AIDS: from fear to unawareness
Incidence of HIV in Spain remains above EU average despite widely available information

“How can this be happening to me?” asks Sergio over and over again. “I know about the issue, I’m a responsible guy and and I didn’t do crazy things.”
Sergio, 22, felt immune. But his ex-boyfriend was unfaithful, and they both ended up contracting HIV. He started on antiretroviral medication a week ago.
“I didn’t expect it to happen to me,” he repeats. “People these days are not as concerned about it as they used to be. They treat the disease as though it could never happen to them. And when it does, they wring their hands in despair.”
People treat the disease as though it could never happen to them. And when it does, they wring their hands in despair”
Ramón Coello was told he had the retrovirus in 1987, shortly after his girlfriend tested positive for HIV. He hadn’t been expecting it, either.
“I was scared; I thought I would be dead in the space of two years,” says Coello, now 58.
More than three decades have elapsed since both men contracted HIV, but cases in Spain (3,278 people in 2013, according to the Health Ministry) remain above the EU average.
“People were dying all around you and it seemed like it was unstoppable,” recalls Coello. “These days very few people die of the virus, and there is lots of available information, but a lot of people are just ignoring it.”
Sergio did not become fully aware that he was an HIV sufferer until he went to pick up the medication that he will need to take for the rest of his life.
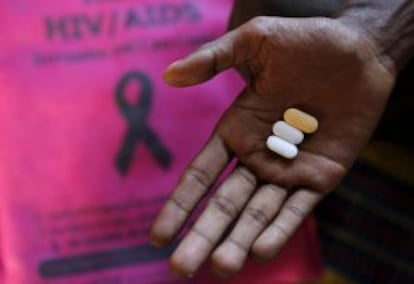
“Every month you have to go collect a bunch of pills,” he explains. “That first time, I realized that it was all true.”
Sergio takes two pills a day, while Coello takes one: Atripla, a combination of three antiretroviral drugs. But his early treatment was a cocktail of 15 different products.
The first official HIV transmission was diagnosed in San Francisco in 1980. A year later, the virus appeared in Barcelona.
“We were told our life expectancy was anywhere between two and 10 years,” says Coello. Back then, HIV was a fierce and dangerous new virus. Shortly after Coello learned about his condition, the first effective antiretroviral drug, AZT, was made available in Spain. But his partner did not live long enough to benefit from it. “When she died, I thought I would soon be next.”
Coello has personally experienced nearly every medical advance made on the subject of HIV. “I never imagined I would be able to keep the disease in check,” he admits.
The first cocktails he took caused significant physical side effects. “Nausea, stomach trouble, pain... Medicine has made an infected person’s life easier. Right now it is a chronic disease that can be kept under control, but people shouldn’t kid themselves: this is not like popping a pill for your blood pressure,” he warns.
Although side effects today are not as overwhelming as they used to be, they can affect the liver, create sleep disorder, produce skin rashes and more.
“At first you’re a mess,” says Sergio about his own limited experience. “You’re tired, you don’t feel like doing anything, you’re kind of exhausted. Later, everything seems to get better.”
Sex education is left up to families, and it is often not properly explained, either out of embarrassment or ignorance” Reyes Velayos, Apoyo Positivo
Mario has just turned 18. He figures he has had sex with around 300 men, and has sexual encounters three times a week on average. He also admits that he often fails to use a condom. A little over a year ago, Mario decided to take the test. It came back positive.
“A lot of people do it without protection in the heat of the moment,” Sergio explains.
Sergio and Mario are both part of the social group that recorded the greatest rise in HIV infections in 2013: young homosexual men. The incidence of the disease in this community has grown 10 points in the last five years. And one out of every four new cases in 2013 were gay men under 30.
By comparison, high-risk heterosexual relations represented 28.5 percent of new cases. Fifteen percent of positive diagnoses affected women.
“When you’re young you don’t consider the possibility of contracting it yourself,” says María. “You feel it’s something that happens to other people with specific traits [prostitutes, very promiscuous people or drug addicts]. And if you feel it can’t happen to you, why take protection measures?”
María got infected at age 27. She was seeing someone, and they decided to stop using condoms. “Are you healthy?” she asked him. “Yes,” he replied. Either he didn’t know he had HIV, or he did not tell her.
Nearly half of all new cases in 2013 had late diagnoses, meaning that they had been infected for some time but had never been tested before. The Health Ministry estimates that between 130,000 and 160,000 people may have HIV in Spain, and that around a fifth of them don’t know it yet.
I’ve felt a lot of support from the community, but I think the world in general does not fully accept you”
“I have a partner and a son. Both they and most of the people around me know about it,” says Coello. “In general I’ve gotten normal reactions, although occasionally I have regretted telling some people.”
Sergio has only told his own family, and friends who are HIV-positive like himself. “I’ve felt a lot of support from the community, but I think the world in general does not fully accept you,” he says.
Sex is the main mode of transmission, and both patients and advocacy groups stress the need for emotional and sex education.
“There is no sex education on the school curriculum, and as a result young people know very little about sex and the virus,” says Reyes Velayos, president of Apoyo Positivo, a support group that is part of the larger CESIDA group. “This type of education is left up to families, and it is often not properly explained, either out of embarrassment or ignorance.”
Just like Sergio, most people feel that it cannot happen to them. Coello sums it up in one sentence: “That emotional distance reflects that Spanish society, in general terms, still doesn’t know how to deal with HIV. It’s been quite some time since the beginning of the pandemic; it’s about time they learned.”








































