The perfect storm of Spain’s sixth coronavirus wave: Omicron is spreading at Christmas, with few restrictions in place, and waning immunity
The new variant of the virus is causing a feeling of chaos among citizens given the high numbers of infections. Experts are warning that the health system could be overwhelmed once more
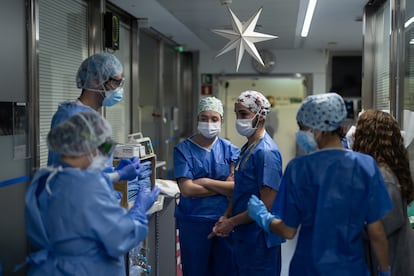
Coronavirus infections are everywhere in Spain right now: not a school, office, group of friends or family is free of a case close to them. “Everyone knows someone who has got Covid in recent days,” explains physicist and expert in computational biology, Clara Prats. The sixth wave of the pandemic is battering Spain and breaking all records. The country’s hospitals, however, are holding up well.
On Thursday, for example, the highest number of infections in a day was reported: nearly 73,000. The 14-day incidence, meanwhile, rose to 911 cases per 100,000 inhabitants. This was also a record for Spain, even compared to the very high levels seen in the third wave.
So what is special about this new wave of the virus? Above all else, there are conditions that amount to a perfect storm: there are few restrictions in place, the immunity offered by Covid-19 vaccines is waning, and a new variant, the more-contagious omicron, is spreading fast.
In just a few weeks, the world has been turned upside down once more, with rampant infections, borders being closed and severe restrictions being introduced in parts of Europe. In Spain, primary healthcare centers are on the brink of being overwhelmed, there is a lack of supply of home antigen tests in the country’s pharmacies, and hospitals – while far from being congested – are holding their breath as they see admissions rise. The coming days will be crucial to calibrate the severity of this wave, the experts warn.
According to Prats, the sixth surge is, in reality, “two waves in one.” “There was a beginning with the delta variant, which became more complicated with omicron,” she explains, in reference to the two strains of the coronavirus that are widely circulating. “In the autumn, the curve was rising bit by bit, as if it was in slow motion and with a margin to react. But then suddenly, omicron arrives and changes everything from one day to the next. First it arrived in Madrid, then in Catalonia and it started to spread. Once you reach 40% of omicron, the infections spike.”
According to the latest report from the central Health Ministry, based on preliminary data from December 6 to 12, 47% of samples analyzed were omicron. The new strain is muscling in on what was dominant until now: delta. In fact, some regions are already reporting higher figures, such as Madrid, where the strain accounts for 80% of cases.
On the ground, healthcare centers are struggling to deal with the lines of sick people waiting outside, and staff are close to burnout. Patients are desperately seeking antigen tests to confirm whether they have an infection, or are impatiently awaiting a call from contract tracers. Or they are simply staying at home to see what happens.
There is a sense of “generalized chaos” in the streets, in the words of epidemiologist Mario Fontán. “There is mayhem because people need their symptoms to be confirmed so that they can be given medical leave,” he explained several days ago. “A sensation of greater chaos has been created compared to the severity that the clinical picture requires.” But this snowball that is growing right now dates from weeks back.
Vaccines are still working very well against serious illness, but the protection against infection falls from six months onwardTomàs Pumarola, the head of microbiology at the Vall d’Hebron Hospital in Barcelona
One of the first elements to spur the resurgence of the virus was the relaxation of restrictions. When the epidemiological curve began to rise, at the start of November, there were barely any restrictions in place apart from masks indoors. Now, six weeks later and with the incidence 18 times higher than then, the so-called “Covid passport” is being used for access to certain spaces, while the government has reintroduced obligatory masks while outdoors – a measure that is of dubious effectiveness according to the experts. Only seven of 17 regions are opting for more severe measures, such as limits on opening hours and capacity, and in the case of Catalonia, also a curfew and limits on social meetings.
What’s more, the protection offered by the Covid-19 vaccines wanes with time. A study from the Health Ministry, for example, shows that their effectiveness against infection and symptomatic infection in the 50-59 group falls progressively: it’s above 90% in those vaccinated in September and falls to 69% in those vaccinated in April. For the 40-49 group, the effectiveness is 80% in those vaccinated in September, but this falls to 35% for those vaccinated in June.
Tomàs Pumarola, the head of microbiology at the Vall d’Hebron Hospital in Barcelona, insists that the vaccines “are still working very well against serious illness, but the protection against infection falls from six months onward.”
This is why the Spanish government is speeding up the administration of booster doses, prioritizing vulnerable collectives such as those with suppressed immune systems and seniors – 86% of the over-70s have already received their third shot, while for the over-40s the figure is 45%.
Third dose
Prime Minister Pedro Sánchez last week announced that anyone vaccinated with the Pfizer-BioNTech or Moderna vaccines would get a third dose six months after their second. The central government wants to see 80% of the over-60s vaccinated before the end of the year, and all of the over-40s by the start of March.
This fall in vaccine protection, combined with the current season of high social interaction and movement due to the national holidays on December 6 and 8 and the Christmas break, have ended up fanning the flames of a blaze that began with delta and has spread thanks to omicron.
Daniel Prieto-Alhambra, a pharmaco-epidemiology researcher at Oxford University, points to several characteristics of this wave. “If you think about the sixth wave with delta, the key to the progress depended on vaccination and the restrictions of different countries,” he explains. “Here in the United Kingdom, for example, masks were not used in the summer even indoors, while in Spain they were.” This difference, along with a higher vaccine coverage rate in Spain, saw incidences 20 times higher in the UK over the autumn. “However, if we focus on the sixth wave with omicron, the key is that it has a greater capacity to infect people who have been vaccinated than delta did, but like the majority of infections among vaccinated people, the percentage of hospital admissions is much lower than during previous waves.”
Omicron has homogenized the situation across Europe – and in a bad way. José Martínez Olmos, a professor from the Andalusian Public Health School, explains that “before omicron, what made [Spain] different from other countries was the better vaccination coverage and greater tendency to be outside due to the climate, but now, with this variant, infections are the same. There are no borders,” he says.
A less-severe wave?
The only positive outlook is to be found in preliminary studies from South Africa, Scotland and England, which point to this wave being less severe. In fact, in South Africa, where the new strain was first identified, the curve appears to be flattening after four weeks of rises and is actually starting to fall, according to the Our World in Data website.
But the impact of this wave could still be “devastating,” experts explain. A flood of new infections will mean – in absolute terms, albeit not in percentage terms – more hospital admissions and stress on the health system. “A small percentage of a very big number is still a big number in terms of the impact on the population,” warns Prieto-Alhambra. “If nothing is done, even if omicron is half as severe as delta, we will be in a catastrophic scenario. It would double the peak of previous waves.”
In Spain, at the beginning of February 2021, in the midst of the third wave, there were more than 30,000 Covid-19 patients in hospitals. In the intensive care units (ICUs) there were more than 4,800. Right now, there are much fewer: 7,924 patients, 1,515 of whom are in the ICU, according to the latest Health Ministry report. Hospitals are not yet suffering at the levels of other waves. But the outlook is not good, according to Toni Trilla, the head of epidemiology at the Clínic Hospital. “There was sustained stress on the health system over time and overwhelming work that was difficult to manage in the primary healthcare system.”
Experts are also criticizing the scant communication from the authorities during this sixth wave. Elena Vanessa Martínez, the president of the Spanish Epidemiology Society, complains that “we haven’t learned anything. We needed to strengthen the primary healthcare system and the public health infrastructure, because they were essential as the first shield against the virus, and this has not been done. The population has the impression that restrictions aren’t necessary, and that testing is enough. And people are looking for tests because they consider them their salvation, because there are no other measures.”
Bad communication
Magda Campins, the head of epidemiology at Vall d’Hebron Hospital in Barcelona, agrees. “The communication from politicians and from Public Health is very bad,” she says. “Until recently they were saying that there would be no restrictions, and when you give out that message, people rely on it.”
There are still many unknowns about how this new wave will progress, and above all its severity. The coming days will be key, the experts insist, as will the restrictions that are taken to contain infections. Relying just on vaccination, they warn will be impossible, although they add that the administration of third doses must be speeded.
Since the summer, Prieto-Alhambra explains, “Spain fell into complacency and the third doses are going slower than in the United Kingdom, which has already given 54% of its over-12 population a booster shot.” Speeding up these injections was another of the strategic approaches announced last week by Prime Minister Sánchez in a bid to slow this sixth wave.
All in all, the race against Covid-19 is far from over. “This virus is capable of changing greatly, whether that’s slowly or in major leaps,” explains Pumarola. “With the measures that we are putting in, we ourselves are forcing it to constantly change. The H3N2 flu virus caused a pandemic in 1965 and even now it causes tension when it returns. Well, that is what is going to happen with Covid.”








































