Burnout among Spain’s healthcare workers
The sixth coronavirus wave is straining staff at hospitals and medical centers and exacerbating the pressure faced by an already-overwhelmed system
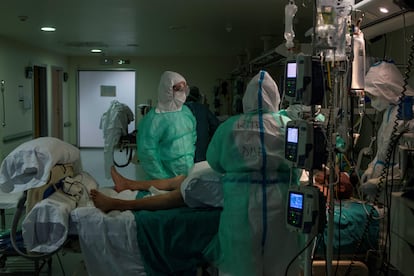
When stress levels exceed one’s capacity for resilience, professional burnout syndrome appears, causing damage not only to physical and mental health, but also affecting one’s ability to respond and adapt to daily circumstances. Before the coronavirus pandemic took hold, the Spanish national health system – in particular primary healthcare – was under considerable stress due to the chronic gap between the available resources and growing demand from patients. In the nearly two years of pandemic, Spain’s healthcare centers have faced successive waves of infections and the overload that these entail, and while they have received reinforcements they have never been sufficient to cover needs. Just when there was light at the end of the tunnel, the sixth wave arrived and multiplied stress levels.
With a 14-day incidence of more than 3,000 cases per 100,000 inhabitants, and more than 300,000 new infections registered in Spain in a single day, healthcare centers are having to attend to a flood of coronavirus patients in addition to those with other illnesses. Adding to the situation is the rise in staff members who are sick themselves due to Covid-19, something that is adding to the pressure on those who remain active. It is no surprise, then, that there has also been a wave of professionals going on leave for depression, taking early retirement or simply quitting their jobs altogether.
Many professionals feel uncomfortable offering minimal levels of care in pressured and chaotic situations, something that is not bringing them any kind of satisfaction and is keeping them constantly on the brink of breakdown. Packed daily schedules, onerous bureaucracy and a lack of manpower are causing physical weariness and emotional exhaustion, all of which are difficult to manage without help. Working under this kind of pressure increases the likelihood of causing medical errors, and there is also the need to manage the dissatisfaction of patients themselves, who have the impression that the care being offered has deteriorated, prompting them to convey this ire to frontline professionals.
A fundamental part of responding to the pandemic consists of taking care of our carers
As such, the ideal conditions exist for the typical symptoms of professional burnout: anxiety, insomnia and depression. Some studies carried out last year suggested that up to 45% of healthcare workers were presenting one of these three symptoms.
A fundamental part of responding to the pandemic consists of taking care of our carers. When the organization itself is showing symptoms of stress, more resounding and effective measures than those adopted until now need to be taken. The healthcare system needs to be strengthened, and not weakened, during this challenge.
Some regions have turned to retired professionals and students in their final year at medical or nursing school to bolster their staffing. If the warning from the regional director of the World Health Organization in Europe, Hans Kluge, comes to pass, and half of Europeans become infected with the omicron strain of the coronavirus in the coming weeks, it is likely that this pressure will continue.
At the same time, there are still no studies on what percentage of patients infected with this variant will develop so-called “long Covid.” But even if the proportion is lower than with previous waves, given the huge spread of the virus the likelihood is that there will be many cases, which will have to be dealt with once more by the primary healthcare system.
It’s very likely that the approved budgets for healthcare will fall short of the needs to attend to all of these eventualities, given the spending of the previous years. The authorities cannot look the other way. The central government and the regions – who are in charge of their healthcare systems – must explain their position on the need for a national emergency plan that is capable of reinforcing the professional structures of public healthcare.








































