Coronavirus infection leads to a loss of gray matter in the brain, study finds
Neurological images show the areas of the brain that display the greatest changes are related to smell, according to research from the University of Oxford


Two scans, one performed before the coronavirus pandemic and another in the worst months of the global Covid-19 crisis, show that people who have contracted the virus experience changes in the brain that do not occur in those who have not been infected. A recent study shows the decrease in gray matter is generalized and the most-affected areas are related to the sense of smell. The authors of the paper do not know whether this damage is caused by the virus itself or as a result of the illness it provokes. They also do not know if the effects are temporary or permanent.
Several studies have linked coronavirus infection to neurological problems. Among the most common symptoms, even more so than respiratory issues, are anosmia and hyposmia, a total or partial loss of smell, respectively. Most people who suffer from long Covid also report a certain slowness of mental capacity (also known as brain fog) or an inability to concentrate. But beyond post mortem tissue analysis of fatal cases, there have been few studies that have focused on what was happening in the brain.
Now, a group of researchers at the University of Oxford has been able to study brain images taken from nearly 800 people in the United Kingdom. The study is longitudinal, which is to say it collates data from the same group of people at different times. This provides additional robustness in terms of results. Half of the study group had contracted coronavirus between one MRI scan and the second, taken more than three years apart, which allowed the researchers to compare changes in the brain caused by the virus and compare them with brain images of unaffected subjects.
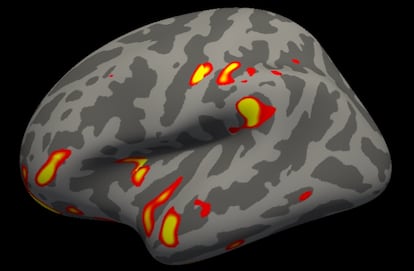
The results, published in the science journal Nature, show that people who have been infected by SARS-CoV-2 had a greater loss of gray matter and more pronounced alternations in cerebral tissue. The differences were bigger in the parts of the brain that control the sense of smell, such as the orbitofrontal cortex or the parahippocampal gyrus. All of the changes noted were more pronounced in older people.
Professor Gwenaëlle Douaud of the Nuffield Department of Clinical Neurosciences at the University of Oxford and lead author of the paper, states that the research also showed “changes in regions unrelated to the sense of smell, such as the temporal pole, the supramarginal gyrus or the cerebellum.” In terms of total brain volume, “there was an additional loss of around 0.3% among infected participants,” she adds. That is the average, but there were cases that showed a reduction of 2% in brain volume, a percentage that is higher still in the olfactory regions. Again, the deterioration was comparatively greater the older the subject was.
In parallel with the second MRI, the test subjects were asked to perform a series of cognitive tests of the type that people with neurodegenerative diseases or who have suffered a brain trauma regularly do. Although in general, the subject who had contracted coronavirus passed almost all of them, “they displayed a greater decline in their mental abilities in completing complex tasks,” says Douaud. Specifically, their scores were lower than volunteers in the control group when it came to the speed with which they were able to complete the tasks.
Tomás Segura, head of the Neurology Department at Albacete University Hospital, has since January been conducting a similar study among a group of 100 Spaniards who have contracted Covid-19. He has yet to analyze the images he has taken of their brains, but the group has been put through a series of neuropsychological tests. Segura has seen, as in the Oxford study, that “they perform them more slowly and have a diminished ability to inhibit attention.”
One of the strengths of the Oxford investigation is that an average of 38 months had passed between the first and second scans. Another is that the second brain image was taken more than four and half months after coronavirus infection, which indicates a certain permanence of the effects. Furthermore, the vast majority of the participants, other than 15 who were hospitalized, experienced mild coronavirus symptoms.
In the view of David García Azorín, spokesman for the Spanish Neurology Society, “this presents a unique opportunity to see if the changes in the brain are due to the infection and not to the aging of the brain itself.” However, only taking more scans within a period of time will allow researchers to determine whether the changes remain, or as García Azorín puts it: “If the two groups retain a similar brain or if those affected by Covid-19 show further deterioration.”
This presents a unique opportunity to see if the changes in the brain are due to coronavirus infection and not to the aging of the brain itselfDavid García Azorín, spokesman for the Spanish Neurology Society
What the authors of the paper and the Spanish experts consulted are not clear on is what is causing what. There are at least three possibilities that could explain the brain changes among people infected by SARS-CoV-2. One is the direct action of the virus on the central nervous system. Another could be that it is all related to the inflammation that accompanies the immune response. And there is a third theory, backed by some investigations: that the virus spreads through the olfactory mucosa, in the inner part of the nose, killing off olfactory neurons and the cells that support them and, as such, leading to loss of smell. This would cause atrophy, through lack of use, of the cerebral circuit that processes smells. Science has known for some time that the loss of one sense or another leads to changes in the associated part of the brain. Unlocking this enigma will help to determine whether the changes observed are temporary or permanent.
This is also one of the weak points of the study: the researchers did not determine if the people in which changes in the brain were observed had reported loss of smell or not, or other disorders of neurological origin, such as brain fog or headaches. Another weak point is the demographic. Although the two groups, infected and uninfected, were balanced in terms of age, gender, risk factors and race, the study was limited to people aged over 50.
Segura poses one final question: the enormous scope of the coronavirus pandemic has allowed the brains of hundreds of people to be studied at the same time but, the neurologist asks: “What is happening with other viruses such as Epstein-Barr or viral encephalitis; what impact on the brain do all the pathogens that attack us throughout our lives have?”







































