What is harlequin-type ichthyosis, the strange ‘fish skin’ disease?
This very rare dermatological condition is caused by a genetic mutation that alters the process that forms the epidermis. One patient spoke out to ‘stop the stigmatization’

Ariadna López’s skin has been eroded since the day she was born. Dry and cracked, sometimes red, from head to toe. This 21-year-old woman suffers from harlequin-type ichthyosis, a highly unusual dermatological condition that is caused by a genetic mutation that alters the process through which the epidermis is formed. It is, as the etymology of the name suggests, a kind of fish skin, always scaly.
Every day, Ariadna has to go through an essential hygiene ritual. Hydration with creams every few hours; showers two or three times, if necessary; soaking in a coal tar preparation several times a week; and exfoliating her body with a special glove that removes dead skin. Care cannot be skipped nor delayed. This is necessary so that the disease is not aggravated by infections or other more serious alterations.
Harlequin ichthyosis is a very rare ailment. Many of the babies that are born with this disease die soon due to the associated complications, as they struggle to breathe and eat, and even get infections from the wounds caused by the skin alteration. Affected newborns enter the world with a kind of armor made up of thick plates of scales that are divided by deep fissures; those fissures facilitate infections through the skin, and this armor can make it difficult to hydrate and regulate the body temperature.

A review of 45 cases published in 2011 revealed that 25 affected individuals (between 10 months and 25 years of age) survived, while another 20, all under three months of age, died of respiratory failure or sepsis, which is a uncontrolled response of the immune system to an infection.
The disease is so rare that there are no clear prevalence data, only estimates and approximations: less than one case per million individuals, according to the Orphanet database. The authors of a 2014 study mentioned that, at that time, there were approximately 200 cases reported in the world.
The scientific community has described more than 30 types of ichthyosis, all with different levels of incidence and severity: some affect only the skin (non-syndromic, such as harlequin-type ichthyosis) while, in others, the genetic defect manifests itself in other organs besides the skin (syndromic). The harlequin type is part of a non-syndromic subgroup, autosomal recessive congenital ichthyosis. They are passed on from parents to children when both parents are carriers of the genetic mutation. In the case of harlequin ichthyosis, there is a 25% chance in each pregnancy that the child will have the disease.
The cause of this condition is a variation of the ABCA12 gene, which alters keratinization, the process by which the epidermis is formed. The ABCA12 gene intervenes in a lipid transporter in the cells that make up the epidermis; since it doesn’t work properly, patients have a completely altered epidermis that does not serve as a defense against the external environment. This genetic alteration prevents the formation of the skin barrier that regulates temperature and protects against infections and dehydration.
Alopecia and joint problems

Dealing with harlequin-type ichthyosis is not easy. This flaking of the skin leads to other bodily alterations that complicate the prognosis from birth. Patients suffer from ectropion, which means that their eyelids do not close properly. They also tend to have their ears stuck, lose flexibility in their fingers and suffer from complete alopecia. In addition to the deterioration in their appearance, they also have eye and joint problems and do not sweat well.
Ariadna has been through, and is still going through, all of that. She sees dermatologists, otolaryngologists, rheumatologists, and ophthalmologists. “My eyelid is not well-formed and it doesn’t close completely, so I have to moisturize my eye because it dries out a lot. I have to wipe my eyelid so that the scaly skin doesn’t get inside, and put some ointment on the edge of my eye before going to sleep. I also suffer from burning and itching of the skin, and I have problems with my joints because, since my skin wasn’t very elastic, my bones could not grow well, so I have arthritis. In the winter, my skin dries out more and it becomes more difficult for me to walk or pick up something,” she says.
The peeling can affect the cornea as well as the ear, plugging it with dry skin. Patients also suffer from hyperkeratosis, a thickening of the skin that can encapsulate or compress the extremities and affect the motor skills. Since they do not sweat properly, they also cannot tolerate hot environments well. Fever, for example, is agony for Ariadna. “I can’t sweat to expel the heat, and the fever usually lasts a long time. My skin becomes super rigid and I can barely move,” she says.
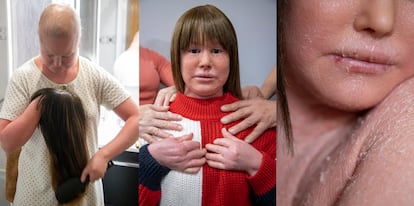
Ariadna, who suffers from alopecia, has been wearing a wig since she was 11 years old. However, she is beginning to leave the house with a headscarf, “overcoming insecurities little by little,” she says. “I am in the process of acceptance, and if one day my skin is very bad, it doesn’t affect me as much. I just think that it will pass.”
José María Soria, president of the Spanish Association of Ichthyosis, explains that a diagnosis of this disease is a hard blow for both the patient and their family. “The ones who first suffer from the disease are the parents, who find themselves before an unfamiliar illness and don’t know if the child will survive.” This is joined later by the psychological weight of the looks of others. But Soria is categorical: “You don’t have to hide anything. You have to show it in order to normalize it.”

Beyond the physical and psychological burden that the patients and their families carry, those affected by the disease also face an economic burden, as any ichthyosis requires a series of topical skin products.
For this reason, Ariadna wants to draw attention to her illness, so that everyone is aware of all the money and time that those affected by it spend by applying treatments that are only palliative, as they suffer from a lot of itching and stinging, among many other things. She also wants to stop the stigmatization. She emphasizes: “Now that I’m older, I deal with it much better. Still, it hasn’t been easy, having to put up with looks of disgust or pity every day, inappropriate comments, expressions of contempt... And all this is due to ignorance and lack of knowledge. We want people to put themselves in our shoes to fight for ichthyosis research, so that one day we can talk about it in the past tense.”

As is the case with all rare conditions, the search for a cure or any therapeutic alternatives to overcome the risks of the disease can be quite a struggle. Starting a study is not easy, although Dr. Ángela Hernández, a member of the Spanish Academy of Dermatology and Venereology, admits that the pace has increased in recent years, and that tests have begun on biological drugs to improve the situation of patients. “In keratinization disorders, we know that patients have systemic inflammation. What we want to do is reduce the external inflammation and improve the condition of the skin. What would be ideal would be to find a biomarker that allows us to carry out a targeted treatment with a biological drug. But, of course, for this type of research we need money, and the resources allocated to rare diseases are, unfortunately, very limited,” she points out.
With so few patients, there’s not much interest from the pharmaceutical industry. “They’re not profitable,” laments the dermatologist.
