Vaccination drive saves Spain’s care homes: from 771 Covid-19 deaths a week to just two
Senior residences have seen a 99.7% drop in fatalities and a 98% fall in infections since the end of January. A total 12 of the country’s 17 regions have not reported a single infection


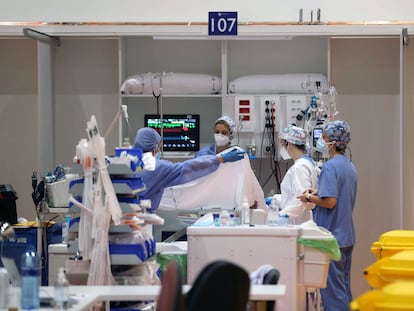
Spain’s vaccination campaign has freed care homes from the stranglehold of Covid-19. With more than 90% of people living in the country’s residences now immunized, residents of one of the black holes of the pandemic can finally breathe easier. According to the latest report from the Imserso institute for seniors and social services, which is part of the Social Rights Ministry, between March 29 and April 4 of this year, there have only been 45 coronavirus infections detected and two deaths. That is a fall of 99.7% in terms of deaths compared to the last week in January, when the third wave of the health crisis was at its peak and the vaccination campaign had not yet taken effect.
A quarter of the deaths registered in Spain since the start of the pandemic took place in the country’s care homes. Since the vaccination campaign got underway, the end of the third wave and the effect of the mass inoculations have also seen infections in residences fall by 98% compared to the end of the first month of the year. In fact, the homes are practically free of Covid-19 now: in 12 of Spain’s 17 regions, there have been no infections reported in the last week.
The virus found a breeding ground in care homes where it could intensify its transmission and it swept through residencesDaniel López-Acuña, former director of emergencies at the World Health Organization
Senior centers were the perfect place for a virus that is transmitted in closed spaces and that preys on the elderly. The healthcare crisis caught these homes unprepared and the coronavirus took hold without any resistance. Over the last year, at least 19,012 elderly people in homes have died from Covid-19 – although the real figure is likely to be much higher, given that testing was limited during the first wave and many people died without having been diagnosed. In fact, the Imserso report includes 10,492 seniors who died in residences with symptoms that correspond to Covid-19, even though infection could not be confirmed.
“The first wave was terrible,” says Daniel López-Acuña, a former director of emergencies at the World Health Organization (WHO). “The virus found a breeding ground where it could intensify its transmission and it swept through residences.”
These centers shielded as best they could during 2020, but they didn’t manage to escape from the virus. Only the vaccine program, which got off to a slow start on December 27 and prioritized residents and staff in care homes, managed to change the course. For this group, the Pfizer-BioNTech vaccine was used. A month after the first shot was administered – the second is given 21 days later – they were protected from Covid-19.
The Imserso report reflects the effects that the campaign has had. During the month of January, when the speed of the campaign was ramped up in senior homes, infections and deaths were still on the rise. Nearly 11% of centers registered cases in the third week of January, falling to 8% in the fourth week. Between January 18 and 24, there were 718 Covid-19 deaths. The following week the number of fatalities peaked for 2021, with 771. But from February onward, the figures began to fall dramatically.

“For this curve, you have to take into account how the progress of the third wave and the vaccinations have had an influence,” explains Salvador Peiró, an epidemiologist at the Foundation for the Advancement of Health and Biomedical Research in the Valencia region. “Seniors were vaccinated in January and they needed two weeks to have some level of protection. By the fourth week, the protection is complete, but from the second week it is already at 80%.”
Last week just Andalusia and Catalonia reported deaths in senior homes, one in each region. That said, the Imserso report clarifies that the data from Andalusia is “notified cases,” meaning that the death could have occurred in previous weeks but not been reported until now. Whatever the case, the downward trend is clear to see in the data, with the occasional spike. From March 22 to 28, there were 24 care home residents who died from Covid-19; from March 15 to 21, there were 17; from March 8 to 14, there were 22; From March 1 to 7, there were 33.
The same thing has happened with infections. Since mid-March, there have been around 45 infections a week, far from the 4,000 a week that were being detected in January. “We’re happy to confirm the hopes that we had placed in the vaccines,” says Jesús Cubero, from the Aeste association in the care home sector. “We knew that they were going to cut infections and that’s what’s happened. We are much calmer now, but we can’t lose our heads. We are gradually restarting activities in the centers and visits, but with prudence.”
Experts consulted by EL PAÍS are also celebrating the good epidemiological data in residences, but voice a call for caution. The pandemic is not yet over and there is no such thing as zero risk, neither inside or outside residences. “Care must be taken when reopening the centers,” warns López-Acuña. “Not enough of the population has been vaccinated outside of the bubbles that are these residences. When we have more people immunized in the general population, we will be on firmer ground.”
Just half of the 80-and-overs in Spain, for example, have had their two doses, a figure that falls to 3% among the 70-79-year-olds and 5% in the 60 to 69 group
Peiró agrees, adding that he fears that vaccinated residents could still infect other people – the vaccine does not avoid infection, but rather the serious forms of the disease. Outside of residences, the percentage of the population that has had their shots is still minimal among the most vulnerable groups, and the risk of infection remains high. Just half of the 80-and-overs in Spain, for example, have had their two doses, a figure that falls to 3% among the 70-79-year-olds and 5% in the 60 to 69 group.
“The danger and the potential for infection still exist,” explains López-Acuña. “There are unvaccinated people in the centers too and they must be protected.” According to the latest report from the Health Ministry, 90.8% of people in institutions – which includes all social centers, the majority of which are senior homes – have had their two shots of the vaccine. But there are residents who have refused the medication, have risk factors, or have been sick and have not been able to have it.
What’s more, the ministry report does not include the percentage of staff in these centers who have been vaccinated. “At the start of the campaign there were refusals from many workers,” explains López-Acuña. “I’m worried that we have people who have not been immunized interacting with these bubbles of residents.”
After a year with the virus inside care homes, staff are now trying to take stock of the damage and set out targets for the future. Experts agree that coordination between the healthcare authorities and social services must be improved, but also that the entire model of care homes needs to be rethought. “This current model, with so many people congregated, represents a risk for future infectious diseases that have an epidemic character,” says López-Acuña. “If that happens, we will be just as susceptible as we were to the coronavirus.”
For the families of residents, the vaccination campaign has brought relief after a year to forget. But they fear that the virus could return to these centers. “We are calmer, but we’re worried about the staff who haven’t been vaccinated and that they end up doing fewer mass tests to detect asymptomatic carriers,” explains María José Carcelén, from the 5+1 care home coordinator. “Our seniors are calmer, but that’s because they can see us more,” she continues. “My mother is 94 and assumes the risk because she is nearing the end of her life. She just wants to spend the time she has left with me. But each infection means isolation. Do we want to give them an end to their lives that involves so much loneliness?”
English version by Simon Hunter.