The lethal kiss between cells that can trigger cancer
Scientists discover how some tumors put the body’s immune defenses to sleep
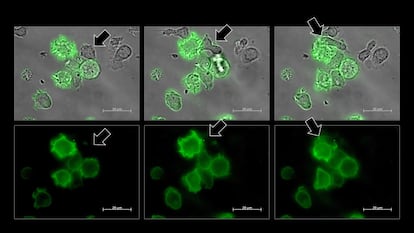
According to scientists from Ottawa Hospital in Canada, cancer can begin in the body due to what they call “a kind of kiss” between multiplying cells and the body’s immune defenses.
As the researchers explain, some white blood cells, such as NK cells (Natural Killers), are capable of recognizing and killing cancer cells.
However, in some blood tumors the defensive NK cells become dormant after interlocking with the cancer cells. This renders the NK cells unable to kill the cancer cells, clearing the way for cancer to develop.
Kissing between white blood cells and other cells is common, explains Italian immunologist Michele Ardolino.
The phenomenon is called trogocytosis, from the Greek trogo, meaning to nibble or gnaw. The defensive cell comes into contact for a few minutes with another cell - which may, for example, be cancerous or virus-infected - and steals a fragment of its membrane. “My hypothesis is that immune cells have evolved these mechanisms to better sense and be influenced by their environment,” says Ardolino, who leads the Ottawa team.
Making proteins takes time and energy, so white blood cells steal them from their neighboring cells to regulate their own behavior in response to the outside world - when infected by a virus, for example. “It’s like if you’re entering a baking competition and you’re late for the competition,” explains Ardolino. By way of comparison, he says that “you could make your own cake batter,” but it would take less energy to “simply take a pre-made one from the fridge.”
The kiss between a cancerous cell and an NK cell is a unique case of trogocytosis. NK cells are extraordinary cancer killers, but a protein called PD-1 prevents them from functioning properly. In the beginning, Ardolino’s team didn’t understand where this protein came from. As they later discovered, “NK cells don’t make their own PD-1 protein, they steal it from cancer cells.” During the kiss, the NK killers steal a fragment of tumor membrane that is riddled with these numbing proteins.

The Italian immunologist says it’s clear some cancers take advantage of trogocytosis to override the human body’s defenses.
The discovery is the result of a multitude of experiments on mice with leukaemia and was published in the journal Science Advances on Wednesday.
Other cancer-killing white blood cells, the T cells, do produce their own PD-1 protein, a natural deterrent that helps prevent them from attacking other normal cells in the body. As Ardolino points out, there are already drugs that target this PD-1 protein. Indeed, some of them are among the biggest moneymakers in the world, such as Keytruda, a drug from the US pharmaceutical company MSD that is indicated against melanoma, certain lung cancers and some other tumors. Sales of Keytruda were close to €16 billion in 2021, according to an analysis by UK company Evaluate Vantage. Opdivo, another similar anti-tumor drug Made by US-based Bristol Myers Squibb, had sales of €7 billion.
By inhibiting PD-1, these drugs release the natural brakes and trigger the ferocity of T-cells against cancer cells. Japanese immunologist Tasuku Honjo won the 2018 Nobel Prize in Medicine for discovering the PD-1 protein more than a quarter of a century earlier and learning how to inhibit it in order to fight cancer. The US approved the drug Keytruda in 2014 and authorized Opdivo the following year. Immunotherapy, in which the human body’s natural defenses are stimulated in an attempt to eliminate a patient’s tumor, was born.
In some countries these treatments can cost more than €50,000 per year per patient. Tasuku Honjo himself lamented these prohibitive prices in an interview with EL PAÍS in 2019. “It’s always the same problem with any drug. It would be better if it were cheaper, so that everyone could benefit. Even penicillin, when it came on the market, was very expensive. And then it became affordable for everybody,” he argued.
Ardolino’s team first noticed four years ago that these blockbuster PD-1 inhibitor drugs, originally designed to stimulate T cells, also stimulated NK cells. Immunologist David Raulet of the University of California, Berkeley, was involved in that work. “The field of cancer immunotherapy has focused on mobilizing T cells, but we believe that NK cells also play an important role,” said Raulet at the time. Some tumors do not respond to current treatments that activate T cells, but they could perhaps succumb to an attack by suitably equipped NK cells.
Michele Ardolino believes his new discovery will help refine the therapies to fight cancer. As each cancer is unique, so is each person’s immune system. Ardolino’s dream is that, when a cancer patient arrives in hospital, doctors will be able to biopsy the patient to not only determine the specific mutations of their tumor, but also obtain a very detailed profile of how the patient’s immune system responds. Each patient could then be offered a more targeted immunotherapy, possibly even tailored to the cancerous proteins stolen by their white blood cells.








































