Alima has bronchiolitis, but there is not enough oxygen to save her at this Ethiopian hospital
A Spanish pediatrician in a rural health center south of the capital city is struggling to save the lives of children with respiratory diseases
Alima inhales deeply, as if each breath were her last. Perhaps it is. Every muscle in her body strains to take in as much air as possible. Each inhalation is a battle won, another breath of oxygen to prepare for the next one. But the war continues. Her lung infection – bronchiolitis – squeezes her inflamed airways, threatening death by asphyxiation. Alima’s ribs are outlined on her small chest as she tries to expand her lungs as much as possible. Just a few months old, Alima arrived exhausted at Gambo Hospital in rural Ethiopia. The major air passages (bronchi) of her lungs are obstructed and she is worn out from the effort of breathing. She stretches her neck toward the sky as she tries to inhale.
Alima had to travel far to get to Gambo Hospital, and she’s not the only one. Small bodies crowd the cramped waiting room to its maximum capacity. Just when it seems like there’s no more room, four more children arrive. Like everyone else, they need oxygen. But in rural hospitals like this one, it’s a scarce commodity.
When I was a pediatric resident at Granollers General Hospital in Barcelona, I remember being able to turn a little dial on the wall and oxygen would magically flow from a duct that ran throughout the building. I thought that was normal and didn’t appreciate it enough. But after my experience in this hospital south of Addis Ababa, Ethiopia’s capital city, the Granollers oxygen supply seems miraculous.
Gambo and most other Ethiopian hospitals use heavy oxygen cylinders that often must be transported long distances to be refilled. I thought that I would be treating children with tuberculosis, AIDS, malaria and other tropical diseases. But instead I found that most of these young patients have bronchiolitis, bronchitis and other respiratory infections. I quickly learned to appreciate medical oxygen, which doesn’t come out of the walls.

We’re in the middle of a bronchiolitis epidemic and don’t have enough resources, especially oxygen. Gambo Hospital has over 15 children in need of oxygen, but only two concentrator devices and insufficient cylinders that are quickly depleted.
One of our most valuable pieces of equipment is the “Y,” a simple plastic or metal tube that splits the oxygen supply so it can be administered to two patients at once. We can attach two more “Y” tubes and supply four patients with oxygen. I wish it would multiply the oxygen itself. While this little device enables us to supply more children, we pay the price in the reduced flow that each one receives.
It’s time now to assess all our patients and prioritize the most serious cases. We’re in a drastic situation – we need more concentrators so we can produce more oxygen and don’t have to ration it as much. As soon as a patient starts to improve, we have to take them off the oxygen to give it to others who have deteriorated. Alima and others like her are the silent victims of the injustice of being born in rural Ethiopia.
When the power goes out, we have to use a generator that runs on very expensive fuel to operate the equipment. The alternative is taking the cylinders to be refilled in Addis Ababa, over 100 miles (260 km) away, another very expensive proposition. Meanwhile, girls like Alima struggle to breathe. As Chilean poet Gabriela Mistral wrote, “To him we cannot answer ‘Tomorrow,’ his name is Today.”
No one is ever sure how many beds we have in the pediatric ward. One day there are 45, the next day 57. Officially, there are 45 beds, but those of us who work here know that this isn’t true – we’ll add as many beds as needed. We can only do this because of all the dedicated workers: cooks, cleaners, nurses, assistants, nutritionists, midwives, maintenance technicians, doctors... a team of more than 150 Ethiopian employees.
It’s also a hospital with 300 hands, offering employment and training to the people of this rural area. Their effort, sacrifice and dedication has a real impact on the health, education and living conditions of these people. The hospital workers are the real heroes – without them, the hospital would not exist. I want to acknowledge each one, because they show up day after day to stand in front of this cannon, this epidemic. We have already faced outbreaks of measles, meningitis and bronchiolitis. What’s next?
I wouldn’t want you to live like we do, surviving on the edge as we measure and divide liters of oxygen and doses of medication. I have learned to jump for joy when the power comes back on, providing electricity for oxygen concentrators, incubators, operating room and laboratory machines, and conserving expensive generator fuel. When the power goes out, the problem is not finding a candle to light. It’s not being able to turn on an incubator or an oxygen concentrator. It’s watching helplessly as lives slip away.
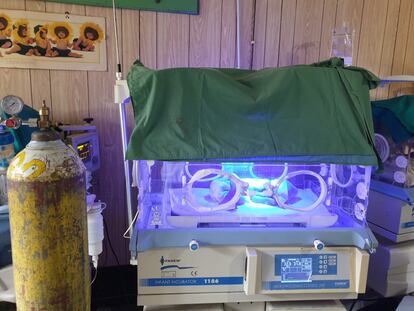
Life goes on and we will keep on filling oxygen cylinders, adding “Y” tubes and dreaming of an endless oxygen supply that comes out of a wall with a simple twist of a dial, like tap water. Speaking of water… well, that’s another story.







































