Turkey: The dangers of low-cost surgery
In the last decade, the country has become a destination for cheap implants and medical procedures. Such operations have hidden costs
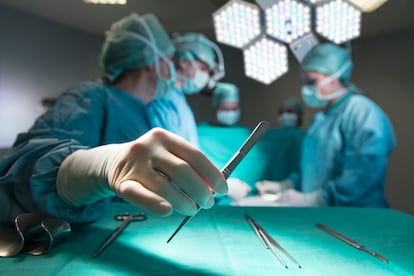
Sixty-seven people in Europe have become infected with botulism after undergoing weight-loss surgery with botulinum neurotoxin in Turkey. The news has called into question the safety of such interventions. The last ten years have seen Turkey become a destination for low-cost implants and surgeries, but they do not always end up as cheap as planned.
The botulism cases are iatrogenic, meaning that they result from a medical intervention. The origin is unknown, however: it is not clear whether they were produced by bad practices or by the toxin itself.
The use of botulinum neurotoxin for weight loss has not been explored beyond clinical studies. It is being used without scientific evidence, which can bring unknown risks. The use of the toxin, through intragastric injection, relaxes the muscle walls of the stomach. In theory, the process slows down the stomach’s emptying, and the person feels more full, allowing them to consume less food and lose weight. No studies have demonstrated the procedure’s functioning, however. If it does work, the intervention should be repeated every five or six months, as the toxin’s effects decrease.
I have received patients who have undergone bariatric surgery in Turkey. They do not know what technique was used, and they did not receive a report or post-operative instructions. Two days after the surgery, they traveled home on an airplane. I do not doubt that there are clinics who follow correct protocol, but my experience is the following: patients do not know what to do after the intervention and lack post-operative check-ups, nutritional guidelines and medical control.
Bariatric surgery is recommended when dietary changes have not worked for patients with a body mass index (BMI) of 35 or above, independently of comorbidities. It is also considered for patients with a BMI between 30 and 34.9 who have a metabolic illness.
The patient’s psychological state should also be evaluated to determine if they suffer from eating disorders or consume toxic substances. A multidisciplinary team, composed by surgeons, nutritionists and psychologists or psychiatrists, should evaluate the candidate and follow up after surgery.
Although bariatric surgery is necessary and successful for most who receive it, many do not receive enough information before deciding to undergo the operation.
No matter the quality of the surgery, the patient will have to change their diet, physical activity and lifestyle for the rest of their life. They also should take into account the risks that any surgery involves.
The dietary changes, in most cases, begin before the operation. A liquid diet is recommended for at least two weeks before the operation to minimize risks, as well as after the operation. Solid foods are to be gradually reintroduced. As the digestive system is affected, the patient may experience vomiting, diarrhea, difficulty swallowing and dumping syndrome (rapid gastric emptying, from 10 minutes to 2-3 hours after eating).
It is necessary to monitor nutritional intake to avoid nutrient deficits. The patient should follow a diet plan specific to their needs, lifestyle and social and economic context.
The ease of changing one’s physique via an operation can be appealing. For that reason, psychological follow-up is recommended. The body changes quickly, but the head needs to assimilate the changes with professional help. Generally, the body retains excess skin. As with any intervention, post-operation checkups are necessary.
Bariatric surgery is a much more complex process than rumored. Health is not just a question of kilos.
Sign up for our weekly newsletter to get more English-language news coverage from EL PAÍS USA Edition








































