandemic years. The excess mortality was attributed to the virus.
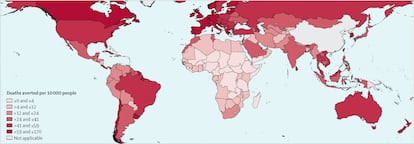
According to the model, the direct benefit of the vaccine i.e. immunization prevented most of the 20 million deaths. But the study found vaccines also saved lives by building herd immunity and relieving the burden on the health system. The impact of vaccination only began to be seen in mid-2021, when most developed countries had fully immunized a large percentage of the population, and also lifted restrictions. The research also highlights the huge divides in the vaccination campaigns of different countries.
“Of the almost 20 million deaths estimated to have been prevented in the first year after vaccines were introduced, almost 7.5 million deaths were prevented in countries covered by the Covid-19 Vaccine Access initiative (COVAX, which aimed to provide vaccines to low and middle-income countries],” said Oliver Watson, the lead author of the study, in a statement.
COVAX, which was supported by the United Nations, the World Health Organization and the vaccine alliance GAVI, aimed to vaccinate at least 20% of the population of the hundred poorest countries by the end of 2021. The WHO was even more ambitious, raising that goal to 40%. But the reality has been very different. For example, the first Covid vaccine arrived in Burundi 10 months after it arrived in the United States. Meanwhile, only 0.07% of the population of the Democratic Republic of Congo had received one dose at the end of 2021, while the US had bought enough vaccines to vaccine its population three times over.
Time has also played a key role. Europe, the United States, Canada and other developed countries started the vaccination drive much earlier than the rest of the world and on a massive scale. “This meant that more deaths were averted as transmission increased in 2021, either due to the easing of non-pharmaceutical interventions or the arrival of the more transmissible delta variant in the second half of the year. If vaccination had occurred before and prior to the arrival of this variant in low-income countries, more lives would have been saved,” said Watson. “If the targets set out by the WHO had been achieved, we estimate that roughly one in five of the estimated lives lost due to Covid-19 in low-income countries could have been prevented.”
The study also confirmed that not all vaccines are equally effective. In countries that primarily used vaccines based on RNA technology (Moderna and Pfizer), the number of lives saved was greater. But in addition to being more effective, especially against the delta variant, the vaccines require stricter storage and transportation conditions, which has meant that they have had little uptake in low-income countries, already lagging behind in the vaccination drive. The model also detected many COVAX countries lacked the infrastructure to carry out the immunization drive, and that the population was relatively less willing to get vaccinated.
“Our study demonstrates the enormous benefit that vaccines had in reducing deaths from Covid-19 globally,” said Professor Azra Ghani, head of Infectious Disease Epidemiology at Imperial College London, in a statement. “Whilst the intense focus on the pandemic has now shifted, it is important that we ensure the most vulnerable people in all parts of the world are protected from ongoing circulation of Covid-19 [...] Ensuring fair access to vaccines is crucial, but requires more than just donating vaccines. Improvements in vaccine distribution and infrastructure, as well as coordinated efforts to combat vaccine misinformation and improve vaccine demand, are needed. Only then can we ensure that everyone has the opportunity to benefit from these life-saving technologies.”








































