Medicine, not science fiction: The medical breakthroughs on the horizon
The coming years will see the consolidation of precision therapy in all of its disciplines. There will be individualized treatments for each person

The essence of science is, in the words of astronomer and science communicator Carl Sagan, that it is a “self-correcting process” all of the time. Writing in his book Cosmos, he said that “new experimental results and new ideas are constantly solving old mysteries.” Biomedical research is a good example of this. After the setback of the pandemic, which forced researchers to focus their efforts on combating the coronavirus, the scientific community has stepped up the pace in order to make up for lost time.
Diseases – including Covid-19 and more – are still being targeted. The coming years will see the consolidation of precision medicine in all of its disciplines, according to the experts. It will all move in the same direction: individualized therapies, personalized approaches and research aimed at the particularities of each person. Every patient is a world to be explored.
The paradigm shift has already happened, and technology – thanks to tools including artificial intelligence, nanomedicine and bioinformatics, is now at the disposal of the scientific community to bring it into practice.
On the table already is promising research: viruses to help kill bacteria that are resistant to antibiotics, and trials to create new vaccines that combat cancer. There is also the consolidation of gene editing, such as the famous CRISPR technology, as well as another technique that repairs errors in DNA without modifying their structure. All of this, and more, is underway. There is no time to lose.
1. The fight against antimicrobial resistance
The therapeutical arsenal against bacteria is drying up. Microbes have learned to evade antibiotics and are starting to show a resistance that endangers the life of a person due to a simple infection. Antimicrobial resistance has become a major global problem – a budding pandemic. “We have to be ready,” warns Jesús Oteo, scientific director for infectious diseases at Spain’s Center for Biomedical Research Network (CIBER). To do so, a network of countries has been created in a bid to strengthen epidemiological monitoring. How? By integrating genomic sequencing and bioinformatic analysis of the available data to create algorithms and predict the behavior of infections.
Innovation is also needed when research into new antibiotics is unlikely – and unprofitable for the pharmaceutical industry – and the main assets with antimicrobial capacities are limited. “They are betting on the combination of existing drugs with substances that inhibit the enzymes of the bacteria that create resistance,” explains Oteo. Also underway are so-called bacteriophage, viruses that infect bacteria and kill them. “Nothing is available commercially still, but in testing there are cocktails of bacteriophage that work,” he adds. In Spain, cases of resistant infections due to the Pseudomonas aeruginosa and Mycobacterium abscessus bacteria have been treated in this way, and there is testing underway for Staphylococcus aureus, which causes skin and respiratory infections as well as food poisoning.

2. Consolidation of precision cancer treatment
If immunotherapy, which trains the immune system to kill the tumoral cells, represents the great cancer revolution of the last decade, the coming years will consolidate it. Josep Tabernero, director of the Vall d’Hebron Institute of Oncology (VHIO) in Barcelona, says the first step is to start applying the treatment to earlier stages of cancer instead of advanced cases, as it is now.
And in the search for new drugs, anti-cancer vaccines are starting to gain traction again. “The vaccine is meant to help reinforce and re-establish the properties of the immune system,” explains Tabernero. Research is even pointing in the direction of personalized vaccines. “They used to be the same for everybody, but now the idea is to analyze the tumor, see what antigen it has developed the most, and prepare ad hoc immunization shots,” he explains.
Tabernero says that the coming years will see great growth of CAR-T therapy, which extracts blood from the patients, selects their T-cells (a type of white blood cell) and modifies them genetically in the lab to increase their ability to recognize cancer cells. For now the technique only works with a few forms of blood tumors.
The VHIO expert is also looking at the potential of so-called TIL or tumor-infiltrating lymphocytes. This type of immunotherapy is similar to CAR-T, but instead of activating the T-cells of the immune system, it specifically targets the lymphocites that are already in the tumor (TIL): “It involves resecting a tumor fragment, separating the TIL cells [which are able to detect the antigens on the tumoral cells], then in the lab we make then expand ex vivo and multiply, then we infiltrate them again.” The VHIO is already testing this technique on melanoma.
Precision oncology is also reaching diagnosis and early detection. Liquid biopsies, which are already being performed at numerous health centers to detect certain types of tumor through blood tests, will continue to improve. “We are assessing patients and changing treatments on the basis of liquid biopsies,” says Tabernero. “And we also want to use them to escalate or de-escalate drug dosage: depending on what the liquid biopsy says, you could decide to stop chemotherapy or, in high-risk patients, administer it preventively.”
Anna Bigas, scientific director for the Madrid-based cancer research center CIBER, talks about the “virtual twins” involved with computational medicine: “It’s about doing a really comprehensive genomic of the tumor and share data so we can create virtual twins of the tumor that let us predict how the patient is going to evolve, their treatment, their prognosis,” she explains. Digitalizing images and using artificial intelligence will also facilitate predictions, adds Bigas.
3. The power of nanotechnology
Human cells are measured in microns, one thousandth of a millimeter. They are invisible to the eye and operate at nanoscales, requiring special tools to handle them. Nanomedicine has been around for years, and the coronavirus pandemic has been a good opportunity to test its maturity. RNA-messenger vaccines against Covid-19, which teach cells to make a protein that triggers an immune response in the body, were achieved because RNA is encapsulated in lipid nanoparticles, notes Laura Lechuga, head of bioengineering, biomaterials and nanomedicine at CIBER. “With these vaccines, a whole world of possibilities is opening up: you can encapsulate RNA to enter the cells and give them clear instructions.” Nanomedicine contributes the vehicle.
Research is advancing on several fronts, from diagnosis to slow-release medication. “The active ingredient reaches the specific spot and the amount required is a lot less than if you were to swallow it. This makes it more efficient and less toxic,” adds Lechuga. Nanoparticles as a form of treatment are another promising line of investigation. “One example would be nanoparticles that can penetrate tumoral cells, and when you administer radiation from without, they start to vibrate and kill the malignant cells.” Lechuga says that nanomedicine will level the playing field for diagnosing certain diseases. It will make it more accessible. For instance, through implants to monitor biological parameters. “The idea is that through urine, blood or sweat samples, in 10 minutes you will know if you have something, and how far along it is.”

4. Perfecting gene editing
The CRISPR technique, something akin to a pair of molecular scissors (Cas9 protein) that cut a portion of DNA to edit or repair it, has revolutionized the field of genetic engineering. “It’s changed our lives,” says Almudena Fernández López, a researcher specializing in rare diseases at CIBER . Researchers are now able to slice a precise spot of the genome of any cell and manipulate it. This technique has not yet reached doctors’ offices, but there are studies underway involving blood-related illnesses and a type of blindness known as Leber congenital amaurosis.
Though promising, CRISPR has its limitations and there are significant ethical implications as well. Gene therapy in adults is allowed, but not in embryonic stages. “The problem is that you’re not in control of 90% of events,” notes Fernández López. There could be cuts in undesired areas of DNA, or dangerous mutations.
But gene editing continues to evolve, seeking vehicles to take these tools to the cells and developing ever more precise editing techniques. “The base editing developed by the California chemist David Liu is key,” says Fernández López. “It does not cut the DNA but works more like Liquid Paper. It cleans the patient¡s erroneous base and puts a new one in place. This prevents undesired repairs.” These techniques offer hope but there is a limit. “The computer can take it all, but when we are faced with biology, we will find out limitations: there are parts of the genome that we cannot reach.”
5. The role of the microbiome
It’s something like an invisible organ made up of “billions of tiny life forms: microbes and their relatives” explains the American microbiologist Martin J. Blaser in his book Missing Microbes: How the Overuse of Antibiotics Is Fueling Our Modern Plagues. And there is a clear role for the microbiome: “It keeps us healthy.” Each one is different depending on the individual, and finding common patterns is proving complicated, admits Francisco Guarner, former scientific president of the International Human Microbiome Consortium. “We already understand that the presence of bacteria and other microorganisms has a functional implication in our bodies, but we got lost when it comes to how to generate diagnostic elements and how to take action. We have probiotics, prebiotics, stool transplants, but no great results for big problems” such as cancer, obesity or mental health disorders.
But research into how bacteria affect disease and how to modulate them marches on regardless. “The future lies in diagnostic tests,” says Guarner. A team led by Núria Malats at Spain’s National Center for Cancer Research has identified a molecular signature of 27 microorganisms in stool samples that might predict who is at high risk of developing pancreatic cancer.
The other major challenge is finding a pattern of ideal conditions in the microbiome. The Consortium wants to gather data from a million individuals in order to find a pattern that might help detect anomalies.
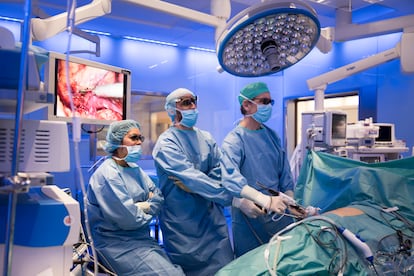
6. Robot-assisted surgeries
The robot known as Da Vinci has made a big impact on surgeons. With its articulated arms and 3D-vision camera, it has become one of the best tools to carry out delicate surgeries in the least invasive way possible. This model was the first of the robot-assisted surgery revolution, but more are on their way. “In 10 years, the robots will be closer to the concept of an independent robot. They will depend on the surgeon, but they will issue alerts, warnings to help them, such as not to cut into an artery or vein for example,” says Alcaraz.
Also on the horizon is extracorporeal robot-assisted surgery, i.e. surgeries occurring outside the living body. “It will not be invasive on the body at all. High energy will be applied in a concentrated way in the organ,” he explains. The robot takes control and the surgeon is just there to supervise and tell the robot where to work.
7. The race to stop aging
Jeanne Calment was 122 when she died in 1997 and became, as her tombstone states, “the doyenne of humanity.” The Frenchwoman holds the record as the oldest person who ever lived, but the average life expectancy of humans is more modest: 73 years, according to the World Health Organization. Life expectancy has increased by six years since the beginning of the century, but the scientific community is trying to slow down the clock even more. The goal is to help people live longer and with a better quality of life.
In this pursuit, the first great advance was made by Shinya Yamanaka, who in 2006 invented a technique to turn adult cells into stem cells. This showed that cells could be rejuvenated in the laboratory. Since then, research on cell reprogramming has been non-stop. The multinational Altos Laboratories has hired some of the world’s best scientists, including Yamanaka and Juan Carlos Izpisúa, to research how to combat aging. “Our main goal is to enable people to have a healthier life for a longer period of time and to reverse illness in patients of all ages,” Izpisúa told EL PAÍS in an interview last month.
The concept of aging as something that can be reversed opens a wide range of possibilities. “Inflammation is common to aging and there are many studies underway to find out where this comes from, if it is due to the accumulation of genetic mutations or due to food,” explains Salvador Aznar Benitah, the head of a stem cell and cancer laboratory at the Biomedical Research Institute of Barcelona in Spain. “We are always going to get old and die, but we can slow down the process.”
8. New advances in transplant surgeries
Spain has become a global leader in donating and transplanting organs: in 2021, more than 5,000 transplant surgeries were carried out. But needs are growing as is the waiting list. More transplant organs are needed and the scientific community has begun looking for alternatives. On the horizon is the creation of organs and tissues made in laboratories or with 3D bioprinters, as well as strategies to prolong the life of organs that have already been transplanted. Research is also being done on genetically modified animal organs, such as the pig kidney that was implanted in a brain-dead woman in 2021, which worked correctly for 54 hours, or the pig heart that was given to an American man in January, which gave him two more months of life.
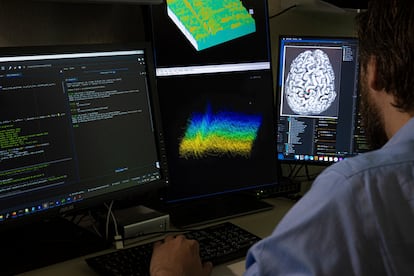
9. Neuroscience revolution
Paralyzed patients who can walk again, chips that allow people to write with their mind… What may seem like science fiction has become a palpable reality when it comes to neurology. Brain-machine interfaces, the name given to communication systems that monitor brain activity and translate it via a computer, have been seen to be effective at overcoming the functional limitations of people with neurological diseases. But the technology is still in its infancy, explains Álvaro Sánchez Ferro, the coordinator of the Committee of New Technology at the Spanish Neurological Society. “It’s an alternative to recover functions when you have lost neurological capabilities. But its long-term safety still has to be demonstrated, and it has to be regulated.”
Scientists are following this line of research, but the technology still has a long way to go, warns Sánchez Ferro. A few days ago the journal Nature Communications published the case of an ALS patient in a completely locked-in state who was able to communicate his thoughts via a brain implant and spell his name. But the interface became less and less effective, and the patient can no longer use it to communicate.
In the area of therapy, biomedical advances will help eliminate proteins, such as those that build up in the brain and cause diseases like Alzheimer’s.








































