Spain set to receive 100 million doses of three new Covid vaccines
In the next few months, inoculations from Janssen, Novavax and CureVax are likely to be approved by the European Union, strengthening the offensive against the coronavirus
/cloudfront-eu-central-1.images.arcpublishing.com/prisa/GLL6L67FMFHTDE6GAJOLHPT7HU.jpg)
In the next few months, at least three new Covid-19 vaccines are set to be approved by the European Union (EU). Two of them are being trialed and made in Spain. Each one uses a different technology, with one candidate only requiring a single dose – instead of two – to vaccinate a patient. Together the three vaccines will provide Spain with up to 100 million extra doses. This is the great offensive against the coronavirus.
Janssen
A new vaccine produced by the Belgian company Janssen, which is a subsidiary of the US multinational Johnson & Johnson, is set to be approved by the EU on March 8 “if everything goes well,” according to Spanish Health Minister Carolina Darias. The vaccine candidate is in the last stage of its clinical trial. If it is given the green light by the EU, which authorized all previous candidates – the vaccine from Oxford-AstraZeneca, Moderna and Pfizer-BioNTech – it will be approved a few days later by the European Medicines Agency (EMA). In the United States, the Food and Drug Administration (FDA) will review the drug for emergency use on February 26.
The vaccine from Janssen, known as Ad26.COV2-S, has many advantages, principally that it only requires one dose. This means that the 400 million doses committed to the European Union (200 million with the option of an additional 200 million) would allow many people to be vaccinated. Under the EU deal, Spain would receive more than 40 million doses of the vaccine.

Another advantage is that it can last three months at a conventional cooler temperature, without needing to be frozen, and two years below 0ºC. This is thanks to technology similar to that used by the AstraZeneca vaccine, which also does not require ultra-cold temperatures. Another positive is that it is being trialed by around 100,000 volunteers in several countries, including Spain. This includes volunteers from the Phase 3 ENSEMBLE trial, which is testing the vaccine as a one-dose treatment, and another study of the drug as a two-dose inoculation. What’s more, a third of the nearly 50,000 participants in the ENSEMBLE investigation are over the age of 65. This means the vaccine candidate will not face the same problems as the AstraZeneca vaccine, which has been restricted to people between the age of 18 and 55 in Spain, given that there is not yet sufficient evidence of its efficiency for the older age group.
The most recent results from the one-dose clinical trial show that the Janssen vaccine is 66% effective at preventing moderate to severe cases, and 85% effective at preventing critical Covid-19. The first figure is lower as the study included thousands of volunteers from South Africa. All signs indicate that the new strain of the coronavirus identified in South Africa is more resistant to the vaccine.
“You can’t compare rates of effectiveness of different vaccines,” says Alberto Borobia, the doctor coordinating the Janssen clinical trial at La Paz hospital in Madrid. Several factors influence this figure, such as the design of the experiment, the size of the sample and the characteristics of the volunteers involved. The ENSEMBLE research study, for example, is designed to measure how well the vaccine protects people against moderate to serious cases of Covid-19, while other vaccine trials also included minor and asymptomatic cases.
La Paz is one of eight Spanish hospitals participating in the ENSEMBLE 2 trial, which is testing the Janssen vaccine as a two-dose treatment. They do not have any results yet, as they only started recruiting the 30,000 volunteers needed in January. According to Borobia, of this figure, “30% are over the age of 65.” The volunteers will be monitored weekly based on their symptoms, as was the case for the previous stage of the trial. Borobia is confident the study will be able to analyze the impact of the new variants of the coronavirus, although this will depend on the incidence of the mutations in the population.
The last advantage of the Ad26.COV2-S vaccine, at least for Spain, is that most of the doses will be made by the Catalan pharmaceutical company Reig Jofre. This laboratory will receive the antigen and be tasked with producing and bottling it. Reig Jofre says that they are able to make 250 million doses a year, potentially making the problem of vaccine shortages a thing of the past.
Novavax
Spain will also produce the vaccine from US company Novavax, which is due to be approved by the EU. Although the contract between Novavax and the EU has not yet been signed, an EU official told the news service Reuters: “Talks with Novavax have intensified and we aim to agree the contract this week or next.” In principle, Novavax could deliver 100 million doses to the EU, with the option of 100 million more. The EMA is reviewing the results of the Novavax vaccine trial as they are released with a view to potentially authorizing the drug in April.
According to data from the company’s study in the United Kingdom, the two-shot vaccine has an effectiveness rate of 89%. This is in a sample where half of those infected had contracted the new, more-contagious strain of the virus detected in Britain. In a parallel trial in South Africa, the rate of effectiveness fell to 60%, confirming the danger presented by this variant.
The Novavax vaccine works differently from the other vaccines that have been approved. The Pfizer and Moderna vaccines, for example, employ messenger RNA, which teaches cells to produce the spike protein of the SARS-CoV-2 virus. The Novavax inoculation, in contrast, uses a lab-made version of the protein that carries a new adjuvant, called Matrix-M, which kick-starts the body’s immune response.
“The antigen – the element that generates an immune response in the human body – is made in insect cells. To do this, the virus is transformed into one that is only able to infect insects,” explains Andrés Fernández, the managing director of Zendal group, which is based in Spain’s northwestern Galicia region.
The Zendal group owns the biotech company Biofabri, which has been creating the antigen of the Novavax vaccine for weeks. This is done by inserting the virus into moth cells. When they have been infected, the virus is deactivated and the protein that provides protection is extracted. The company is making 1,000 liters of the antigen a week at its laboratory in O Porriño in Pontevedra province.
CureVac
Another vaccine should arrive after summer. This one is created by the German biotech company CureVac. The agreement with the EU stipulates that CureVac will deliver at least 405 million doses of the vaccine, of which 10% will go to Spain. CureVac is also undergoing a clinical trial in Spain.
The study began a few days ago at the Biocruces and Donostia hospitals in Spain’s Basque Country and the Clínico San Carlos hospital in Madrid. Some 30,000 Spanish volunteers are taking part in the investigation, which is part of a broader global trial. Antonio Portolés, the lead researcher at Clínico San Carlos hospital, told Spanish news agency EFE when the trial began that the study was “looking to test the immunogenicity of the vaccine” against Covid to see whether “it is possible to completely neutralize the virus and for those vaccinated not to spread the disease once they are immunized.”
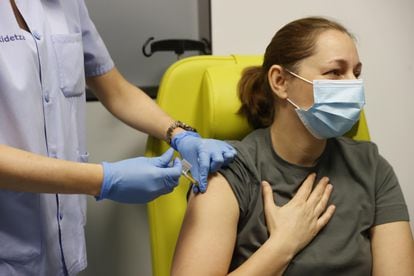
The CureVac vaccine uses the same method made famous by the Moderna and Pfizer vaccine, the RNA messenger. Of the 242 vaccines monitored by the World Health Organization, 63 are in human trials and 11% use the RNA messenger to stimulate an immune response. But of the vaccines approved, counting CureVac, 50% use this technology.
“They are easier to make and produce,” explains Felipe García, the coordinator of a separate vaccination project at Barcelona’s Clínic hospital and Biomedical Research Institute (IDIBAPS). “It takes just a few weeks from when we have the sequence of the virus to when we create the vaccine. No other technology allows this.” García is also using the RNA messenger for the vaccine he is investigating, which is still at the preclinical stage. But he is following the CureVac trials closely. “The particle that protects the RNA messenger is different to that of Moderna or Pfizer,” he says, explaining that this vaccine will have an advantage over the others if the RNA messenger is protected until it enters the cells.
For García, although other vaccines – such as those developed by Spanish companies – may arrive late to the game, the technology that is available in Spain will still be key. He argues that the country has the technological flexibility to develop new defenses against a possible viral threat, not in a year – which is an achievement of itself – but “in months or even weeks.” García also points out that there are growing indications that “we have to vaccinate against the coronavirus every year, like the flu.”
Europe’s offensive against the coronavirus doesn’t end there. The EMA has reviewed the legal and regulatory aspects of various vaccine candidates from Asia, most of which come from China. But up until now, they have not shown interest in being approved in Europe. The makers of the Russian vaccine, Sputnik V, which has already been distributed en masse to other regions of the world, have, however, expressed interest in being authorized by the EU, according to European health officials.
But the more likely arrival, with no set date, is a vaccine from the French company Valneva. This vaccine uses an inactivated SARS-CoV-2 virus, which is the most traditional vaccination method. “Our vaccine is as of today the only inactivated candidate in clinical trials against Covid in Europe,” says Juan Carlos Jaramillo, the chief doctor of Valneva. In January, the company announced that its talks with the EU about delivering 60 million doses were at an advanced stage. Another weapon in the arsenal against Covid-19.
English version by Melissa Kitson.

/cloudfront-eu-central-1.images.arcpublishing.com/prisa/BUDCLNN3TMNNWVPLEDPKPPDLWY.jpg)
/cloudfront-eu-central-1.images.arcpublishing.com/prisa/W7GEBMEA3FA4RBMJZWRG72BAEU.aspx)